Michigan: HAP ain't happy...with Trump's CSR/mandate sabotage. They're out.

Just a few days ago I noted that Michigan's Dept. of Insurance issued the semi-final 2018 individual market rate changes for the 10 carriers offering indy policies in the state (9 of which are on the ACA exchange; one of them is only offering plans off-exchange). At the time, the breakout was roughly 16.8% average increases assuming CSR payments are made next year or 26.8% assuming they aren't made.
Just moments ago, however, the Detroit News reported that Health Alliance Plan (HAP) is out at the last minute:
A major health insurer is leaving Michigan’s individual marketplace, ending its policies offered here under the Affordable Care Act as the federal government slashes funding for enrollment and outreach groups.
Health Alliance Plan said Friday it has withdrawn individual plans it expected to sell on the Michigan exchange. The decision will affect about 9,100 customers, according to the Detroit-based insurer, which previously asked the state to approve an average 24 percent rate increase for 2018.
HAP cited a variety of motivations for its withdrawal. They included uncertainties over rate premium stabilization programs, along with questions over the individual insurance mandate and cost-sharing insurer payments President Donald Trump’s administration has threatened to end amid continued debate over repealing and replacing the federal health law.
The article also gives a local angle to the other Trump Admin sabotage of the ACA: The massive advertising/outreach budget cuts:
...The HAP announcement came less than two months before the open enrollment period begins Nov. 1. It is the second insurer to withdraw from the state marketplace for 2018, when overall premiums are expected to rise nearly 28 percent. Alliance Health and Life Insurance Company did not file any on-exchange plans with the state.
...Enroll Michigan, which also hands down funding to 28 smaller groups, said its budget was cut 90 percent from $1.2 million to $129,899 for the 2018 grant year. Funding for the ACCESS nonprofit was cut 36 percent from $555,000 to about $352,000.
This announcement doesn't really change the average rate increase statewide since the numbers are relatively small...but it does raise one bit of confusion: According to their SERFF filing, HAP has over 25,500 ACA-compliant individual market enrollees total...but the News article says this will only impact around 9,100 people. The only way this makes sense is if HAP is if about 2/3 of their indy enrollees are off-exchange and they're doing what Alliance Health did: Dropping off the exchange but sticking around off-exchange. THat would look something like this:
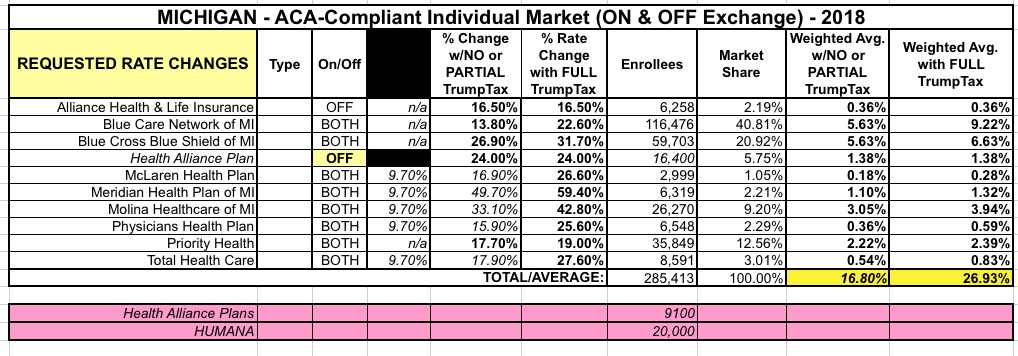
I'll have to clarify this confusion, but in the meantime, the Trump Sabotage Effect strikes again...this time in my home state.
How to support my healthcare wonkery:
1. Donate via ActBlue or PayPal
2. Subscribe via Substack.
3. Subscribe via Patreon.



