CMS Report: ~410K of those kicked off of Medicaid enrolled in #ACA exchange plans or BHPs thru June
Last month, Amy Lotven of Inside Health Policy found an excellent scoop from a new CMS report hiding in plain sight:
New CMS data, quietly released in late August, show about 178,000 consumers chose a qualified health plan (QHP) through a state or federal exchanges after losing Medicaid and CHIP coverage in the first two months of the Medicaid unwinding. Those sign-ups through the end of May are more than three times the 54,000 enrollments that CMS reported in July, which reflected only the April numbers.
As a reminder: Normally, states will review (or "redetermine") whether people enrolled in Medicaid or the CHIP program are still eligible to be covered by it on a monthly (or in some cases, quarterly, I believe) basis. However, the federal Families First Coronavirus Response Act (FFCRA), passed by Congress at the start of the COVID-19 pandemic in March 2020, included a provision requiring state Medicaid programs to keep people enrolled through the end of the Public Health Emergency (PHE). In return, states received higher federal funding to the tune of billions of dollars.
As a result, there are tens of millions of Medicaid/CHIP enrollees who didn't have their eligibility status redetermined for as long as three years.
With the end of this continuous coverage as of March 31st, 2023, healthcare advocates have been warning that millions of people would lose coverage, including many who are still actually eligible...and sure enough, as of this week, at least 7.9 million Medicaid enrollees have lost coverage so far, of whom a stunning 73% (5.75 million) were kicked off the program for purely procedural reasons--that is, failure to return a form or, in some cases, state administrations either mistakenly or deliberately sweeping entire families off the programs if a single member is no longer eligible.
The 178K figure only ran through the end of May, however. Recently the HHS Dept. posted a new report which updates the data through the end of June:
- For HC.gov, across 32 states (Oregon is missing), ~436K people who were kicked off of Medicaid/CHIP applied for ACA exchange coverage
- Of those, ~52.6K (12%) were determined by HC.gov to still be eligible for Medicaid/CHIP and presumably were re-enrolled
- The remaining ~383K (88%) were determined by HC.gov to be eligible for an ACA exchange Qualified Health Plan (QHP), with or without subsidies
- 337.2K receive subsidies; 45.5K don't
- Of those, ~291K (67% of the total who applied) actually enrolled in a QHP
The state-based exchange report is laid out little differently, but out of ~594K who applied, 414.5K were determined to be eligible for a QHP (70%); of those, only 63K actually enrolled in one, plus another 55.8K who enrolled in a BHP.
Across all states, that's 354,361 who actually enrolled in a QHP through the end of June, plus the BHP enrollees for a total of 410,138 total.
Overall, that's roughly 40% of the 1,029,856 people who applied for ACA marketplace coverage through June. Another 52.6K were determined to still be Medicaid/CHIP eligible, leaving 567K (~55%) who had to find some other type of coverage.
It's also important to note that this obviously does not mean that only ~1.0 million Americans had lost Medicaid/CHIP coverage through the end of June. Aside from Oregon missing, it also only includes those who actually applied for coverage to begin with. The KFF Medicaid Unwinding Tracker put the total number of Americans who had lost Medicaid/CHIP coverage as of July 19th at over 3.09 million. The dates don't match up, but it's also likely that the actual figure as of July 19th was higher than that; assuming those cancel each other out, this suggests that perhaps 13% of those who had lost Medicaid/CHIP enrolled in ACA exchange plans or QHPs.
If you further extrapolate that out to the 7.9 million who have lost Medicaid/CHIP coverage as of October 2nd, it would mean slightly over 1.0 million have enrolled in QHPs/BHPs, although this is still speculative.
It may seem surprising at first that there are more people in state-based exchange states who lost coverage given that only 40% of the total U.S. population lives in those states, but note that Oregon is missing from the HC.gov data. Also keep in mind that all of the state-based exchange states have expanded Medicaid under the ACA, while 10 of the HC.gov states haven't done so (including huge states like Texas and Florida), meaning they generally had a higher portion of their residents in Medicaid/CHIP in the first place.
There's also still a strange disconnect between the ratios of HC.gov and SBM states here: 67% of HC.gov applicants enrolled in QHPs, while only 20% of SBM applicants enrolled in either QHPs or BHPs. Huh.
I'll post an update once I've had a chance to dig into the data in more detail.
