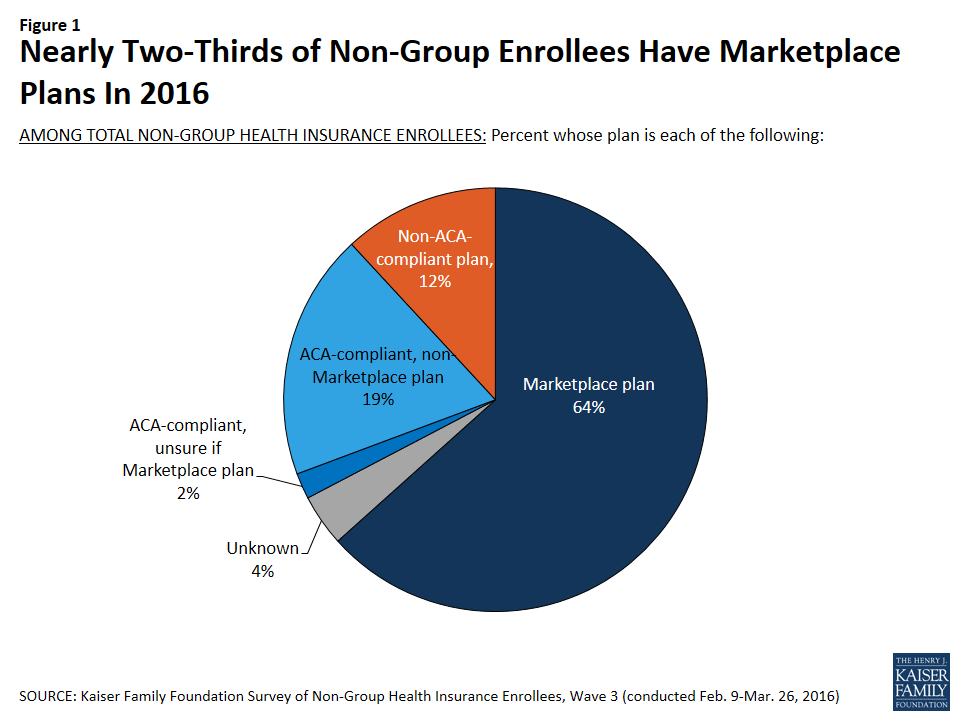Kaiser Family Foundation: Survey Says...
The Kaiser Family Foundation has just released their 3rd Annual survey of people enrolled in the "Non-Group Health Insurance Market", otherwise known as the Individual market. It's important to note that this survey includes Americans enrolled in all individual market plans, both on and off-exchange. There are technically 5 separate categories, although they can effectively be merged into three categories for most purposes:
- 1. EXCHANGE-based QHPs (Qualified Health Plans)
- 2a. OFF-Exchange QHPs
- 2b. OFF-Exchange ACA-compliant non-QHPs
- 3a. OFF-Exchange NON-ACA compliant "Grandfathered" plans (ie, enrolled in prior to 2010)
- 3b. OFF-Exchange NON-ACA compliant "Transitional" or "Grandmothered" plans (ie, enrolled in between 2010 and 2013)
I tend to merge #2 & 3 together (off-exchange, ACA-compliant) in virtually all cases, and merge #4 & 5 together (grandfathered/grandmothered) except in cases where I need to make a distinction.
First, KFF's methodology:
The survey was conducted by telephone from February 9 through March 26, 2016 among a random sample of 786 adult U.S. residents who purchase their own insurance. Computer-assisted telephone interviews conducted by landline (293) and cell phone (493 including 302 who had no landline telephone) were carried out in English and Spanish by SSRS. Respondents were considered eligible for the survey if they met the following criteria:
- Between the ages of 18-64
- Currently covered by health insurance that they purchase themselves or purchased insurance that would begin in the next month
- Not covered by health insurance through an employer, COBRA, Medicare, Medicaid, a parent’s plan, or the U.S. military or VA
- If a small business owner, the health insurance they purchase is only for themselves and/or their family, and does not cover non-related employees of their business
In other words, this should be pretty representative of the indy market nationally, although not including children probably skews the results a bit. However, they go on to say that they performed several types of weighting for various factors, so that isn't likely too much of a factor.
With that in mind, let's dig in!
The first thing which caught my eye was this: They didn't even bother asking how many people are "Newly Insured via the ACA exchanges" this year.
