CMS posts claimed December 2025 Medicare data; Advantage enrollment DROPS for first time in at least 12 years (updated)

Medicare Advantage (technically "Medicare Part C" & originally called "Medicare+Choice") is a type of health plan in the United States offered by private companies as part of the original Social Security Act of 1965 that created Medicare. It permits a private insurance option that wraps around traditional Medicare. Medicare Advantage plans attempt to fill some coverage gaps and offer alternative coverage options.
Under Part C, Medicare pays a plan operator a fixed payment for each enrollee. The operator then pays for their medical expenses. Traditional Medicare directly compensates providers on a fee-for-service basis. Plans are offered by integrated health delivery systems, labor unions, non profit charities, and health insurance companies, which may limit enrollment to specific groups of people (such as union members).
Medicare Part C/Advantage only covered around 2.8% of total Medicare enrollment as of 1986, then gradually grew to around 18% by 1999. After that it dropped off before growing again to cover roughly 1 out of 4 Medicare enrollees as of 2010, when the Affordable Care Act was passed. Since then, it has grown to the point that as of a year or so ago it crossed the 50% threshold, making it the default choice of Medicare enrollees.
The Centers for Medicare & Medicaid Services (CMS) just published updated enrollment data for Medicare, adding December 2025 to the data archive.
Whether the data posted since the Trump 2.0 Regime took power is accurate or not, I can't say for certain, but at least they're updating it...and so far, at least, I don't see anything in their monthly reports which is setting off any obvious red flags.
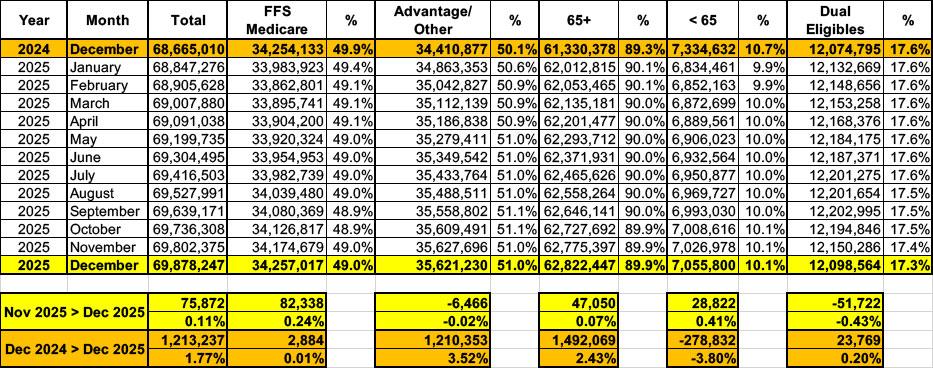
According to the latest report, as of December 2025:
- Total Medicare beneficiaries are up to 69.88 million (up ~76K month over month)
- Traditional/FFM Medicare beneficiaries are at 34.26 million (up ~82K m/m)
- Medicare Advantage beneficiaries dropped slightly to 35.62 million (down ~6.5K m/m)
- 12.10 million Medicare enrollees (17.3% of the total) were "Dual Eligibles"...that is, enrolled in both Medicare and Medicaid.
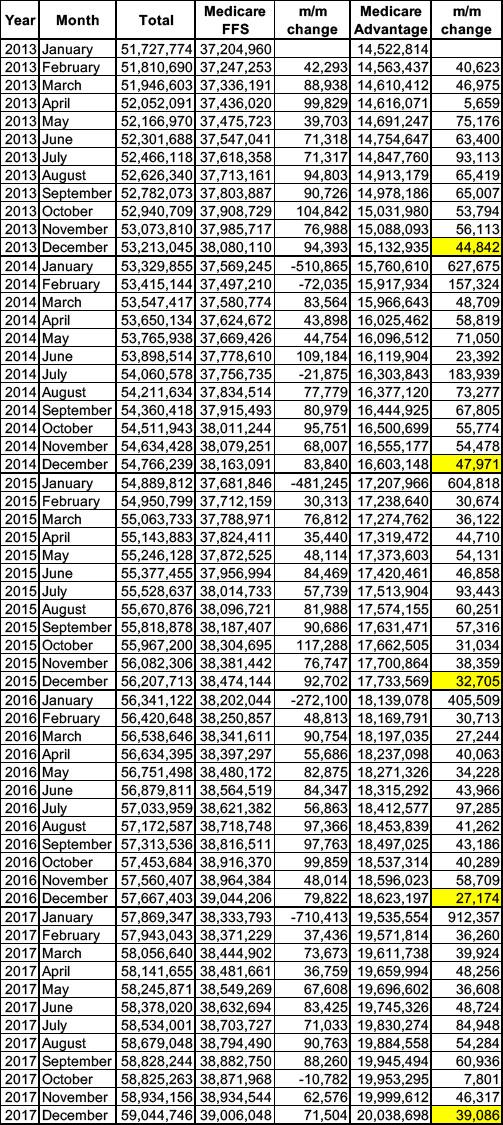
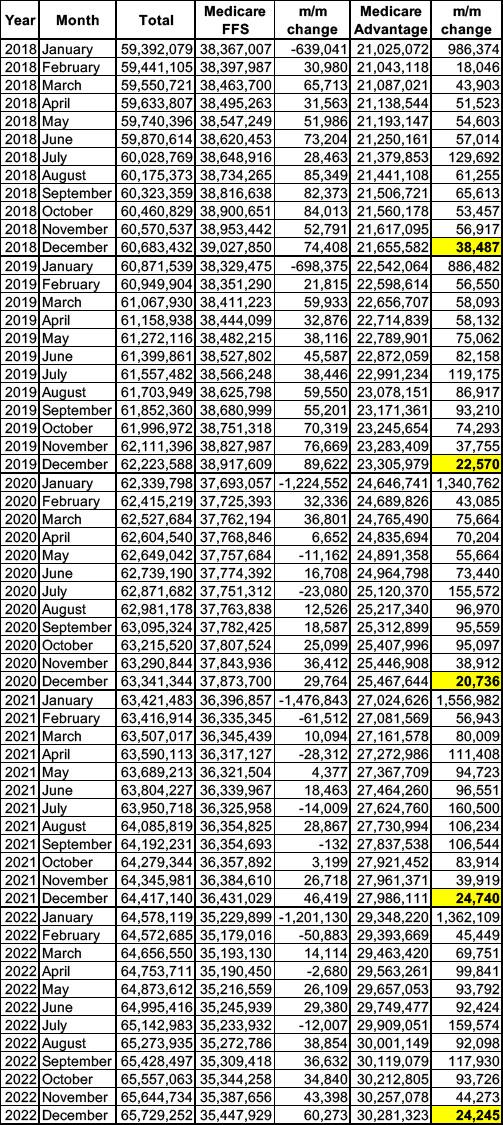
The third bullet above--Medicare Advantage enrollment dropping, even if only slightly--could be a data entry error or a one-time anomaly. If it isn't, however, it's actually hugely important, at least symbolically...because according to the CMS, this is the first time that enrollment in Medicare Advantage plans has dropped month over month since at least 2013:
As you can see above, December usually features the smallest month over month enrollment increase in Med Advantage while January typically features the highest increase...but from at least January 2013 (the earliest month in the CMS database) through November 2025, Advantage enrollment had always increased at least a little each and every month.
Again, this might just be a statistical blip; both enrollment in and market share of Medicare Advantage likely jumped several hundred thousand higher starting January 1st. Regardless, this may be a sign that the popularity of Advantage plans has finally peaked and that the bloom may be finally coming off the rose.
To give you an idea why, here's an article from about a year ago from the Center for Medicare Advocacy:
...On the other hand, there appears to be increased scrutiny of Medicare Advantage by the new administration. Perhaps this is because as Medicare becomes more privatized and more people are in MA plans, overpayments and barriers to accessing care are harder to ignore. For example, CMS announced that it will be expanding its audit efforts for MA plans. In a recent press release, CMS stated that “Beginning immediately, CMS will audit all eligible MA contracts for each payment year in all newly initiated audits and invest additional resources to expedite the completion of audits for payment years 2018 through 2024.” As noted by STAT News in an article by Bob Herman (May 21, 2025), this effort builds on a Biden Administration rule from 2023 that “finalized the structure of these audits — known as risk adjustment data validation, or RADV.”
...The article notes that the “criminal probe adds to a list of government inquiries into the company, including investigations of potential antitrust violations and a civil investigation of its Medicare billing practices, including at its doctors offices.” Noting that DOJ has “struggled to make its case in fraud claims against UnitedHealth in the past”, the article describes a civil case brought by a whistleblower in 2011 and joined by the government in 2017 “concern[ing] claims that UnitedHealth submitted $2 billion worth of diagnoses recorded by doctors that its own reviewers determined weren’t supported by patients’ medical charts.” The reporters state that:
...Now a blockbuster lawsuit filed May 1 by the federal Department of Justice alleges that insurers Aetna, Elevance Health (formerly Anthem), and Humana paid “hundreds of millions of dollars in kickbacks” to large insurance brokerages — eHealth, GoHealth, and SelectQuote. The payments, made from 2016 to at least 2021, were incentives to steer patients into the insurer’s Medicare Advantage plans, the lawsuit alleges, while also discouraging enrollment of potentially more costly disabled beneficiaries.
