Following up on ACA Open Enrollment data, and just as I predicted a month ago...

...I'm bringing all of this back up again today because I strongly suspect that the situation is about to reverse itself, with the Trump Administration already preparing to brag about impressive-sounding ACA enrollment numbers for 2026 in spite of the enhanced tax credits expiring less than 60 hours from now...even though the actual negative impact of the expiring tax credits (along with several other administrative policy changes made by CMS this year) likely won't be known for several months after Open Enrollment officially ends in January.
...I honestly don't know exactly what it will look like. The main point to keep in mind is that CMS is unlikely to actually publish that data until sometime in July 2026 if at all, so any crowing by the Trump Administration, Congressional Republicans or their allies about the tax credits expiring having a "minimal impact" etc. should be taken with a massive grain of salt until then.
As I noted on January 16th, sure enough, the Wall St. Journal took the bait & posted an editorial piece which was utterly full of shit, falsely claiming that the drop in 2026 ACA exchange enrollment was far smaller than predicted even though a) the actual data won't be known for months and b) they completely misrepresented the projections in the first place:
- They understated the initial data by over 10% out of the gate (the shortfall as of Jan. 3rd was 1.54M plan selections, not 1.40M)
- They confused the CBO's projection of average effectuated enrollees per month (18.9 million) with plan selections as of the end of Open Enrollment (still unknown, likely to be somewhere around ~23.3M give or take)
- They confused the Urban Institute's projection of how many fewer subsidized enrollees there would be this year (7.3 million) with the net drop in total enrollment
- They further confused the Urban Institute's projection of how many more people will become uninsured due to the subsidies expiring (4.8 million) with how many fewer will be enrolled in exchange coverage
- Finally, the WSJ completely ignores (they likely didn't even have a clue, actually) the fact that 9 states with a combined population of over 83 million people (~25% of the total U.S. population) have either newly-launched or retooled programs to at least temporarily backfill some or all of the lost federal tax credits, as well as three states newly implementing robust Premium Alignment pricing policies which dramatically mitigate the damage for many enrollees.
The main point I was making is that not only was it way too early to conclude what the final Open Enrollment Period data would look like, the average effectuated data is likely to look very different from whatever that OEP number does end up being due to many of those who were auto-renewed terminating their coverage the moment they receive their first premium invoice or to others being able to stick it out for a couple of months before being forced into dropping coverage.
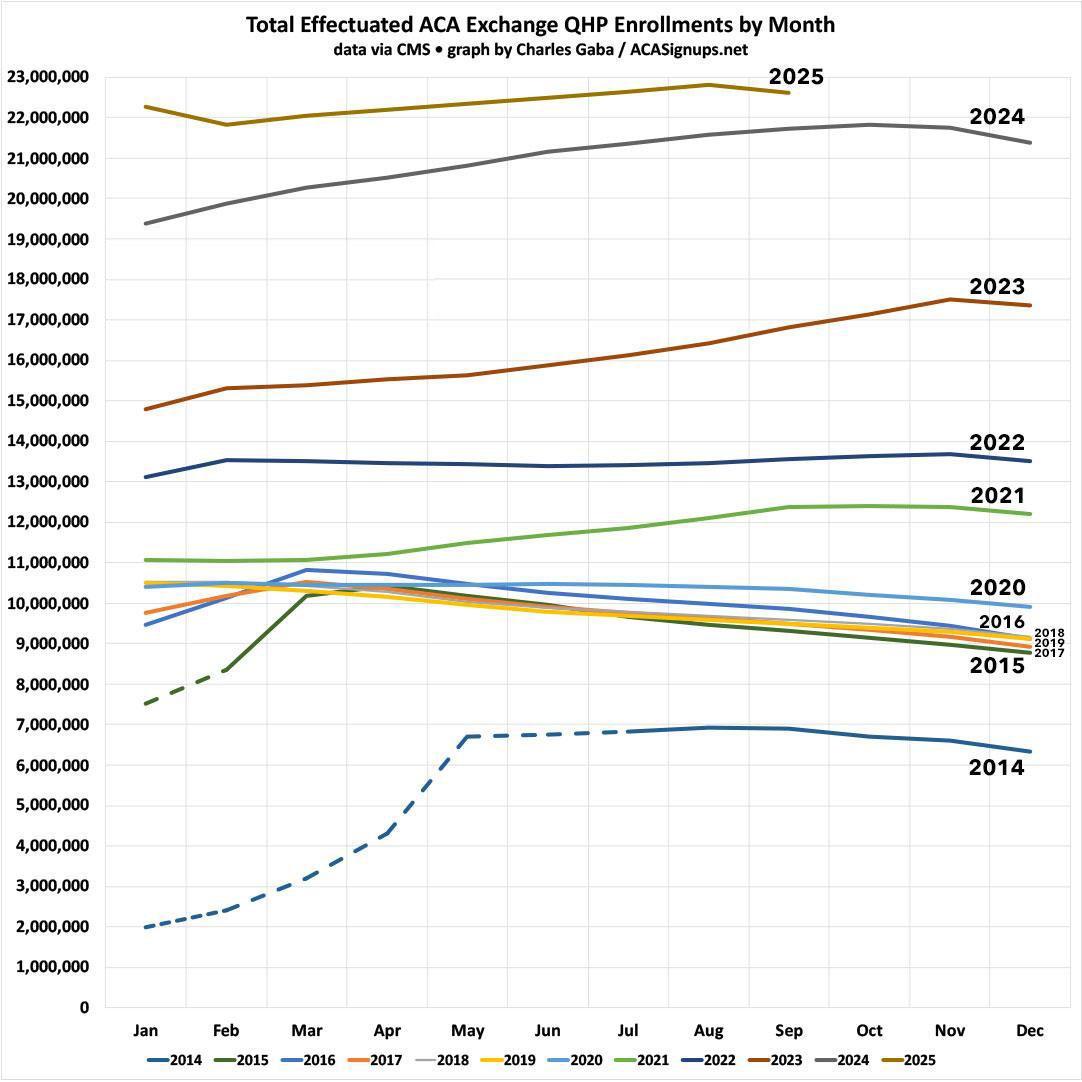
As I noted, this is what actual effectuated enrollment has looked like over time in prior years (early months of 2014 & 2015 are estimated; 2025 only runs thru September). As you can see, prior to the enhanced tax credits being put into effect starting in 2021, there was a clear pattern of effectuated enrollment peaking early in the year before gradually dropping off as the months went by...and prior to 2021 the monthly average never reached higher than ~90% of the OEP plan selection total:
Well, it's only been 10 days since I posted that, but new data is already confirming exactly what I kept saying would happen:
Total enrollments dropped from 1,942,928 as of 12/20 to 1,939,528 as of 12/27, 1,924,899 as of 01/03, 1,910,476 as of 01/10 and 1,906,033 as of 01/17. In other words, more current enrollees have canceled than new enrollees signing up.
...a rise in insurance premiums following the expiration of federal enhanced Premium Tax Credits (ePTCs) may have discouraged some residents from enrolling, said Kevin Patterson, chief executive officer of Connect for Health Colorado – and may also be driving an 83% increase in the number of people who are canceling their plans compared to this time last year, he noted.
...Connect for Health Colorado also reported enrollment declines across several populations. Enrollment among new customers dropped by approximately 24% compared to last year, while enrollments among customers ages 55 and older declined by 6%. Enrollment among customers in rural communities also decreased 5%.
...Early data indicate that enrollment behavior in 2026 is shaped by affordability pressures following the expiration of the Federal Enhanced Premium Tax Credits (EPTCs). More than 8,000 consumers who were previously covered through CoverME.gov have cancelled their coverage since the start of Open Enrollment due, with approximately 33 percent of cancellations pointing to affordability as their cancellation reason. Over 3,000 consumers who have cancelled coverage previously qualified for tax credits in 2025 but no longer qualify, mostly due to federal eligibility changes.
While more than 7,000 new consumers have enrolled, new enrollments in CoverME.gov are down approximately 24 percent compared to this time last year. New enrollments are at the lowest level at this point in Open Enrollment since Maine launched its state-based Marketplace in 2020.
At the same time, more consumers are selecting plans with higher deductibles. Enrollment in bronze plans has increased by more than 10 percentage points and now represents nearly 60 percent of all plan selections.
The full enrollment impact of the loss of enhanced subsidies is unlikely to be realized until after the first quarter of 2026 or later.
A clearer picture of the Maryland marketplace will be more apparent in coming months. The expiration of the credits is expected to result in lapsed policies as consumers are unable to pay the first month’s premium. Cancelled policies also contribute to increasing the cost of coverage in the pool.
Recipients of the Deferred Action for Childhood Arrivals (DACA) which were allowed to enroll through the marketplace for the first time last year were no longer eligible as of September due to the One Big Beautiful Bill Act.
In addition, there are about 18,000 lawfully present immigrants who earn under 100% of the federal poverty level that as of Jan. 1 were no longer eligible for Advanced Premium Tax Credits. Many of them terminated coverage, but not yet all.
104,286 Nevadans enrolled in health insurance plans through NevadaHealthLink.com, with nearly 20% also enrolling in a dental plan.
...By comparison, during the 2025 Open Enrollment Period (OEP), 110,687 NV residents selected plans, so that's a 5.8% drop in plan selections year over year.