In 2014, this was a huge talking point for ACA critics, so much so that I got into a huge debate with Avik Roy in the crazy final weeks of the 2014 Open Enrollment Period, with him insisting that only 27% of exchange enrollees were newly insured, while I explained that it was likely to turn out to be more like 50%. As it turned out, not only was I right, but it was even higher than that: KFF's 2014 survey showed that 57% of exchange enrollees were newly-covered.
In 2015, KFF found that 26% of all individual plan enrollees were previously uninsured, but this included the off-exchange market, which made up around 40% of the total. There's no way of knowing whether that 26% was evenly distributed between the two, so there's no easy way of adjusting it to get the on-exchange percentage. HOWEVER, the CommonWealth Fund did ask the "exchange-based newly insured" question in their survey, and came up with 53% being previously uninsured in 2015. The percentage dropping actually makes sense because the total number of exchange enrollees was larger:
- 57% of around 7.1 million paying exchange enrollees in 2014 = roughly 4.1 million newly-insured exchange enrollees
- 53% of around 10.2 million paying exchange enrollees in 2015 = roughly 5.4 million newly-insured exchange enrollees
So, 4.1 million gained coverage for the first time via the exchanges in 2014, and an additional 1.3 million who had been previously uninsured gained coverage via exchange policies in 2015.
For 2016, I expected the net increase in "newly covered" specifically via exchange-based policies to shrink further, to perhaps 51% of total exchange enrollees this year (ie, around 5.8 million out of 11.3 million paying enrollees...a net increase of perhaps 400,000 more "previously uninsured" people). However, Kaiser didn't even bother asking the question this year...probably because the actual wording of the question was based on them being previously uninsured "for two years or more". Three years in, it starts to get into a very fuzzy area (what if you were uninsured in 2013, enrolled in an exchange plan in 2014, uninsured again in 2015 and enrolled in an exchange plan in 2016??)
OK, enough with what they didn't ask; here's what they did:
Looking at the non-group market as a whole, nearly two-thirds of enrollees (64 percent) report being in a Marketplace plan.3 This is similar to the share who had Marketplace plans in 2015 (59 percent) and an increase from 2014 (48 percent). Currently, about one in five enrollees (19 percent) report being in an ACA-compliant, non-Marketplace plan purchased from a broker or insurance company, and 12 percent report having pre-ACA, non-compliant plans.4
It's important to remember that the survey was done between mid-February and late March, and included people whose policies wouldn't actually go into effect until April. That means that while 12.7 million people selected exchange policies by the end of January, the survey presumably didn't include people whose policies were cancelled/never effectuated due to non-payment or for other reasons. This should mean that the exchange-based total utilized as part of the survey pool was around 11.3 million people nationally, but could potentially include all 12.7 million, since some people may not have known that their policy was cancelled yet.
Now, 6% of those surveyed either weren't sure whether their ACA-compliant policy was exchange-based or not (2%), or had no idea whether it was even compliant (4%). This means marketplace plans make up anywhere from 64% to 70% of the total individual market. Those 6% can also make a big difference in further breaking out the off-exchange policy estimates, but for the moment, here's how the total individual market adds up under all 4 scenarios:
- Using 12.7 million (64% exchange-based): Total market of 19.8 million; 7.1 million off-exchange
- Using 12.7 million (70% exchange-based): Total market of 18.1 million; 5.4 million off-exchange
- Using 11.3 million (64% exchange-based): Total market of 17.7 million; 6.4 million off-exchange
- Using 11.3 million (70% exchange-based): Total market of 16.1 million; 4.8 million off-exchange
Every other data source I've seen strongly indicates that the total individual market is at the higher end of this range (19-20 million total), which would suggest the top scenario. If so, however, that also means that the off-exchange number (7.1 million) would in turn break out as follows (with an irritatingly-high "Unknown" factor):
- 56.8% ACA-compliant (4.0 million)
- 32.4% Non-compliant (2.3 million)
- 10.8% Unknown (0.8 million)
In any event, this suggests that I was pretty close in my estimate of the total off-exchange market when I ran my "Show Your Work!" pie chart last month (I had it pegged at 7.2 million off exchange), but that I was way off in the compliant/noncompliant ratio (I figured it was around 6 million compliant vs. 1.2 million noncompliant). On the other hand, I had also given a noncompliant range of 1.9 - 2.8 million noncompliant in a separate analysis, so there's obviously a lot of unknowns and variables here.
The good news is that within another year or two, all of the remaining non-compliant plans (both "grandfathered" and "grandmothered") should be completely gone anyway, leaving us with just 2 categories: On exhange and Off exchange. It will be interesting to see if on-exchange enrollments continue to grow as a percentage of the total individual market. I could see it hitting perhaps 75% of the total market over the next few years before plateauing.