via the Center for American Progress:
Ending Overpayment in Medicare Advantage: A new Center for American Progress analysis finds that Medicare Advantage (MA) plans are overpaid by 22 to 39 percent; savings from curbing MA overpayments should be used to improve the Medicare program for all beneficiaries.
via the Committee for a Responsible Federal Budget:
Medicare Advantage Will Be Overpaid by $1.2 Trillion: The Medicare Payment Advisory Commission (MedPAC) released their latest status report on the Medicare Advantage (MA) program last week. Based on this information, we estimate that MA will be overpaid by $1.2 trillion between 2025-2034. As MA enrollment continues to grow, policymakers should right-size payments to improve Medicare’s Hospital Insurance (HI) Trust Fund and the programs overall fiscal outlook.
via the Medicare Rights Center:
Watchdog Estimates $7.5 Billion Medicare Advantage Overpayment from “Questionable” Health Risk Assessments
Hidden audits reveal millions in overcharges by Medicare Advantage plans
Newly released federal audits reveal widespread overcharges and other errors in payments to Medicare Advantage health plans, with some plans overbilling the government more than $1,000 per patient a year on average.
Summaries of the 90 audits, which examined billings from 2011 through 2013 and are the most recent reviews completed, were obtained exclusively by KHN through a three-year Freedom of Information Act lawsuit, which was settled in late September.
As for the enrollee's side of things, via Health Affairs:
Medicare Advantage Denies 17 Percent Of Initial Claims; Most Denials Are Reversed, But Provider Payouts Dip 7 Percent
Policy makers have been paying increasing attention to claim denials by Medicare Advantage (MA) plans. For example, the US Senate recently released a detailed report on claim denials in MA,1 and the Centers for Medicare and Medicaid Services (CMS) recently released a proposed rule mandating increased transparency around MA denial criteria.2
The direct impact of denied claims falls primarily on providers, as denials are tied to services that have already been rendered. However, claim denials may have meaningful indirect effects through deterring certain types of utilization.
Medicare Advantage enrollees and their physicians in 2022 saw a larger share of their prior authorization requests denied when compared with previous years, according to a recently released KFF analysis of data that Medicare Advantage insurers submitted to the Centers for Medicare & Medicaid Services (CMS) between 2019 and 2022.
Data from 2022 showed that 7.4% of all prior authorizations were denied or partially denied—for example, the insurer approved 10 of 14 requested therapy sessions. That’s up from the less than 6% of requests denied in each of the years from 2019–2021, says the report from KFF, an independent health policy research, polling and news organization that until last year was known as the Kaiser Family Foundation.
