Six years later, the Final Chapter of the #RiskCorridorMassacre saga concludes (updated)
I've written at least a dozen explainers about what I've termed the Risk Corridor Massacre over the past five years, starting with this one from 2015, and I pray to God that this is the last time I have to do so. Here we go:
- The Affordable Care Act made massive changes to many parts of the U.S. healthcare system, but by far the most radical changes were made to the individual, or "non-group" market. This is health insurance for people who aren't covered by Medicare or Medicaid but who also don't have coverage through their employer (or who are self-employed, as I am).
- Before the ACA, individual market carriers could cherry-pick their enrollees, either denying coverage to those with pre-existing conditions, covering them but charging massively higher rates for doing so, or covering them but exempting themselves from coverage of the very conditions which were most in need of treatment.
- Starting in 2014, the ACA no longer allowed this; insurance carriers were required to offer the same insurance policies to everyone regardless of their health status, medical history, gender, age, occupation, hobbies and so forth. Furthermore, those policies had to cover the same services/treatments regardless of those factors...and finally, the price of a given policy could only vary based on three things: Where the enrollee lives; how old they are (within a 3:1 range); and whether they smoke or not (in most states).
- Because of this complete overhaul of how health insurers estimated their costs and revenue, which was bound to cause things to be pretty rough for awhile, the ACA included three stabilization programs to help smooth things out. Two of them were time-limited "training wheels" ("Reinsurance" and "Risk Corridors", which were only to be in place for three years, from 2014 - 2016); the third is permanent ("Risk Adjustment").
- The ACA's federal Reinsurance program, as far as I know, worked pretty well when it was in place to help mitigate the cost of extremely expensive-to-treat enrollees...but it was sunsetted at the end of 2016. Since then, over a dozen states have reinstated their own version of a reinsurance program using a provision of the ACA called a Section 1332 Waiver. In some cases these new state-level programs are actually more generous than the original federal one was. If you want a deep dive into reinsurance, read this.
- The ACA's Risk Adjustment program is long-term, and is the one I'm the least familiar with of the three; read this for a better explanation of how it works.
- Finally, there's the 3-year ACA Risk Corridor program. The basic idea of Risk Corridors is to help protect insurnace carriers from facing massive losses by limiting their downside risk...with the tradeoff being that they also have their potential profits limited as well.
Here's a summary of how it was supposed to work from The Commonwealth Fund:
Because the ACA marketplaces are so new and the health risks of new enrollees uncertain, some insurance companies could make a windfall or lose their shirts in the early years of the rollout. This could encourage companies to set premiums higher than necessary just to make sure they aren’t among the losers.
To prevent this, the federal government has created a program under which it will collect money from plans sold in the new marketplaces with unexpectedly high gains and redistribute them to plans with unexpectedly high losses. If plans make or lose up to 3 percent more than expected, they keep the gains or eat the losses. However, if they make or lose 3 percent to 8 percent more than predicted, they give up 50 percent of the winnings or are compensated for 50 percent of their shortfalls above 3 percent. If losses or gains exceed 8 percent, the insurers give up or get back 80 percent of gains or losses exceeding 8 percent of the predicted amount. If the government collects more from winners than it has to pay out to losers, it keeps the balance.
In other words, for three years--2014, 2015 & 2016--let's say that an insurance carrier made a 10% profit on $1 billion in revenue ($100 million). Under the RC program, they'd have to pay $41 million into the federal kitty (50% of $50 million + 80% of $20 million). If another carrier took a 10% loss for those years (again, assuming the exact same $1 billion in revenue), they'd be entitled to be paid $41 million from the federal kitty.
Again, the idea was that the carriers would be effectively throwing darts blindfolded and thus would take a few years to figure out and adjust to the new realities of the individual policy marketplace.
Obviously the carriers would be all over the place in terms of revenues, profits, losses, percentages and so forth. At the time that the Commonwealth Fund explainer was written, there was some confidence that the federal government might actually end up profiting off the deal--if there were more winners than losers, anything extra would go to the feds. Of course, the flip side was that if there were more losers than winners--that is, if more money had to be paid out than came in--the feds would have to eat the loss.
It was a calculated gamble, but a reasonable one...especially since a similar Risk Corridor program had been quietly working pretty well for the Medicare Part D program for many years without anyone raising a fuss.
Unfortunately, with the ACA, everything causes a fuss, and so began the first chapter of what I've dubbed the Risk Corridor Massacre.
In November 2013, in the middle of the first Open Enrollment Period, Republican Senator Marco Rubio of Florida introduced a bill to completely eliminate the Risk Corridor program before it even went into effect. Keep in mind that he introduced this after the 2014 policies had already been locked into place and just weeks before the first ACA-compliant policies were set to go into effect.
Rubio's bill to wipe out the RC program didn't make the cut in 2013, but in late 2014, a modified version was included in the "must-pass" Continuing Resolution Omnibus bill ("CRomnibus") which accomplished something similar: It didn't destroy the program, but it did change it so that it had to be revenue-neutral to the federal government. What this meant in practice is that the only money which could be paid out to the "losers" was that which came from the money coming in from the "winners". If there were more winners than losers, this would be a moot point...but if there were more losers than winners, there wouldn't be enough money in the kitty to pay them their full share.
I should note, by the way, that while Marco Rubio tried hogging all the "credit" for this "victory", it was actually three other Republicans who pushed it through: Then-Senator Jeff Sessions, Rep. Fred Upton and then-Rep. Jack Kingston. However, since he's the one who insisted on bragging rights for this stupid, pointless stunt, I'm more than happy to give him full credit. Besides, neither Sessions nor Kingston are in office anymore.
Anyway, it wasn't until October of 2015 that the final report was issued on individual market performance for 2014, and when it did, the news wasn't pretty:
Today, HHS is announcing proration results for 2014 risk corridors payments. Based on current data from QHP issuers’ risk corridors submissions, issuers will pay $362 million in risk corridors charges, and have submitted for $2.87 billion in risk corridors payments for 2014. At this time, assuming full collections of risk corridors charges, this will result in a proration rate of 12.6 percent.
In other words, $2.9 billion was owed to some carriers but only $362 million had come in from the other carriers, meaning the federal government could only pay the losers 13 cents on the dollar. Ouch.
The amount of carnage this caused--especially with the news breaking just a few weeks before the launch of the 2016 Open Enrollment Period--can't be overstated. Every week, and in some cases every few days, I had to write an obiturary for another small start-up insurance carrier. Most of these were, as it happens, created by the ACA as public/private non-profit Co-Operatives, but it also included a few pre-existing (no pun intended) private carriers such as WINHealth in Wyoming.
To be fair, many of the Co-Ops had other problems besides the lost Risk Corridor payments; as Adam Cancryn laid out in his fantastic, definitive autopsy report, the co-ops were effectively designed to fail from the start. Frankly, what's surprising isn't that so many of them failed but that a handful of them have managed to still survive past those ugly initial years (there's just three left in Maine, Wisconsin and Idaho/Montana). Still, having the RC payments cut off at a critical time was the final blow in many cases; several of those co-ops would likely have survived otherwise.
There was a desperate hope that things might turn around in 2015 or 2016, allowing carriers to recoup their losses from 2014 as well...but it wasn't meant to be: The 2nd and 3rd year of the ACA saw even larger losses for most carriers, for a cumulative net total federal I.O.U. of over $12 billion.
In the end, over 800,000 people were forced to find new healthcare coverage in large part due to Rubio's stunt, which I presume was mostly done to boost his budget hawk cred for his impending (and doomend) Presidential campaign. As ACA expert & law professor Nicholas Bagley noted at the time, the whole thing was done for show, not out of "fiscal conservatism", because the odds were that the insurance carriers would eventually be paid the money legally owed to them anyway.
Furthermore, as my colleague David Anderson noted at the time:
...Anywhere where a closed insurer was the issuer of the second least expensive Silver (the benchmark plan) or the cheapest silver, the Federal government will pay more in Advanced Premium Tax Credits. The new benchmark plan is either the former #3 Silver or #4 Silver plan. The gap between the personal contribution and the new benchmark plan is now wider than it would have been. Over the long run, there are fewer competitors and more importantly, fewer competitors who are mainly concerned about the Exchange market and thus can offer low provider reimbursement level products (with attendant skinny networks).
So the Rubio rider causes a lot of chaos, does not actually solve the problem it is superficially intended to solve, costs the government more money in the short term as the benchmarks are recalculated upwards, and costs the government more money in the long term as there are fewer insurers and thus less competition. The big winners are Rubio (as he gets to fundraise and preen off of it) and incumbent insurers that have large cash reserves.
Brilliant!
Let's skip a few years to June 2018. Lawsuits had indeed been brought by the insurance carriers (or by creditors for the now-defunct ones which went belly-up), and while Bagley had assumed they had an open-and-shut case, after winning in the early stages, a lower court actually ruled against them. Bagley was shocked:
..Even as congressional Republicans kicked up a kerfuffle over “bailouts,” HHS was reassuring insurers that the agency would “record risk corridors payments due as an obligation of the United States Government for which full payment is required.” Knowing full well that it had an obligation to pay, Congress shut off the funding stream in a deliberate effort to sabotage the ACA.
And it worked! Loads of co-ops went under in response to the unexpected financial hit. Did Republicans in Congress care that they were reneging on a promise? Not a bit. They saw a chance to hurt Obamacare, and they took it.
...I’m again at a bit of a loss. You don’t have to use magic words to enter into a contract. You just have to make a promise.
...From there, it’s on to the Supreme Court. Who knows if it’ll agree to hear the case? It’s not an implausible candidate for review, and lord knows the Court can afford to take more cases. But the Court might be gun-shy about wading into another case about the ACA.
So this isn’t the end of the road for insurers. But it’s a Michigan-sized pothole in that road. And the opinion reflects a disturbing unwillingness to hold the government accountable for its promises. That’s a point Judge Newman made in concluding her dissent.
However, there was another twist almost exactly a year later:
Big news: SCOTUS is taking up the ACA risk corridors case. GOP's decision to stymie that program arguably did the most damage to the ACA marketplaces.
— Bob Herman (@bobjherman) June 24, 2019
And sure enough, in April of this year...
A big Obamacare decision from SCOTUS this morning: The court rules 8–1 that insurers who lost money under the Risk Corridors program have a right to payment from the government AND damages for unpaid amounts.
— Mark Joseph Stern (@mjs_DC) April 27, 2020
From the actual Supreme Court ruling, the final decision was an easy one, exactly as Bagley had predicted years earlier:
In establishing the temporary Risk Corridors program, Congress created a rare money-mandating obligation requiring the Federal Government to make payments under §1342’s formula. And by failing to appropriate enough sums for payments already owed, Congress did simply that and no more: The appropriation bills neither repealed nor discharged §1342’s unique obligation. Lacking other statutory paths to relief, and absent a Bowen barrier, petitioners may seek to collect payment through a damages action in the Court of Federal Claims.
These holdings reflect a principle as old as the Nation itself: The Government should honor its obligations. Soon after ratification, Alexander Hamilton stressed this insight as a cornerstone of fiscal policy. “States,” he wrote, “who observe their engagements . . . are respected and trusted: while the reverse is the fate of those . . . who pursue an opposite conduct.” Report Relative to a Provision for the Support of Public Credit (Jan. 9, 1790), in 6 Papers of Alexander Hamilton 68 (H. Syrett & J. Cooke eds. 1962). Centuries later, this Court’s case law still concurs.
The judgments of the Court of Appeals are reversed, and the cases are remanded for further proceedings consistent with this opinion.
It is so ordered.
This, in turn, gave dozens of insurance carriers (and, again, some creditors who had bought up whatever legal assets were left of the now-defunct ones) the right to demand payment from the Court of Federal Claims.
And here's where things get really interesting: How would the payments be recorded in the carriers books?
What I mean is this: Some payments are recorded on a "cash basis"...that is, if a client owed you money in 2019 but doesn't actually pay you until 2020, "cash basis" means you record it as being part of your 2020 revenue. Others are recorded on an "accural basis"...you would backdate the payment to be part of your 2019 revenue since that's when it was actually owed.
$12 billion is an awfully big past-due invoice, and how it gets recorded would have some pretty big implications for all sorts of reasons for any business...but for health insurance carriers, it's even bigger:
OK, so if SCOTUS rules in favor of the carriers (and they absolutely should...regardless of what you think of health insurance companies, the fact remains that they are contractually owed this money by the U.S. Government), most of the carriers will get paid what they were originally owed, and whatever firms now own the assets of the carriers which went belly-up will finally get a return on their investment. Big deal for the rest of us, right?
Well, yes...except that there's more to the story, and it involves, once again, the beauty which is the ACA's Medical Loss Ratio rule.
Again, under the Affordable Care Act, insurance carriers on the individual market are required to spend at least 80 of their premium revenue on actual medical claims. If they spend less than 80% over a rolling three-year period average, they have to pay back the difference to the policyholders.
