California: @CoveredCA issues preliminary 2021 rate hikes; 0.6% indy market; #COVID19 nominal factor; 230K enrolled via #COVID19 SEP to date
Just out from Covered California:
California’s Efforts to Build on the Affordable Care Act Lead to a Record-Low Rate Change for the Second Consecutive Year
- The preliminary rate change for California’s individual market will be 0.6 percent in 2021, which marks a record low for the second consecutive year and follows California’s reforms to build on and strengthen the Affordable Care Act.
- Covered California’s increased enrollment, driven by state policies and significant investments in marketing and outreach, has resulted in California having one of the healthiest individual market consumer pools and lower costs for consumers.
- The impact of COVID-19 on health plans’ costs has been less than anticipated as many people deferred or avoided health care services in 2020, and while those costs are rebounding, it now appears the pandemic will have little effect on the total costs of care in California’s individual market for 2020 and 2021.
- All 11 health insurance companies will return to the market for 2021, and two carriers will expand their coverage areas, giving virtually all Californians a choice of two carriers and 88 percent the ability to choose from three carriers or more.
SACRAMENTO, Calif. — Covered California announced on Tuesday a record-low insurance premium rate change for the second consecutive year. The preliminary average rate change for California’s individual market is 0.6 percent for the upcoming 2021 plan year, which is the lowest mark since the launch of the Affordable Care Act and follows a rate change of only 0.8 percent in 2020.
“California continues to show the nation what can be done when you build on and strengthen the Affordable Care Act,” said Peter V. Lee, executive director of Covered California. “California’s bold policies to provide additional state financial help, to reinstate the penalty to encourage consumers to enroll in health care, and to make significant marketing investments in Covered California are providing stability and lower costs in the face of national uncertainty.”
The historically low rate change was driven by California’s efforts to build on the Affordable Care Act through affordability initiatives — the state subsidies and the individual mandate enforcement provision that went into effect in 2020 — as well as ongoing investments in marketing and outreach that have led to increased enrollment and one of the healthiest consumer pools in the nation. The most recent data from the Centers for Medicare and Medicaid Services found that California has the second lowest “State Average Plan Liability Risk Score” in the nation, which marked the sixth straight year that California has been among the top five healthiest states.
“Access to affordable health care coverage is more critical than ever as our nation and state navigate the COVID-19 pandemic,” said Gov. Gavin Newsom. “Covered California is leading the nation by eliminating barriers to access and providing Californians real opportunities to get the care and coverage they need.”
California’s Individual Market Rate Change for 2021
California’s individual market consists of approximately 2.3 million people, including 1.5 million enrolled through Covered California. Nearly nine out of 10 (88 percent) of those enrolled through the marketplace are getting federal or state subsidies, or both, to lower their costs; the rest are buying coverage directly from carriers in the individual market.
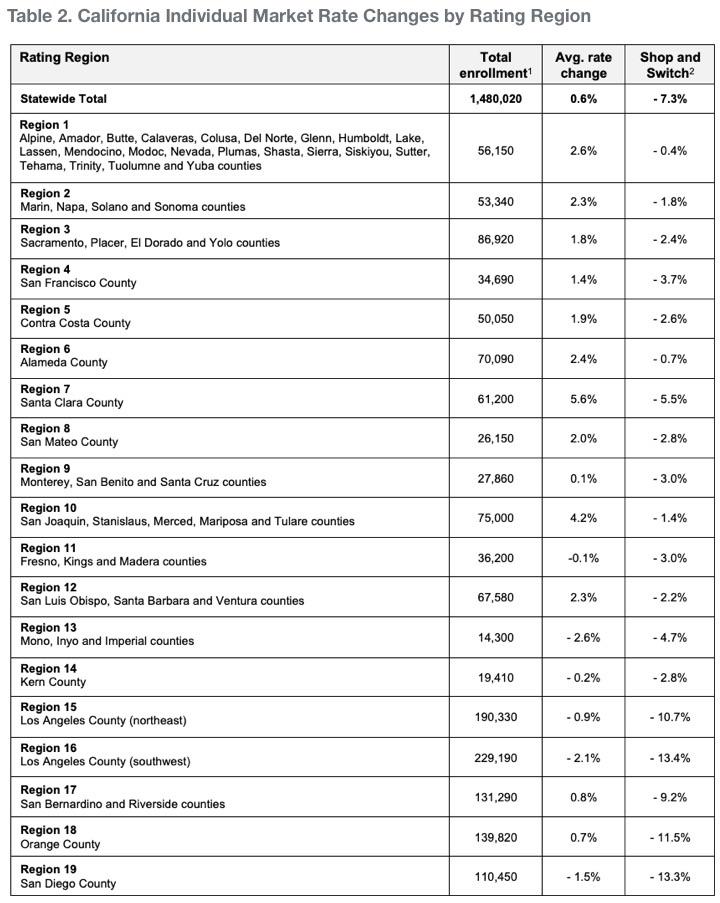
The preliminary average rate change of 0.6 percent varies by region and by an individual’s personal situation (see Table 2: Covered California Rate Changes by Rating Region).
