2023 Open Enrollment is over...but many people can still #GetCovered!

The 2023 ACA Open Enrollment Period has now officially ended in every state.
However, as I keep noting, there's still plenty of people who are eligible to enroll in ACA healthcare coverage during the off-season (thanks to Louise Norris for providing some of the links below):
MOST STATES: If your household income is less than 150% of the Federal Poverty Level (or higher in some states), you can enroll year-round:
In September 2021, the U.S. Department of Health & Human Services finalized a new special enrollment period (SEP) in states that use HealthCare.gov (optional for other states), granting year-round enrollment in ACA-compliant health insurance if an applicant’s household income does not exceed 150% of the federal poverty level (FPL) and if the applicant is eligible for a premium tax credit (subsidy) that will cover the cost of the benchmark plan.
This SEP became available on the HealthCare.gov website — and enhanced direct enrollment entity websites — as of March 21, 2022 (it was available prior to that only by calling the HealthCare.gov call center and completing the application over the phone). Outside of the annual open enrollment period (November 1 through January 15), applicants need to select “see if you can enroll” and then select the option that says “Medicaid, CHIP, or a new Special Enrollment Period based on income.” The prescreener tool will then ask questions to determine whether the person/household’s income is in the eligible range. If so, the special enrollment period opportunity will allow them to proceed with the enrollment. Enhanced direct enrollment entities have similar enrollment pathways.
In addition to the 33 states hosted via HealthCare.Gov, the 150% FPL SEP is also active in California, Colorado, Connecticut*, DC*, Kentucky, Maine, Massachusetts*, Minnesota*, New Jersey*, New Mexico*, New York*, Pennsylvania, Rhode Island, Vermont* and Washington*.
*In some states the year-round SEP income threshold is higher than 150%:
- Connecticut: Up to 175% FPL (Covered Connecticut)
- District of Columbia: Up to 215% FPL (Medicaid threshold)
- Massachusetts: Up to 300% FPL (ConnectorCare)
- Minnesota: Up to 200% FPL (MinnesotaCare)
- New Jersey: Up to 200% FPL
- New Mexico: Up to 200% FPL
- New York: Up to 200% FPL (Essential Plan)
- Vermont: Up to 200% FPL
- Washington State: Up to 250% FPL
I don't believe the 150% FPL SEP is available in Idaho, Maryland or Nevada; I'll update this if I'm wrong about this.
ALL STATES: Alaska Natives and members of federally recognized Native American tribes can enroll year-round:
Members of federally recognized tribes and ANCSA shareholders can enroll in a Marketplace plan any time. You can change plans up to once a month.
Special health coverage protections and benefits for American Indians and Alaska Natives
The Health Insurance Marketplace® benefits American Indians and Alaska Natives (AI/ANs) by providing opportunities for affordable health coverage through Marketplace health insurance plans, Medicaid, and the Children’s Health Insurance Program (CHIP).
Marketplace health insurance plans
While you’re not exempt from paying monthly premiums for an insurance plan you buy through the Marketplace, like all Americans you may qualify for tax credits that lower your premiums based on your income.
If you buy a Marketplace plan and your income is between 100% and 300% of the federal poverty level, you can enroll in a “zero cost sharing” plan. This means you won’t have to pay any out-of-pocket costs -- like deductibles, copayments, and coinsurance -- when you get care.
If you get services from an Indian Health Care Provider, you won’t have any out-of-pocket costs like copayments, coinsurance, or deductibles, regardless of your income. (This benefit also applies to Purchased and Referred Care.)
You can enroll in a Marketplace health insurance plan any time, not just during the yearly Open Enrollment Period. You can change plans as often as once a month.
ALL STATES: If you're eligible for Medicaid or the Children's Health Insurance Program (CHIP), you can enroll year-round:
Medicaid & CHIP coverage
Medicaid and the Children’s Health Insurance Program (CHIP) provide free or low-cost health coverage to millions of Americans, including some low-income people, families and children, pregnant women, the elderly, and people with disabilities.
Some states have expanded their Medicaid programs to cover all people below certain income levels.
Even if you don't qualify for Medicaid based on income, you should apply. You may qualify for your state's program, especially if you have children, are pregnant, or have a disability. You can apply for Medicaid any time of year — Medicaid and CHIP do not have Open Enrollment Periods.