I wrote about this extensively in my big MLR Rebate Project a few months ago, which analyzed not only the record-breaking actual 2018 MLR payments ($770 million nationally) which went out in September, but also made projections as to the potential 2019 MLR rebates which will go out a year from now. My conclusion was that the 2019 payments (going out in 2020) could end up being double this years' due to the overpricing for the 2017 & 2018 plan years being fully baked in (potentially up to $2.0 billion total).
Sure enough, the actual total amount which individual market carriers have had to pay out to policyholders in the form of MLR rebates over the past month or so have totalled almost exctly...$2.0 billion.
So what's this have to do with the Risk Corridor lawsuit settlement? Simple: If the payments are recorded on an accrual basis, that means the insurance carriers will have to dig up their financial records for 2014, 2015 and 2016, record their payments for those respective years, and then re-file their MLR paperwork for those years.
If the carrier only made, say, a 10% gross margin for the year (a 90% MLR) and the cash infusion only drops this down to, say, 85% MLR, then it also doesn't mean much; they're still over the 80% threshold so no MLR rebates would have to be paid out.
However, if they were hovering just over the 80% line and the RC settlement drops them below it (from 82% to 78% or whatever), then they'll have to pay a chunk of it out...and in cases where they already came in below 80%, they may have to turn right around and pay all of the settlement amount right back out to their policyholders in the form of MLR rebates!
It's important to keep in mind that even in 2016, the worst year for ACA market profitability, 54 carriers still had to pay out $103 million to around 904,000 individual market enrollees. I assume another hundred or so were just barely above the 80% MLR threshold. Keep in mind that the 80% figure is based on a 3-year rolling average, so a carrier which does terribly one year could still owe money due to having done great the previous two years.
OK, but what about if the RC settlement is recorded on a cash basis? That means that it's recorded in the year the revenue is received...which presumably means this year, 2020 (or possibly 2021...I'm not sure how long it'll actually take for the payments to be made).
If that happens, then holy cow...because the carriers are doing very well (for the most part) these days, and a lot more of them have had to shell out MLR rebates. As noted above, nearly $2 BILLION is being paid out this year.
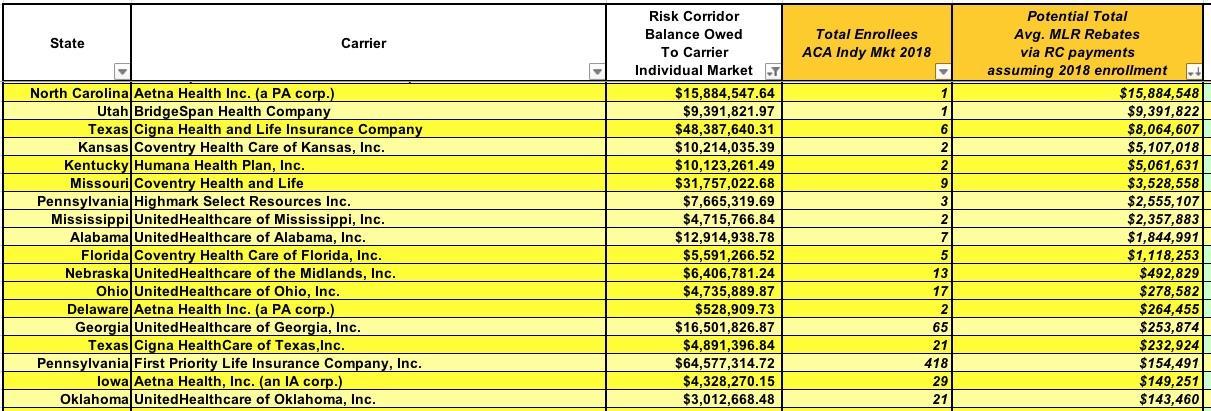
I did a lengthy write-up about this possibility last year, and another one this year in which I actually listed every single carrier which is owed Risk Corridor payments (there's also money owed to Small Group carriers, but that's only around $1.4 billion of the total and their MLR rebates tend to be a lot more stable year to year anyway). A total of 345 individual market carriers are owed around $10.9 billion.
I concluded at the time that assuming the RC payments are recorded on a cash basis, and assuming that these carriers come in at 80% MLR or lower this year (not all of them will), and assuming that they have the exact same number of enrollees this year that they did in 2018 (highly unlikely; most will be higher or lower), then it was conceivable that a small number of individuals could see some massive MLR rebate checks showing up over the next few years:
That's right: If the RC payments are recorded on a cash basis, it'd be hypothetically possible that a single enrollee in North Carolina could end up receiving an MLR rebate check for nearly $16 million...when they presumably only paid a few thousand dollars in actual premiums for the year.
