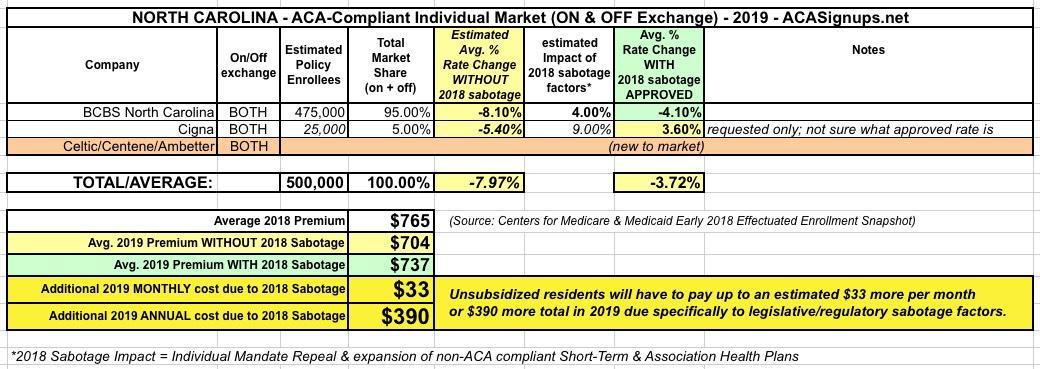
North Carolina: APPROVED 2019 rate change: 3.7% drop..but WOULD have dropped 8.0% w/out #ACASabotage
North Carolina has three insurance carriers offering individual market policies next year: Blue Cross Blue Shield, which holds a whopping 96% of the individual market; Cigna, which holds the remaining 4%, and newcomer Ambetter (aka Centene).
I ran a write-up on BCBSNC's preliminary 2019 rate request at the end of July. While they're lowering their 2019 premiums by 4.1%, they also made it very clear that yes, they'd be lowering rates even further if not for the ACA's individual mandate penalty being repealed:
BLUE CROSS NC FILES TO LOWER ACA RATES BY AVERAGE OF 4.1 PERCENT
Durham, N.C. – Blue Cross and Blue Shield of North Carolina (Blue Cross NC) announced today it requested an overall average rate decrease of 4.1 percent for 2019 Affordable Care Act (ACA) plans offered to individuals. The reduction marks the first rate decrease in the history of Blue Cross NC since entering the current individual market more than 25 years ago.
...Many factors went into the Blue Cross NC’s rate filing:
- After several years in the ACA marketplace, Blue Cross NC has gained substantial information about the pool of customers, including how to help manage their care, reduce their medical expenses and price health plans to fit their needs.
- Blue Cross NC used tax savings from the 2017 Tax Cuts and Jobs Act to lower rates by an additional 0.5 percent.
- Congress’ one-year suspension of the ACA’s Health Insurer Tax (HIT) for 2019 helped lower rates by an additional 3 percent. Rates for 2020 will need to be approximately 3 percent higher unless Congress extends the suspension or ends this tax altogether.
- Had the federal government not eliminated the individual mandate penalty, requested rates would be another 4 percent lower.
- If federal Cost Sharing Reduction (CSR) payments to insurers that were eliminated as of October 2017 were still in place, requested rates would be another 14 percent lower.
- Requested rates assume that transfers of funds among insurers under the Risk Adjustment Program will take place as normal for 2019.
- Blue Cross NC has entered into new arrangements with health systems that will reduce costs in 2019. Blue Cross NC thanks these health systems for their partnership on behalf of consumers.
Pretty cut & dried: 4.1% drop with mandate repeal, 8.1% drop without.
At the time I didn't have Cigna's requested rate changes, but it didn't make much difference to the statewide average seeing how they only hold 4% of the market. Ambetter, meanwhile, is brand new to the state, so there aren't any existing rates to be changed.
Today, however, this local NC article, primarily about BCBSNC's 4.1% drop being approved also mentions that Cigna requested a 3.6% rate increase, and that they appear to have a slightly higher enrollment than I thought--the article reiterates BCBS's 475,000 number, but also notes that NC's total individual market is "over 500,000 people", so Cigna must have at least 25K.
I don't know whether Cigna's 3.6% request was approved as is or not, but if it was, this is what North Carolina's 2019 weighted average looks like:
That's a weighted average rate reduction of 3.7%. The Urban Institute projected a whopping 17.8% rate increase due to mandate repeal/short-term plans, but given that BCBSNC states that it's only adding 4 points to their rates, I'm going to cut that in half for Cigna and assume a 9 point impact.
Overall, this means unsubsidized enrollees will be paying around $390 apiece more than they would if the mandate hadn't been repealed.
The official BCBSNC blog provides some more handy information as well:
...We reached an agreement with UNC Health Alliance to lower individual ACA rates in the Greater Triangle Region by more than 21% before subsidies. Benefits are staying similar.
It’s our first rate decrease since we entered the current individual market more than 25 years ago. Many factors allowed us to lower rates – the biggest being new provider arrangements that will reduce health care costs by $120M in 2019.
While most things will remain the same for most people, some members in the Triangle will see changes to their network. We reached an agreement with UNC Health Alliance that will allow us to lower rates by more than $140 a month on average, per person before subsidies.
...The 4.1 percent reduction is an average. This year, rate changes range from a 22 percent reduction to a 9.5 percent increase.
...If you live outside the Greater Triangle region, not much is changing.
- Through new arrangements with regional providers, Blue Cross NC will be reducing pre-subsidy premiums in Charlotte and Gastonia by an average of 16.5 percent. The rate reductions were made possible through collaboration with Blue Cross NC’s provider partners.
- Blue Local with Atrium Health and Blue Value with Novant and Caromont will continue to be offered.
- The average Blue Value price reduction is $173 a month before subsidies. The average Blue Local with Atrium Health price reduction is $87 a month before subsidies. Benefits will remain similar.
- Rates are also being reduced in the Triangle by a pre-subsidy average of $140 a month, due to a new agreement with UNC Health Alliance. Benefits will remain similar.
- Beginning in 2019, Blue Cross NC will no longer offer its Blue Local with Duke Health and WakeMedSM product in the individual market.
- Duke Health and WakeMed remain close partners with Blue Cross NC. Both providers are still in-network for other Blue Cross NC products, such as Medicare Advantage, FEP, State Health Plan, and the majority of our Blue Advantage®, Blue SelectSM and group plans.
...After December 31, 2018, you can continue seeing your Duke Health and WakeMed doctor but they will be considered out-of-network; you will pay out-of-network rates which are much higher than in-network and out-of-network benefits will apply. In order to have the lowest, out-of-pocket costs you will need to transition to a UNC Health Alliance provider.
...Blue Cross NC will continue offering transitional plans in 2019.
The requested rate increase for transitional plans in 2019 is 9.8 percent. These plans were purchased between March 2010, when the ACA was signed, and October 2013 when regulations went into effect. Transitional plans cannot be sold to new customers because they do not meet ACA requirements. Currently, there are 41,500 members with these plans.