“Health care costs are never a one-year story, and California has shown — again and again — that it can provide stability and lower costs in the face of federal policy changes that could have resulted in dramatic rate increases,” Lee said. “The past three years can serve as a roadmap for the rest of the nation when it comes to successfully responding to federal challenges, reducing prices and encouraging enrollment.”
The main factors that contributed to the low rate change include the following:
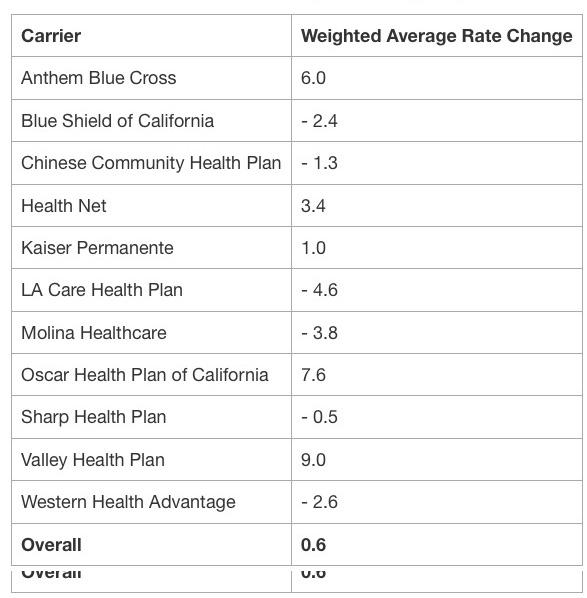
- Increases in Health Care Costs: The underlying trend for health care costs — absent the impact of COVID-19 — for 2021 was generally projected to be in the 4 to 8 percent range across Covered California’s 11 contracted health insurance companies.
- COVID-19 Impact: Covered California reviewed the experiences of health plans through 2020 and their projections for 2021 related to COVID-19 health care costs. While carriers did incur increased costs for COVID-19 treatments, increased telehealth provider services and extended grace periods for consumers enrolled during the current year, the costs were offset by a decrease in the volume of medical care and elective procedures as many people decided to stay home during the pandemic. While there continues to be considerable uncertainty about the pandemic and resulting health care costs, the latest information shows that health care costs will likely end up being close to what was originally priced for in California. For 2021, most plans project that caring for enrolled members with COVID-19 and the impacts of the pandemic on other care will have no to little net impact on premiums.
- Strong and Healthy Enrollment: Covered California saw a surge of new sign-ups during both the 2020 open-enrollment period (a 41 percent increase over the previous year) and the current special-enrollment period, during which more than 230,000 people have signed up for coverage since March 20, which is more than double the rate seen during the same period last year. The risk and demographic analysis of the new consumers indicates that both cohorts of incoming consumers are “healthier” on average than the equivalent cohorts from 2019.
