Colorado: APPROVED rate hikes: 27% if CSRs are paid, 33% (or 41%?) if not
(sigh) Colorado's state insurance division just released their approved 2018 rate increases (busy day!), and the situation appears to be similar to Maine: The average requested rates which I thought already assumed no CSR reimbursements appear to have assumed CSRs would be paid after all:
Division of Insurance approves health insurance premiums for 2018
Commissioner: Measures to stablize market for 2018 must happen by Sept. 30DENVER (Sept. 6, 2017) – The Colorado Division of Insurance (DOI), part of the Department of Regulatory Agencies (DORA), has approved the individual and small group health insurance plans for 2018. Average premium changes within each market - individual and small group - as well as the average change for each insurance company are listed below.
The Division will have more information, with tables and charts that offer detailed analyses such as county-by-county statistics, in late September / early October. At that time, the DOI will also announce the date of a public forum to discuss the 2018 plans and premiums, with personnel from the Division as well as representatives from the insurance companies in attendance.
Providing stability for the individual market
Colorado did not lose any on-exchange insurance companies selling individual plans for 2018, as noted in the August 16 release. The Division worked to keep those companies in the market by maintaining ongoing discussions, providing information and addressing their concerns.
“While we have worked to provide a foundation of stability in our state, I want to echo what Governor Hickenlooper said in his letter last week,” said Insurance Commissioner Marguerite Salazar. “Even though we need long-term approaches that preserve the gains we’ve made and work to improve our health care system, the immediate need is for our Congressional partners to take actions that stabilize the market and sweep away the uncertainty pushing up rates and making companies skittish. Along with the Governor, I implore Congress to fully fund the CSR program to provide that relief.”
Added Commissioner Salazar, “In the spirit of the bi-partisan approach being spearheaded by Governors Hickenlooper and Kasich, we also turn to our friends in Congress on both sides of the aisle to establish a reinsurance program that would provide relief to the entire individual market, including those who don’t qualify for subsidies, by reducing rates for 2018. Affordable health insurance is truly a non-partisan issue, and these rate increases keep me up at night. While a a reinsurance program can have a dramatic effect on rates, I have to stress that time is of the essence. Any help that Congress can offer for 2018 would have to be completed by Sept. 30 of this year to ensure that we have enough time to implement that help before open enrollment for 2018. But we are preparing and we are working with our colleagues at Connect for Health Colorado to make sure we are ready to respond if Congress acts.”
“We at Connect for Health Colorado are near final preparations for the 2018 Open Enrollment Period but we support the proposals to add stability to the health insurance Marketplace in 2018 that the Governor has brought forward and which have the backing of other state marketplaces.We will do everything in our power to implement changes that could help our customers,” said Connect for Health Colorado Chief Executive Officer Kevin Patterson. “We stand committed to work with the Division of Insurance to increase access, affordability and choice for individuals and small businesses buying health insurance in our state.”
Premium increases in the individual and small group market
This past Spring, the Division asked insurance companies to submit two sets of premiums for 2018 - one that assumed the Cost Sharing Reductions (CSRs) would be funded by the Federal government in 2018, while the other set assumed the CSRs would not be funded. The premiums detailed below for the individual market use the rates that assume the CSRs will continue to be funded.
“Recent signs point to more and more bi-partisan support of the CSRs, so I believed it was important to use the CSR-funded premiums in our review,” said Commissioner Salazar. “The premiums would be up to 14 percent higher if we used the non-CSR-funded premium requests. I simply cannot ask my fellow Coloradans to pay even higher premiums for something that at this point almost everyone agrees should be fixed.”
In Colorado, premiums for individual plans (not from an employer) will be increasing by an average of 26.7 percent. It’s important to remember that this number and the numbers below are averages. The specific plan purchased, along with a person’s age and residential location will impact their specific premium, making it higher or lower from the average. In Colorado, the individual market (plans not from an employer) makes up about 7 - 8 percent of the population who have health insurance (around 450,000 people), while at least 51 percent of Coloradans get their insurance through an employer (small and large employers).
Know that these average premium changes do not reflect federal tax credits for consumers, known as Advance Premium Tax Credits (APTC). These credits make premiums more affordable for consumers who qualify. It is also important to note that in many cases, people can reduce the impact of increasing premiums by shopping and comparing their health insurance options.
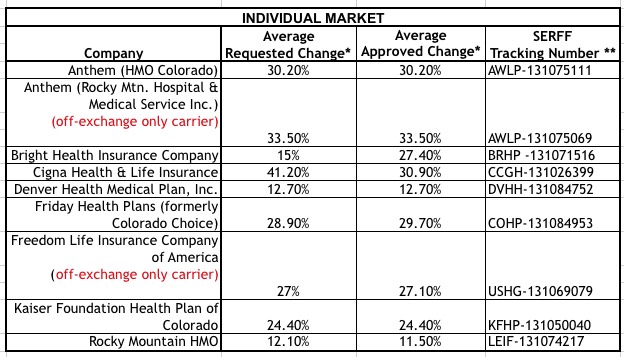
INDIVIDUAL Medical Plans, Average Premium Change, by Company
Average individual premium change across all companies: 26.7% (average requested change was 26.96%)
* Averaged over all individual plans continuing from 2017 into 2018 that a company will sell, in all areas of Colorado where the company does business, for all ages.
** The SERFF Tracking Number is way to search for the filing on the Division of Insurance’s system.
That "up to 14% higher" quote is a bit confusing for two reasons: First, because of the "up to" part; second, because I don't know if that 14% figure refers to all individual policies or only Silver plans. The Kaiser Family Foundation estimated that killing CSR payments should add an average of 15% to Silver plans specifically in Medicaid expansion states; since only 44% of Colorado exchange enrollees chose Silver plans, 14% added to them would translate into perhaps 6.2% being added across all metal levels. Until I clarify this, I'm going to err on the side of caution and assume the lower 6.2% CSR factor.
If so, that gives the following approved average rate increases on the individual market:
- If CSR payments are made: 26.7%
- If CSR payments aren't made (assuming 14% only applies to Silver plans): 32.9%
- If CSR payments aren't made (assuming 14% applies to all metal levels): 40.7%
The press release also breaks out the approved small business market rate changes:
In the small group market (health plans for small employers with 2 - 100 employees), the average increase will be 6.6 percent. Insurers have more experience working with this market and better understand how to price their products, which is why increases are typically lower than the individual market.
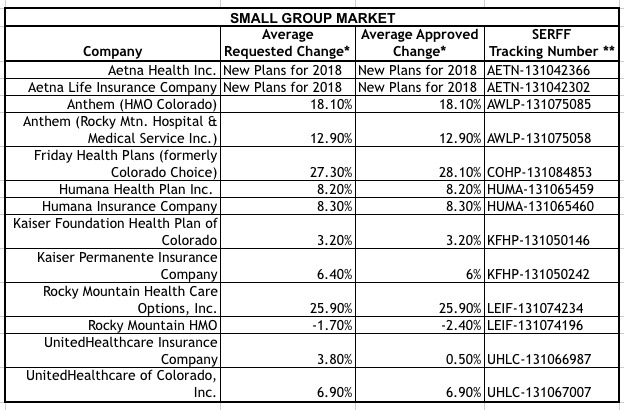
SMALL GROUP Medical Plans, Average Premium Change, by Company
Average small group premium change across all companies: 6.6% (average requested change was 7.46%)