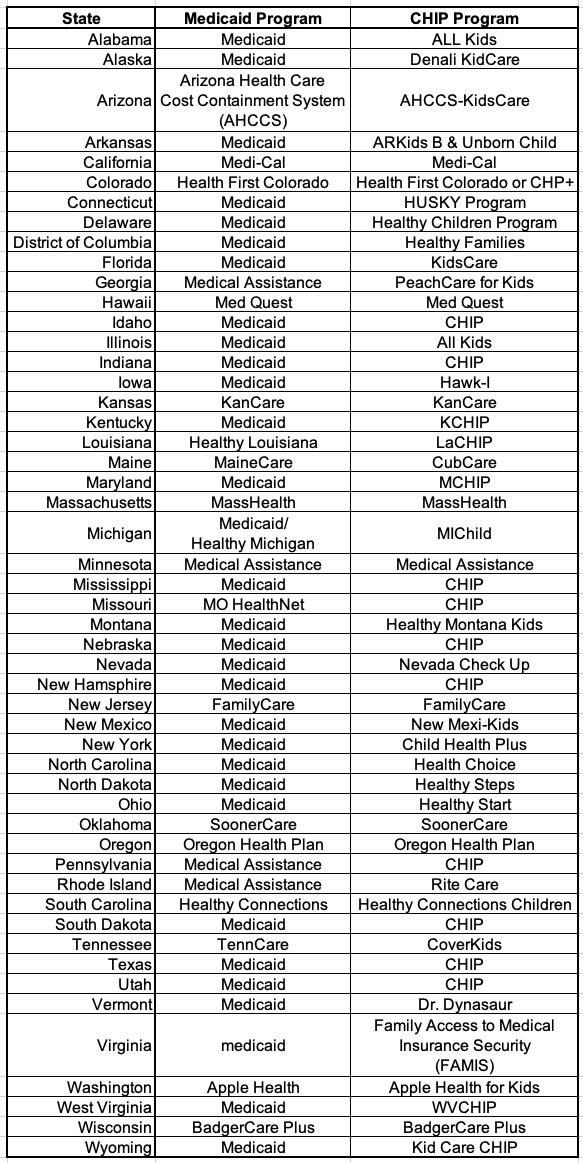
Medicaid & CHIP program names vary:
ALL STATES: If you have a Qualifying Life Experience (QLE), you may be eligible for a 60-day Special Enrollment Period. QLEs include:
- Lost qualifying health coverage in the past 60 days
- Expects to lose coverage in the next 60 days
- Got married
- Had a baby, or adopted/fostered a child
- Gained/became a dependent
- Got divorced or legally separated and lost health insurance
- Death of someone on your policy which caused you to lose coverage
- Changed your primary place of living
- Had a qualifying change in income
- Denied Medicaid or CHIP coverage
- Recently gained citizenship or lawful presence in the U.S.
- Was released from incarceration (detention, jail, or prison)
- Starting or ending service as an AmeriCorps State and National, VISTA, or NCCC member
- Employer offered to help with the cost of coverage either through an individual coverage HRA or QSEHRA
Easy Enrollment Programs via state tax return filing:
An easy enrollment program is a system that allows people without health insurance to check a box on their state tax return, giving the state department of revenue permission to share pertinent details with the state Medicaid office and health insurance exchange/marketplace. That information is then used to make a preliminary determination about whether the tax filer and their family members might be eligible for financial assistance with their health coverage – either Medicaid/CHIP or a premium tax credit (subsidy) in the exchange.
The state Medicaid office or health insurance exchange will then reach out to the tax filer, notify them of the coverage and financial assistance for which they may qualify, and provide enrollment assistance.
...The following states have enacted legislation to create easy enrollment programs:
- Maryland
- Colorado
- Massachusetts
- Pennsylvania
- Virginia (Medicaid/CHIP only for now)
- New Mexico (early 2023)
- New Jersey (launching in early 2024, for the 2023 tax year)
- Maine (launching in early 2024, for the 2023 tax year)
- California (launching in early 2024, for the 2023 tax year)
- Illinois (Medicaid/CHIP only for now)
MISCELLANOUS: Some states may have their own additional Qualifying Life Experiences which make you eligible for a SEP. For instance, in California, you're eligible if your household experienced a natural or human-caused disaster (such as wildfires) declared as a state of emergency. For that matter, you're also eligible during the COVID-19 National Public Health Emergency, currently set to expire on May 11th.
Unwinding SEP: As I noted last week, HealthCare.Gov announced that they'll be launching a 16-month "Unwinding SEP" for those who lose their Medicaid/CHIP coverage due to the end of the federal COVID-19 pandemic Medicaid "Continuous Coverage" provision (which allows states to start redetermining Medicaid/CHIP eligibility again starting on April 1st). Anyone losing Medicaid/CHIP coverage due to this is already eligible for a 60-day coverage loss SEP anyway; all this really means is that they don't have to apply within the first 60 days of losing coverage--they could theoretically wait until as late as July 31, 2024, although I can't imagine too many people would wait that long.