- Removal of Federal Health Plan Tax: The repeal of the Health Insurer Tax lowered premiums by 0 percent to 3.3 percent across carriers, with the weighted average decrease to premiums at 1.7 percent.
- Exchange Fee: The participation fee Covered California charges qualified health plan issuers was reduced for 2021 from 3.5 percent to 3.25 percent, leading to a further reduction in premium.
“After a large increase in 2019 caused by the federal action that zeroed out the penalty on individuals failing to have insurance coverage, California has seen two years of less than 1 percent premium increases,” Lee said. “Covered California’s ability to provide stability and lower costs to consumers is the product of strong state policies, a competitive market and major investments in marketing.”
“State policies make a difference, and California is showing how you can keep health care costs under control and bring coverage within reach of more people,” said California Health and Human Services Secretary and Covered California Board Chair, Dr. Mark Ghaly. “Making more financial help available and encouraging consumers to get covered means fewer people without insurance and lower health care costs for everybody.”
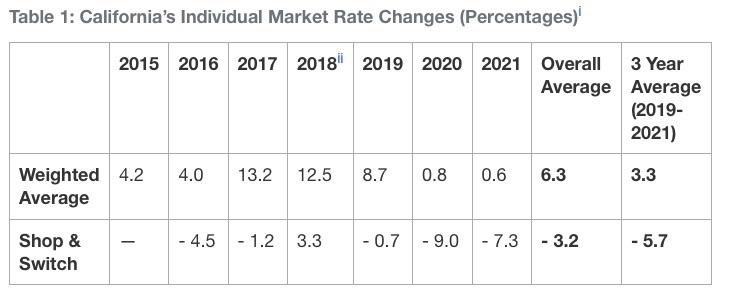
Consumers both on and off the exchange will benefit from Covered California’s competitive marketplace, which allows them to shop for the best value and save money if they switch plans. The average rate change for unsubsidized consumers who shop and switch to the lowest-cost plan in the same metal tier is -7.3 percent, which means many Californians may be able to get a lower gross premium than they have now if they shop and switch (see Table 1: California’s Individual Market Rate Changes).
“Shopping for the best deal will once again be important for consumers because as our carriers become more competitive on pricing and the cost of the second-lowest Silver plan decreases, consumers may find that the amount of their financial help is lowered,” Lee said.
The preliminary rates will be filed with California’s regulators, the Department of Managed Health Care and the Department of Insurance, and are subject to their final reviews.
Financial Help Lowers Costs for Consumers
Roughly nine out of every 10 consumers who enroll through Covered California receive financial help — in the form of federal tax credits, state subsidies, or both — which help make health care more affordable. California’s state-specific enhanced subsidies are benefiting about 590,000 consumers out of the current 1.5 million enrollees in Covered California. In 2020, with the combination of federal tax credits and state subsidies, the average consumer receiving financial help were paying only $130 per month of their total premium of $587 (with federal and state assistance reducing their costs by $457 or nearly 80 percent).
In addition, nearly 38,000 middle-income consumers have qualified for new state subsidies, with an average state subsidy to eligible households of $475 per month, lowering their monthly premium by nearly 44 percent.
The state subsidies are only available to eligible consumers through Covered California. The amount of financial help consumers receive will vary depending on their age, their annual household income and the cost of health care in their region.
Increased Competition and Consumer Choice
In the coming year, all 11 carriers will continue offering products across the state, and two carriers will expand their coverage areas, providing increased competition and consumer choice. In 2021, 99.8 percent of Californians will have two or more choices, 88 percent will be able to choose from three carriers or more, and over three-fourths of Californians (77 percent) will have four or more choices.
Anthem Blue Cross will expand into Imperial, Inyo, Kern, Mono and Orange counties, and Oscar Health Insurance will expand into San Mateo County.
“A competitive market means virtually everyone across California will have a choice in coverage and is further proof that the Affordable Care Act is working in California for both consumers and health plans,” Lee said.