As of December 27th, Nevada was only running 2.5% behind last year, which goes to my point about the WSJ massively jumping the gun with their declaration that the 2026 ACA enrollment drop was exaggerated.
- As of the 12/27/25 CMS report, New Mexico was running 19.5% ahead of the same point a year earlier.
- By the end of the 2026 OEP, New Mexico was only running 17.1% ahead of the final 2025 OEP tally.
Expiring enhanced premium tax credits (ePTCs) increased many people’s monthly costs. Around 40,000 fewer Washingtonians are receiving premium tax credits in 2026 than 2025. Some customers saw significant increases in their health insurance premiums, resulting in more than 61,000 customers changing their plans.
Customers also canceled their coverage more than any year prior — more than 28,000 in 2026 compared to just over 20,000 in 2025. Based on higher costs, it is expected that even more customers will disenroll before final counts are published in spring.
...The Exchange will not have the full picture of enrollment data until the spring as many people will drop coverage in the months to come. Customers have 30 days to pay their first premium and to make decisions about whether to continue to pay high premiums due to the expiration of ePTCs. Many customers shared their financial concerns with the Exchange and were unsure if they could keep their higher priced health plans going forward.
So, what does this all look like in hard numbers?
Well, as I keep saying (reiterated by several of the press releases above), it will take months to know for sure, but there's preliminary data already showing that even official OEP enrollment will be down by more than the WSJ claimed.
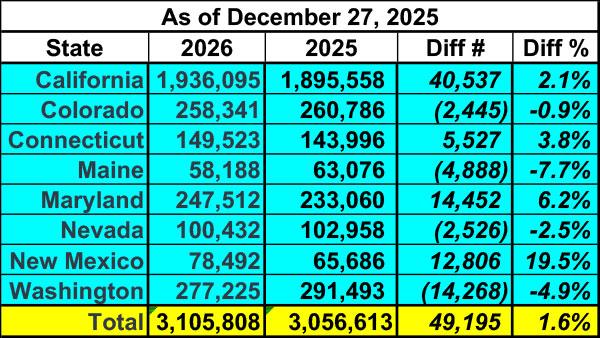
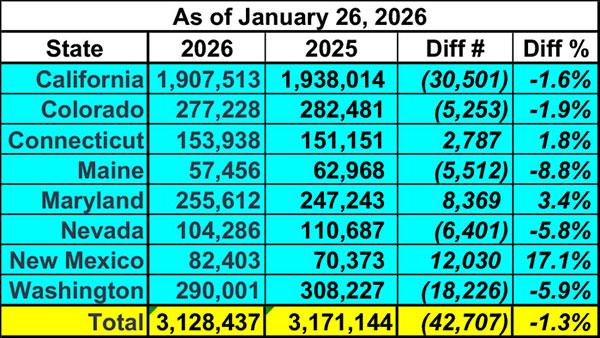
This table breaks out the year over year OEP plan selections as of 12/27 for the states above (plus Connecticut)...followed by the most recent year over year OEP data:
Update: Just a few hours after I published this, Covered California updated their enrollment dashboard to include another week of data; the tables below have been updated to reflect this:
Across these 8 states, plan selections went from running 1.6% higher than a year earlier to 1.3% lower...a net gap increase of nearly 92,000 people.
If you extrapolated this across all 50 states +DC, it would amount to the year over year drop increasing by around ~700,000 more people than it was as of the CMS report which the WSJ based their claims on.
That's still likely a major underestimate, however, because again, six of the eight states above are among those backfilling significant chunks of the lost federal tax credits (New Mexico is backfilling 100% of them for every enrollee on their exchange, which is why their enrollment is up dramatically year over year). In addition, Washington is one of three states (Arkansas & Illinois are the other two) which has newly-implemented Premium Alignment pricing this year.
All of this strongly suggests that terminations since that CMS report both are & will be significantly higher across the remaining 42 states, most of which have no such measures in place to mitigate the financial carnage, over the next few months.
Again: Assuming CMS follows a pattern similar to prior years...
- The final 2026 Open Enrollment Period report won't be published until late April/early May
- EFFECTUATED enrollment data for the first few months of 2026 won't be published until sometime in July
- AVERAGE MONTHLY effectuated enrollment data for the full year of 2026 (which is what the CBO projection referred to) won't be known until sometime in 2027 (again, as of today they haven't even published anything past September for 2025 monthly effectuations)
Keep all of this in mind if/when you hear Trump, RFK Jr., Dr. Oz, GOP House/Senate members, FOX News talking heads or the WSJ Editorial Board flapping their gums again about "The ObamaCare Enrollment Apocalypse That Wasn’t" again.