Full prior authorization denials accounted for the majority of denials each year; meanwhile, the proportion that were partial denials became a smaller and smaller share of the overall denials.
Anyway, you get the idea. Again, this may not mean much of anything, but it's worth keeping an eye on.
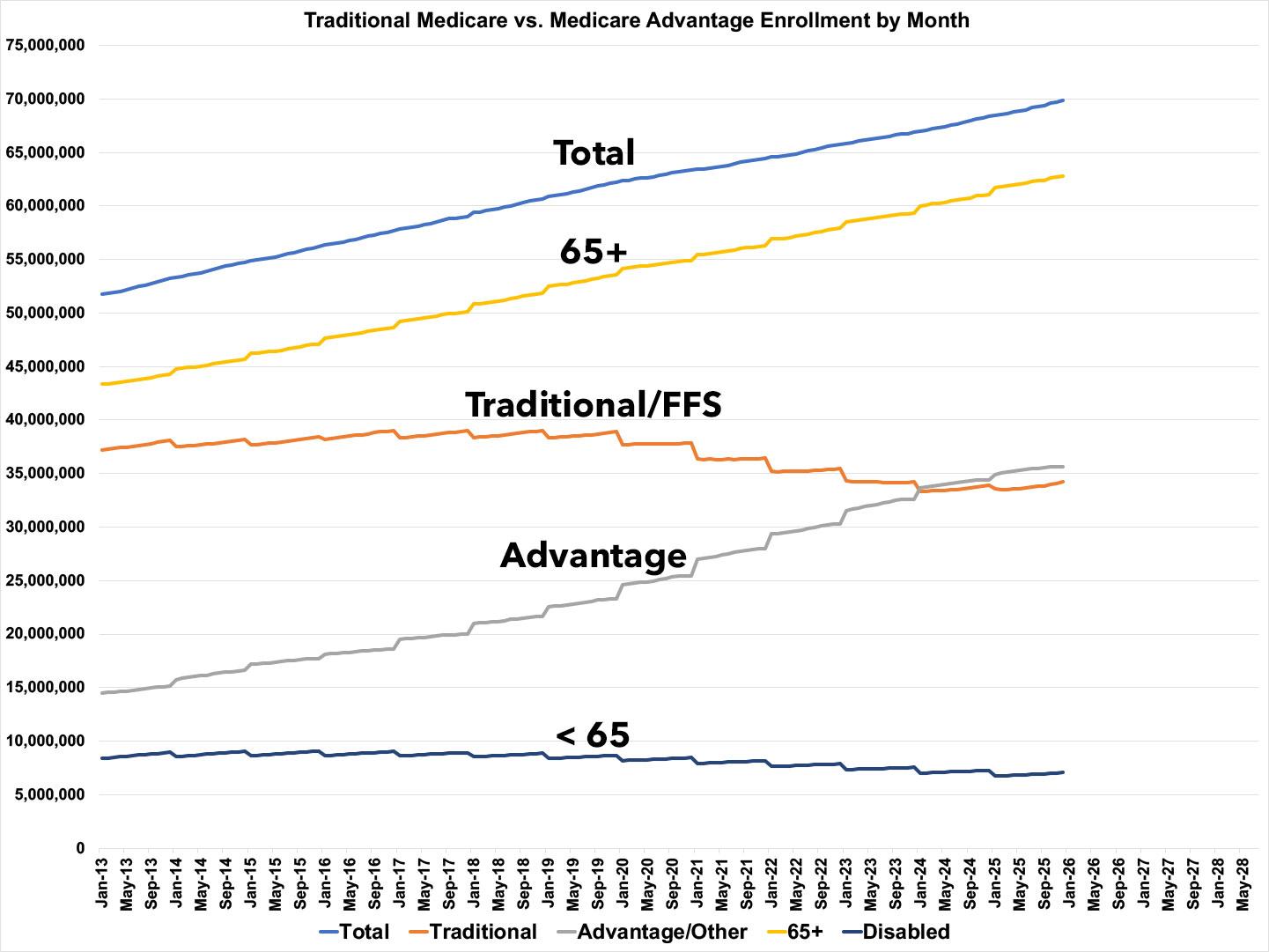
In the meantime, here's how Medicare Advantage enrollment has grown (and how traditional "Fee for Service" Medicare has shrunk) over time:
It's also worth noting that, given the Musk/Trump Admin's obsession with erasing any reference or data regarding gender, race or ethnicity, the Medicare enrollment reports still include breakouts of those demographic factors.
UPDATE: There was another major factor announced last fall which I had forgotten about which may explain some of the December drop as well:
CVS Health, Humana, and UnitedHealth Group have announced that they will pull back on Medicare Advantage (MA) and Part D prescription drug plans next year. These changes are a response to financial pressures, including changes to government funding and rising healthcare costs. This has led insurance carriers to scale back their offerings in less profitable regions.
"The combination of (Centers for Medicare and Medicaid Services) funding cuts, rising healthcare costs, and increased utilization have created headwinds that no organization can ignore," said Bobby Hunter, who is the CEO of Government Programs at UnitedHealthcare.
One of the reasons insurers are dropping Medicare Advantage (MA) plans is reduced government funding. It is estimated that by 2026, government reimbursement will have fallen 20% from 2023 levels, Hunter said. This longer-term cut is masked by the projected 2026 average reimbursement rate increase of 5.06%, which is higher than the initial 2.23% increase proposed by the Biden administration back in January 2025.
- ...UnitedHealthcare (UHC): The nation's largest MA provider is making "strategic adjustments" and will stop offering Medicare Advantage plans in 109 U.S. counties in 2026, impacting 180,000.
- Humana: The second-largest MA insurer is also significantly retrenching, cutting plans in hundreds of counties and in a few states to stabilize its financial margins. Humana plans will be available in 85% of U.S. counties next year, down from 89% in 2025, and in 46 states, down from 48 in 2025.
- Aetna (CVS Health): CVS Health's Aetna insurance business will operate prescription drug plans in 100 fewer U.S. counties next year than it did in 2025. It will provide plans in 43 states and Washington, D.C., and 2,159 counties for 2026, down from 44 states and 2,259 counties in 2025.
While these plan terminations didn't actually kick in until January, it's likely that it did have some impact on December enrollment as well, I'd imagine.