As it happens, however, for good or for bad, this latter batcrap scenario wasn't meant to be:
Date: September 30, 2020
From: Samara Lorenz, Director, Oversight Group, Center for Consumer Information & Insurance Oversight
Title: Draft Insurance Standards Bulletin Series – INFORMATION
Subject: Treatment of Risk Corridors Recovery Payments in the Medical Loss Ratio and Rebate Calculations
...Under section 2718 of the PHS Act, an issuer’s MLR and rebate calculations must account for, among other things, the net payments or receipts related to the RC program. The purpose of this draft guidance is to describe how issuers must treat the RC payment amounts recovered as a result of the Supreme Court decision in their MLR and rebate calculations. The contents of this document do not have the force and effect of law and are not meant to bind the public in any way, unless specifically incorporated into a contract. This document is intended only to provide clarity regarding existing requirements under the law.
...We propose the following instructions to guide the reporting of the recovered RC payment amounts and the issuance of additional rebates.
Issuers must submit a revised MLR reporting form(s) for the 2015 through 2018 reporting years for each state, market, and year in which the issuer has a greater rebate liability based on inclusion of the recovered RC payment amounts. Issuers must pay the outstanding rebate amounts to the enrollees who were enrolled in the respective MLR reporting year. Issuers that do not have a higher rebate obligation based on the inclusion of the recovered RC payment amounts for any of the applicable reporting years do not need to submit a revised MLR reporting form.
Issuers must revise their MLR and rebate calculations and pay the additional rebate amounts based on the full calculated RC payment amount, even if the issuer sold their rights to receive all or a portion of its recovered RC payment amounts to a third party. If an issuer has been acquired by a new company and the ceding issuer’s rebate obligation based on the inclusion of recovered RC payment amounts is higher than the rebate amount paid in the respective reporting year, the assuming company is responsible for submitting the revised prior year MLR reporting forms(s) and paying the additional rebate amount to the ceding entity’s enrollees in the respective MLR reporting year(s).
Timing of Submission of the Revised Prior Year MLR Annual Reporting Form(s)
Issuers with a higher rebate obligation based on the inclusion of the recovered RC payment amounts for one or more of the applicable prior reporting years must submit the revised reporting forms to CMS by December 31, 2020, or within 60 days of receiving additional RC payments, whichever is later. Affected issuers should contact CMS at MLRQuestions@cms.hhs.gov for instructions on how to submit the applicable prior year reporting forms in the CMS Health Insurance Oversight System (HIOS).
Timing of the Disbursement of Additional Rebates
Issuers must disburse additional rebate payments to enrollees in the respective year within 60 days of submitting their revised MLR reporting forms to CMS. If an issuer fails to pay the additional rebates by the required deadline, rebate payments must then include late payment interest amounts at the Federal Reserve Board lending rate or ten percent annually, whichever is higher, on the total amount of the additional rebate, accruing from the date on which the additional rebate was due as outlined in this guidance.
Put more simply, it looks like insurance carriers are being told to record the Risk Corridor payments on an accrual basis after all...although the bit at the beginning about it "not having the force of law" is a bit confusing. On the other hand, I'm pretty sure practically every carrier would prefer to record it that way, since if they did it on a cash basis they'd be a lot more likely to have to pay most (or even all) of it back out to policyholders anyway.
On the other other hand, this presumably also means a massive amount of overtime for accountants, actuaries and lawyers as they painstakingly go through their records from up to six years ago to calculate exactly how much they have to pay out to everyone who was enrolled in one of their individual market policies that year. Then they'll have to cut a check and mail it to people who may have moved or died in the four, five or six years which have passed.
So, just how much of that $12.3 billion (again, $10.9 million on the indy market, $1.4 billion on the small group market) will actually have to be paid out in the form of MLR payments now that we know how it's being recorded?
Well, according to actuarial accounting firm Wakely...around $298 million:
...CMS (Centers for Medicare & Medicaid Services), through the published guidance, proposed that issuers that receive risk corridor payments should refile their MLR reports for 2015 through 2018. Additionally, if the updated MLR calculations for the individual and small group market exceed the MLR threshold, then issuers must make the additional rebate payments. Rebates must be made regardless of whether the issuer is still active or owned by a new controlling entity. The additional MLR rebates must be paid out by December 31, 2020, or within 60 days of receiving additional RC payments.
