District of Columbia: Preliminary avg. 2021 ACA rate change: +3.8%; +1.9% for sm. group
The District of Columbia has joined Vermont and Oregon in releasing their preliminary 2021 Individual and Small Group market premium rate filings:
This page contains proposed health plan rate information for the District of Columbia’s health insurance marketplace, DC Health Link, for plan year 2021.
The District of Columbia Department of Insurance, Securities and Banking (DISB) received 188 proposed health insurance plan rates for review from Aetna, CareFirst BlueCross BlueShield, Kaiser Permanente and United Healthcare in advance of open enrollment for plan year 2021 on DC Health Link, the District of Columbia’s health insurance marketplace.
The four insurance companies filed proposed rates for individuals, families and small businesses for the 2021 plan year. Overall, 188 plans were filed, compared to 181 last year. The number of small group plans increased from 156 to 163, and the number of individual plans remained at 25.
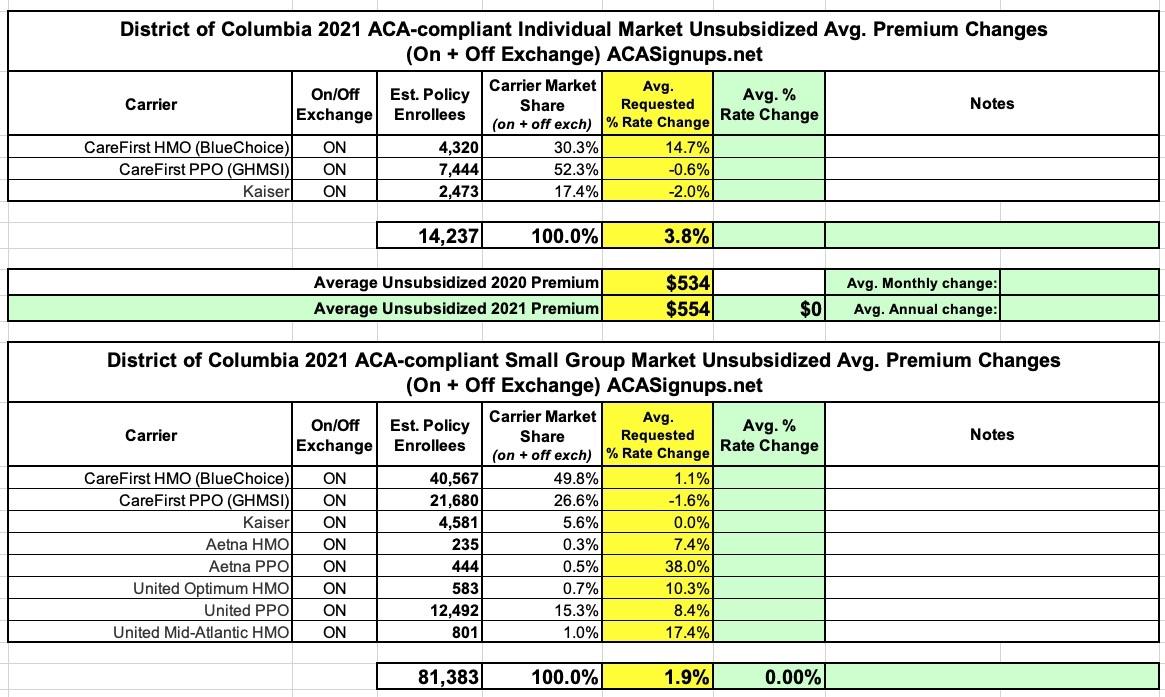
In the individual market, CareFirst proposed an average increase of 14.7 percent for HMO plans, and an average decrease of 0.6 percent for PPO plans. Kaiser proposed an average decrease of 2.0 percent. For small group plans, CareFirst filed average rate increases of 1.1 percent for HMO plans and an average decrease of 1.6 percent for the PPO plans. Kaiser small group rates proposed, on average, no change from the prior year. Aetna filed for an average increase of 7.4 percent for HMO plans and 38.0 percent for PPO plans. Finally, United proposed an average increase of 17.4 percent and 10.3 percent for its two HMOs and 11.4 percent for its PPO plans.
Some of these are pretty standard, but that massive 38% hike for small group PPO plans is quite an eye opener...but it's important to note that they only appear to have 444 people actually enrolled in those plans. Here's the summary of each market...it comes to a weighted average increase of 3.8% on the individual market and just 1.9% for the small group market: