Colorado: Final approved unsubsidized 2018 rate hikes: 34.3%, 6 points due to CSR sabotage
When I last looked at Colorado's 2018 rate hike summary in early September, it appeared that they were looking at an overall average rate increase of either 33% or 41% without CSR reimbursement payments depending on your interpretation of a state DOI quote, or 26.7% assuming CSR payments are made. The confusion wasn't really cleared up much by the later announcement that Colorado is going with the "Broad Load" strategy for their "lost" CSR reimbursements.
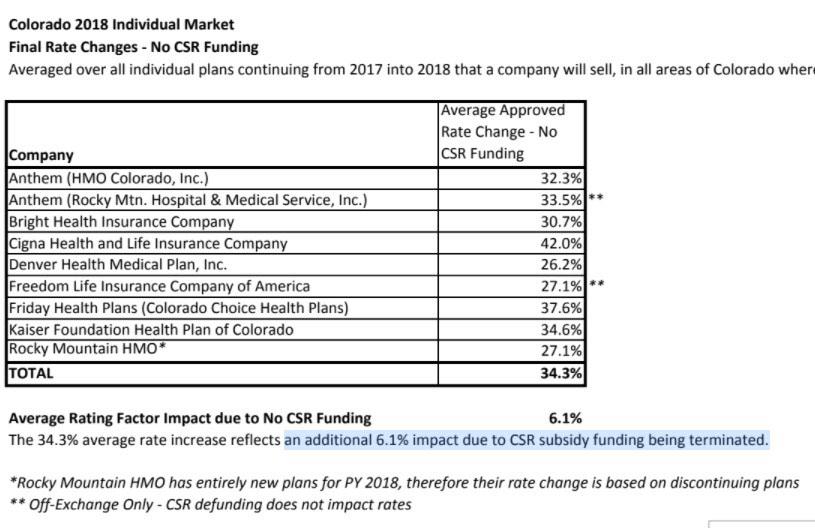
Today I checked in with the Colorado DOI again, and they've posted the official, presumably final rate increases, assuming no CSR funding:
If you subtract the 6.1 CSR load points, you get 28.2% overall w/out any CSR load vs. 34.3% with the CSR load added across the board.
It's important to note that carriers which don't have any on-exchange offerings also don't have any CSR load here even though Colorado is a "Broad Load" state, which just confuses the issue even further for some, I'm sure...
Related to this, Connect for Health Colorado, the state's ACA exchange, issued a press release the other day with a curious passage (h/t Hannah Recht & Jay Norris for the catch):
DENVER — Connect for Health Colorado opens for business Wednesday, November 1, with an improved customer support tool and an urgent message to consumers: Check your options, you may be surprised.
“We know the current climate has been confusing for many of our customers and stakeholders,” said Connect for Health Colorado Chief Executive Kevin Patterson. “The bottom line is the story is the same. Everyone who buys their own insurance can benefit from taking time to review the health plan options available to them and to check their eligibility for financial help.
“Too many people assume they make too much to qualify for help with the cost of insurance. That is like ‘leaving money on the table.’ It only takes a minute to check at ConnectforHealthCO.com. And even consumers who do not qualify for the help reduce the increase in their premiums by looking at comparable plans in their area. I am urging everyone to ‘stop, shop and enroll’ by December 15.”
Open Enrollment runs from November 1, 2017, to January 12, 2018 but consumers need to enroll by December 15 to have coverage in place by January 1, 2018.
The state Division of Insurance (DOI) has calculated that, on average, premiums will increase 33% in 2018. But because the level of assistance increases as premiums rise, the average net premium (what consumers pay after assistance) will go down 20%.
Connect for Health Colorado shoppers will find an improved Quick Cost and Plan Finder Tool that helps them estimate their out-of-pocket costs including prescription costs in the coming year, relying on claims data from the All Payers Claims Database maintained by the Center for Improving Value in Health Care. They will also find streamlined user experience within the award-winning tool that allows them to complete their estimates and comparisons in half as many screens.
Hmmmm...technically the state DOI calculated the unsubsidized average increase at 34.3%, not 33%, but the discrepancy might be because C4HCO isn't concerning themselves with "Anthem (Rocky Mountain Hospital & Medical)" or "Freedom Life" (which is a phantom carrier anyway).
The larger head-scratcher is the second part: "avg. net premium will go down 20%". I'm not sure I follow this.
If Colorado was a Silver Switcharoo state, this might be feasible...but since they're a "Broad Load" state, I can't see any way that anyone is gonna see their net premiums drop by 20% for the same policy next year:
- Subsidized enrollees will see their unsubsidized rates go up about 33% on average...and their subsidies should also go up about 33%, so they should pay about the same.
- Unsubsidized enrollees will see their unsubsidized rates go up about 33% on average...and that's it. A 33% price hike, ouch.
It's possible I'm missing something here, of course; Louise Norris (who lives in Colorado herself) is on the case and will hopefully be able to explain this soon...