Consumers can find out what they will pay for their 2021 coverage starting during the renewal period in October, when they can visit Covered California’s website at www.CoveredCA.com and begin using the Shop and Compare Tool.
Staying Safe While Getting Help Enrolling
Covered California is currently in a special-enrollment period due to the COVID-19 pandemic, which allows the uninsured to sign up for coverage if they are eligible to enroll in the exchange. The most recent data shows that 231,040 people have signed up through Covered California for health care coverage between March 20 and July 25, which is more than twice the number who signed up during the same time last year. The special-enrollment period is available through the end of August.
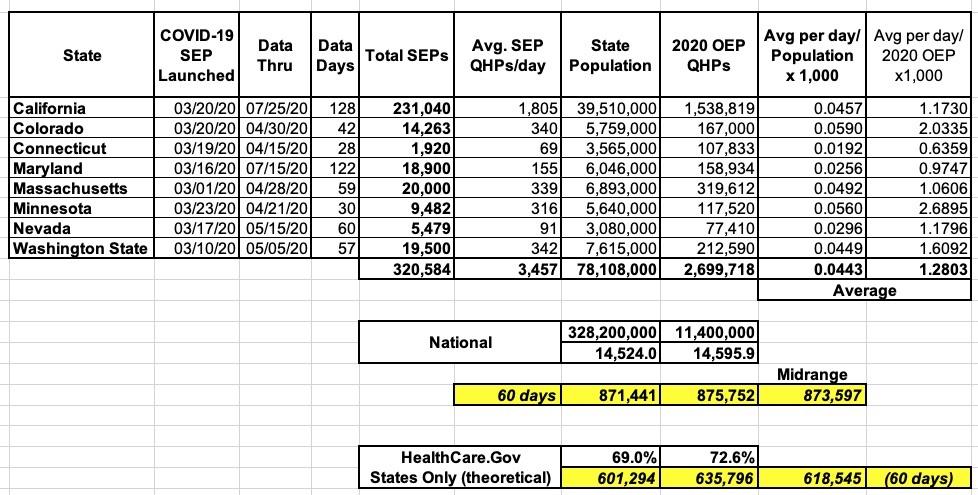
As an aside, this brings the total number of confirmed COVID-19-specific SEP enrollments up to at least 320,000 across the 8 state exchanges which offered one and have released their COVID SEP enrollment data:
Consumers can easily find out if they are eligible for Covered California or Medi-Cal – and see whether they qualify for financial help and which plans are available in their area – by using the CoveredCA.Com Shop and Compare Tool and entering their ZIP code, household income and the ages of those who need coverage.
Those interested in learning more about their coverage options can also:
- Visit www.CoveredCA.com.
- Get free and confidential assistance over the phone, in a variety of languages, from a certified enroller.
- Have a certified enroller call them and help them for free.
- Call Covered California at (800) 300-1506.
Interested consumers should go to www.CoveredCA.com to find out if they qualify for financial help and find free local help to enroll. They can contact the Covered California service center for enrollment assistance by calling (800) 300-1506.
Table 2. California Individual Market Rate Changes by Rating Region
- 1. Effectuated enrollment for coverage in the month of March 2020: See here for full data profile.
- 2 Shop and Switch refers to the average rate change a consumer could see if they shop around and switch to the lowest-cost plan in their current metal tier.
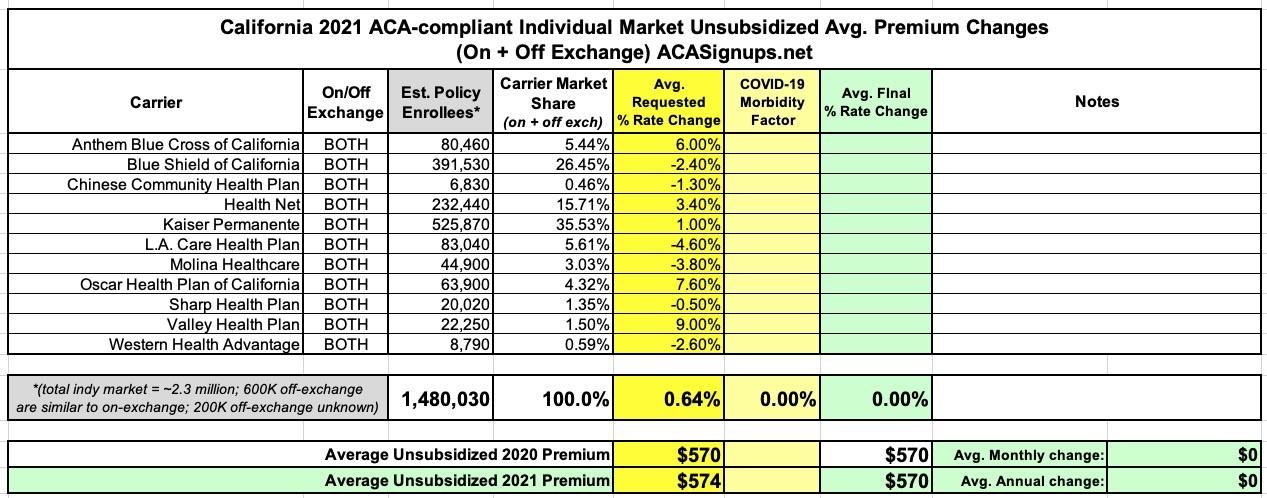
Here's what this looks like with enrollment figures included. It's important to note that unlike my spreadsheets for most other states, the one below for California only includes on-exchange enrollees. California's total individual market is around 2.3 million people, with the remaining ~800,000 being enrolled in OFF-exchange ACA policies.
HOWEVER, I asked about this during the CoveredCA webinar a few moments ago and Peter Lee (CoveredCA executive director) stated that around 3/4ths of those 800K (roughly 600K) are enrolled in "mirrored" ACA plans which are identical to the on-exchange plans and should be very similar in breakout in terms of average rate changes/etc. The other 200K enrollees are in non-standard off-exchange plans which they haven't really looked at yet, but it sounds like the overall weighted average including all 2.3 million should still be pretty close to 0.6%:
Unfortunately, neither the press release nor the webinar provided any info whatsoever about California's small group market, but I've always been kind of spotty about covering that anyway. It would still be nice to see it, and they said data on the sm. biz market will be coming soon.
About Covered California
Covered California is the state’s health insurance marketplace, where Californians can find affordable, high-quality insurance from top insurance companies. Covered California is the only place where individuals who qualify can get financial assistance on a sliding scale to reduce premium costs. Consumers can then compare health insurance plans and choose the plan that works best for their health needs and budget. Depending on their income, some consumers may qualify for the low-cost or no-cost Medi-Cal program.
Covered California is an independent part of the state government whose job is to make the health insurance marketplace work for California’s consumers. It is overseen by a five-member board appointed by the governor and the Legislature. For more information about Covered California, please visit www.CoveredCA.com.
- i The premium changes reported are based on the total premium, while many consumers pay only a portion of the total premium due to the federal and state subsidies that lower their costs. In some cases, consumers may receive relatively lower subsidies in the coming year so their out-of-pocket premium expenses may be different from the “average change” in premium.
- ii The Weighted Average rate increase for 2018 was 21.1 percent, but much of that increase was directly offset for consumers by an increase in the federal subsidy which lowered their net premium. The 12.5 percent Weighted Average is consistent with prior Covered California rate change analyses which removed the cost sharing reduction (CSR) “surcharge” in Silver, since off-exchange enrollees do not incur the surcharge, and Covered California encouraged its unsubsidized Silver enrollees to move off-exchange to avoid the surcharge. The vast majority of the consumers on-exchange did not experience the surcharge because tax credits also grew as a result.
- iii The weighted average rate change refers to the overall average throughout the state. Actual rate changes for consumers may vary based on their personal circumstances, the area they live in, and their plan’s metal tier.