...Based on our findings, Wakely estimates that approximately $298 million (or 2.4% of total additional RC recovery payments) additional MLR rebates will be distributed as a result of the adjustment to the 2015-2018 MLR filings due to retroactive RC payments.
Again, not every carrier is entitled to a chunk of the Risk Corridor payments in the first place. According to the Wakely analysis, of the $2.02 billion paid out in MLR rebates by all individual & small group carriers from 2015 - 2018, only about a quarter of it came from carriers which are owed RC payments:
Issuers set to receive the remaining RC payments paid a total of $578 million of MLR rebates to consumers between 2015 and 2018. Those same issuers are estimated to pay out an additional $298 million in rebates as a result of the additional RC recovery payments, increasing the total rebate paid for these issuers by roughly 52%
The other $12.0 billion will end up pocketed by the individual and small group market carriers...although again, in a couple dozen cases it'll go to whoever acquired their assets. In some cases the carriers have long since sold off the rights to RC payments to a third party hedge fund or whatever...although Wakely says that over 99% of the total will go to insurance carriers which are still offering policies today ($297 million out of the $298 million total).
Most of the issuers (or entities) receiving payments were still actively offering coverage to new enrollees as of 2019. Using CMS’ 2019 risk adjustment report, we identified issuers that were still active in 2019 and issuers that were no longer actively offering new coverage in their respective market.
As Anderson notes:
One way of looking at this is that this is a massive distribution of hookers and blow.
The other way to look at it is that insurers lost billions from 2014-2016 and the RC payments still have them, on net, still losing billions but just not as many.
Unfortunately, the Wakely report doesn't list the actual carriers which will owe rebates; in order to do that, I'd have to go back to the 2015, 2016 & 2017 MLR reports and compare each carrier's data to the amount they're owed, which would be a royal pain.
And so, in the end, Marco Rubio's Risk Corridor Massacre ended up pretty much exactly as Bagley, Anderson and I predicted in the first place years ago:
- 800,000 people nationally lost their insurance coverage, on very short notice, and were forced to scramble to find alternate coverage,
- the new coverage these people ended up with is generally more expensive, and in many cases had worse networks,
- the federal government had to therefore pay out more in premium subsidies to cover the increased costs as benchmark plans were increased,
- over a dozen insurance carriers went out of business, meaning hundreds of people lost their jobs,
- the loss of over a dozen carriers meant less competition in those markets, therefore higher premiums, therefore even more cost to the federal government in subsidies to make up the difference
- since all of the carriers which went out of business were little guys, this also means the big kahunas sucked up even more market share, and...
- the original $12.3 billion which Rubio was supposedly trying to "save" taxpayers ends up being paid out anyway...
- ...all just to make Marco Rubio look good for his 2016 Presidential campaign...which ended up failing miserably anyway.
Bravo, Senator Rubio. Nicely done.
UPDATE: Since I posted this I've learned two more surreal little tidbits about the CMS Risk Corridor Settlement Handling guidance:
- First: There are some carriers which are still operating but which sold off their Risk Corridor receivables to a third party years ago for a fraction of the total owed; this gave them an immediate cash injection while leaving the hassle of actually following up on the lawsuit/etc with someone else. In those cases, the third party gets the payment...but the carrier still has to refile their MLR paperwork as if they had received the full RC payment.
In other words, let's suppose Blue Cross Blue Shield of West Dakota was owed $50 million, but sold that IOU off to a hedge fund for $10 million. The hedge fund's investment eventually pays off as they get the full $50 million..but BCBSWD is stuck refiling their 2015 - 2018 MLR forms as if they had received all $50 million...and if doing so puts them below the 80% MLR threshold, they could end up having to pay out millions of dollars in MLR rebates anyway. It's even theoretically possilbe that they'd have to pay out more than $10 million, meaning they'd end up taking a net loss while the hedge fund pockets a cool $40 million net profit.
However, any carrier which was so desperate for cash that they were willing to hold such a fire sale probably took such a loss those years that they'd still end up over the 80% threshold even with the RC amount tacked onto their MLR books.
- Second: While the RC payments have to be booked on an accrual basis for MLR purposes, they're entered on a cash basis for federal tax purposes. The corporate tax rate in 2015, 2016 & 2017 was 34%. The corporate tax rate in 2020 is 21%.
If I understand this correctly, this means the insurance carriers will only end up having to pay $2.6 billion of the total right back to the IRS in taxes instead of $4.2 billion...giving them an additional net profit of around $1.6 billion more.