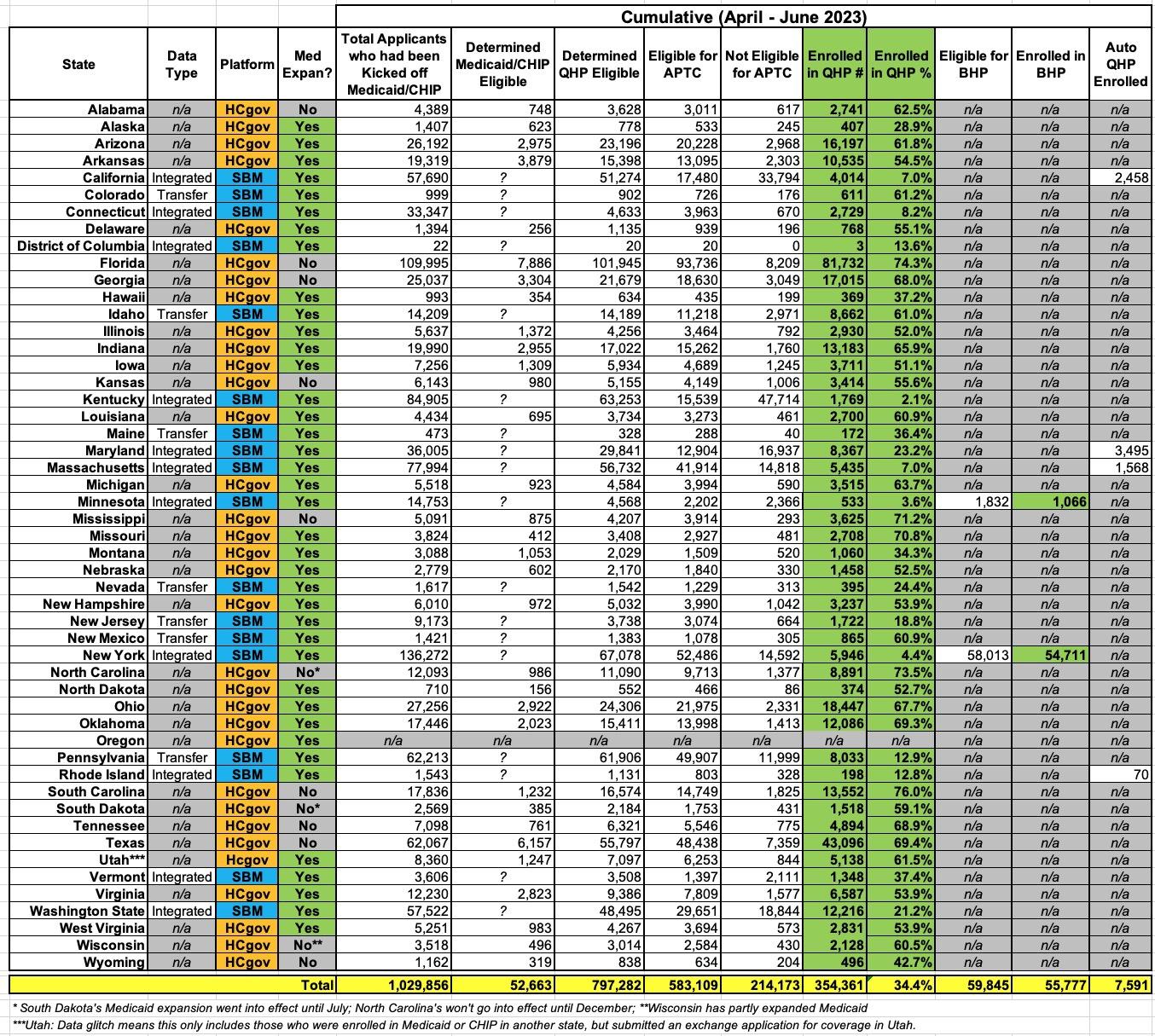
UPDATE: I've reformatted most of the relevant data into a simplified, easier-to-follow spreadsheet with all 49 states +DC (again, Oregon is missing). Some key takeaways:
- 7,600 people in 4 states (CA, MD, MA & RI) which have this capability have been automatically transferred from Medicaid/CHIP over to ACA exchange plans.
- Nationally, around 34.4% of the Unwinding population who applied for coverage via their ACA exchange have actually enrolled in a QHP, plus another 5.4% in MN/NY who enrolled in BHP plans
- The percentage ranges widely, from as little as 2.1% in Kenucky to as much as 76% in South Carolina.
- Only 73% of those determined eligible for QHPs were also deemed eligible for APTC subsidies. This is noteworthy because it's significantly lower than the 90.5% of all ACA exchange enrollees who are receiving subsidies. It suggests that either a disproportionately high portion of the Unwinding population is higher income or that those most likely to actually apply in the first place are higher income, which is rather counterintuitive. Unfortunately the report doesn't break out the APTC/no APTC numbers of those who actually enrolled in QHPs, however.