HHS Dept. targets These Darned Kids Today® for OE4
One of the biggest challenges the HHS Dept. has encountered when it comes to enrolling people in ACA exchange policies has been encouraging (or "goading" depending on your POV) millennials into signing up. This is important for several reasons:
- First: The sheer numbers. One of the major goals of the ACA is to reduce the uninsured rate by as much as possible, after all; the more people who enroll, the better.
- Second: Funding the exchanges. This isn't as much of an issue for HealthCare.Gov, since it's federally funded and therefore presumably has more leeway/flexibility in terms of covering any budget shortfalls...but the state-based exchanges are all funded via some sort of per-enrollee fee. The more people who enroll, the more tax/fee revenue the exchanges receive to keep operating. This isn't as vital in some states as in others due to variances in the tax/fee structure, but the bottom line is that they need a minimum threshold enrollee base to keep afloat.
- Third, and most importantly, however, is the impact on the risk pool. The original hope for the exchanges (for the entire individual market including off-exhange enrollees, really, since all ACA policies are part of the same risk pool) was that around 40% of all enrollees would be 18-35 years old. The reason for this is simple: Younger people tend to be in better shape than older folks, and are therefore less expensive to treat. Of course, I suppose it could be argued that younger people are also more likely to get injured by doing high-risk activities like snowmobiling, ski-jumping and so forth, but it's still a lot less expensive to treat a broken leg than to have chemotherapy or whatever.
Anyway, the actual percentage of Young Adults has remained consistently at around 28%, about 30% lower than officials keep hoping for in order to ensure a fairly stable risk pool. The youngins' just don't seem to be diving into the risk pool the way that HHS keeps hoping, so this fall, they're upping their outreach game in several ways:
Strengthening the Marketplace by Covering Young Adults
Deploying New Targeting Strategies and Partnerships to Reach Young Adults and Others Who Are Still UninsuredToday, we are announcing a series of actions to step up Marketplace outreach, especially to young adults, for the 2017 Open Enrollment. Highlights include:
- New outreach to uninsured people who paid the individual responsibility penalty. For the first time this fall, we will conduct outreach to individuals and families who paid the fee for being uninsured, or claimed an exemption from that fee, for 2015. Young adults are overrepresented among those who paid the fee, and healthier individuals of all ages presumably are as well. This new outreach strategy, which has been recommended by outside experts and is already in use in Massachusetts, will let us directly reach millions of people who were recently uninsured and may newly appreciate the value of Marketplace coverage.
- Smarter outreach during Open Enrollment, especially to young adults. Research during the 2016 Open Enrollment showed that young adults are almost twice as likely as older consumers to enroll because they receive an email about Marketplace coverage. During the upcoming Open Enrollment, we will draw on lessons learned this year about the messages, timing, and tactics that make email outreach more effective. Also, new since the 2016 Open Enrollment, this year we will be able to email consumers in near-to-real time if they open an account but don’t start an application, start an application but don’t finish, or select a plan but don’t pay their first premium. We’ve learned that sending an email, with the right information, at just the right time, can make a significant difference in whether someone gets covered, and those are lessons we’ll act on this year.
- Facilitating young adults’ coverage transitions. Today, we are making it easier for issuers to conduct outreach to young adults turning age 26 and moving off their parent’s plans. Specifically, new guidance from the Department of Labor makes clear that the sponsors of employer plans can – and are encouraged to – provide additional information that will help young adults understand their options and enroll in Marketplace coverage as appropriate. Along with issuing new policy guidance, we are strongly encouraging insurers to contact these consumers with targeted information about Marketplace options. Additionally, on June 13, we provided states and outreach organizations with $32 million in additional funding to help with Medicaid and Children’s Health Insurance Program (CHIP) outreach. In conjunction with that funding announcement, we reminded them of their obligation to help children aging out of Medicaid and CHIP transition to Marketplace or other coverage.
- Public-private partnerships to engage young adults. HHS has created a network of diverse outreach partners. While we will keep building that network until the start of the 2017 Open Enrollment and beyond, we are excited to announce that this year’s partnerships will include:
- Lyft: New this year, Lyft will develop user discount codes for people utilizing the ride-sharing service to attend Open Enrollment events where they can receive assistance signing up for coverage via the ACA. In addition, Lyft will again amplify enrollment deadlines and the importance of getting health insurance via the ACA to their drivers in 190 cities.
- American Hospital Association: Along with other actions, the American Hospital Association will develop a social media toolkit that hospitals may use to reach young adults in their communities to educate them about health insurance, how to enroll in the Marketplace, where to go for enrollment assistance, and information about subsidies.
- Coordinated young adults campaigns. Along with more than 75 partnering organizations, Enroll America, Young Invincible, and Out2Enroll are announcing four targeted campaigns for the 2017 Open Enrollment. These campaigns are aimed at reaching the broad population of young adults, community college students, young families, and LGBTQ youth. To help focus these efforts, the White House will host a National Millennial Health Summit on September 27, 2016.
The press release goes into quite a bit more detail on each of these programs/initiatives, but you get the idea. How effective will it all be? I have no idea, but it certainly shouldn't hurt.
Oh, one more thing: Every once in awhile, a new survey/report will come out claiming the "Uninsured Rate in America" to be some percentage or another. This percentage can have a pretty wide range depending on your source; Gallup's latest survey lists it as 11.0% as of the end of March 2016, while the CDC's National Health Interview Survey had it as low as 9.1% as of last fall.
Obviously there are a lot of variables at play here, including the different dates (NHIS was from before 2016 open enrollment; Gallup is from after it ended), methodology, the wording of the question and so forth. However, the single biggest detail to look for in my book is always whether the survey includes children and senior citizens or not (as well as whether it includes undocumented immigrants).
To illustrate this, here's a graph from CMS's "Young Adult Outreach" entry which shows the uninsured rate of everyone in the country by how old they are:
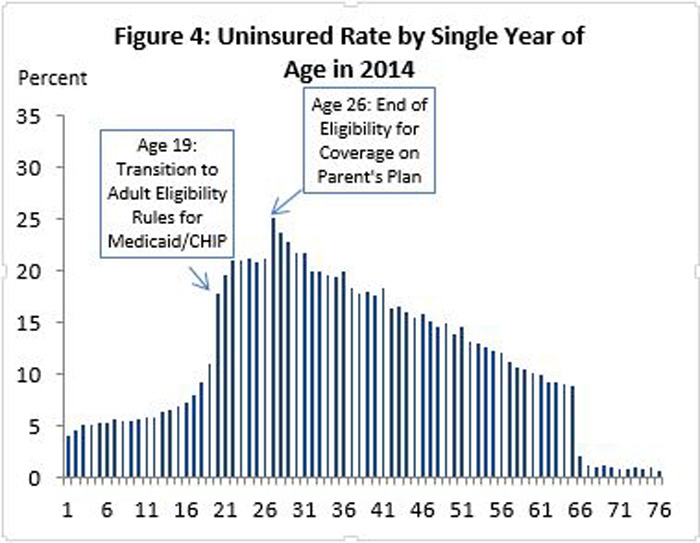
CMS used this to illustrate the importance of targeting young adults, and I agree...but it also serves to illustrate my point above. Notice how the uninsured rate hovers in the 5-10% range for children under 18, then shoots up to the 18-25% range for young adults (who, ironically, are themselves between around 18-25) before gradually dropping off to around 10% again as people hit their mid-60's...and finally, plummets off a cliff to just 1-2% for those over 65, as Medicare kicks in.
If you don't include children under 18 or seniors over 65, you're obviously going to come up with a much higher uninsured rate than if you include everyone.