There's a whole mess of other data nerd goodness to be found in this year's KFF survey, much of which has to do with satisfaction ratings (how happy are you with your plan, with your network, etc) and the like. The big takeway is, as Larry Levitt put it:
ACA marketplace enrollees like their coverage, but they like others are getting cranky about the cost. https://t.co/TZLN01zeSz
— Larry Levitt (@larry_levitt) May 20, 2016
The biggest problems, as you'd expect, have to do with cost. In 2014, only 1/3 of all enrollees were complaining about their premiums or deductibles; that's now up to around 45%. Even when you look at exchange-based enrollees only (most of whom receive APTC assistance and about half of whom receive CSR assistance), the grumbling has grown from around 30% up to 43%:
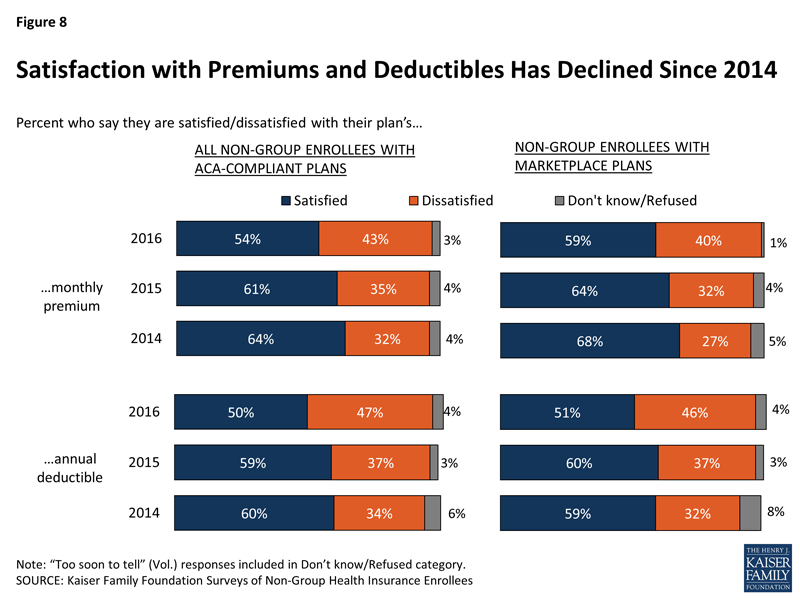
One other interesting thing I noted from the graph above: People are starting to familiarize themselves with what's "typical" when it comes to insurance costs. Note that in 2014, anywhere from 4-8% of all survey respondants didn't have any idea whether they should be "happy" or "upset" with what they were paying in premiums or deductibles. This year, the range is only from 1-4% in all categories. I don't know if this means that more have decided that they're happy or unhappy, but at least they've come off the fence on the issue.
What else? Lessee...well, unfortunately, for all the complaining about high deductibles, there's a depressing lack of education about the free services which are included with every ACA-compliant plan:
The survey also finds a lack of awareness about new rules for coverage introduced by the ACA. Among all those with ACA-compliant coverage, fewer than half (47 percent) know that preventive services are covered completely by their plans, while a third (33 percent) think that copays or deductibles apply to preventive services and one in five (20 percent) are not sure. Among those in high-deductible plans, awareness is even lower: 41 know that preventive services are covered with no cost-sharing.
This is a facepalm-inducing paragraph. One of the major reasons the ACA exchange plans were set up this way was specifically to help promote preventative care, to avoid a simple problem today turning into an expensive problem later on. If people don't know these services (such as vaccinations, blood pressure screenings, mammograms, etc) are free, they're likely to avoid taking advantage of them since they think they'll have to pay for them, which defeats the whole point.
On the technical side, the exchange websites have continued to improve significantly, not just in terms of setting up an account but also the new features added this year like the Network and Formulary tools:
Among those with Marketplace coverage, most say that when they were shopping for their current plan, it was easy to compare premiums, cost-sharing, and provider networks, and to find a policy to meet their needs. While most measures of the shopping experience are similar to 2015, among those with Marketplace plans, the share saying it was difficult to set up an account with the marketplace decreased from 34 percent in 2014 to 25 percent this year.
At first, I was surprised that only 34% said it was difficult to set up an account back in 2014 given the ugly launch of the websites the previous fall...but then I realized that this was because almost no one COULD set up an account at all the first 2 months, and over 40% of 2014 enrollees didn't sign up until March or April anyway, so by the time they got around to even trying, the worst of the problems had already been taken care of.
Anyway, there's a whole mess of other interesting stuff here, but these are just some oddball items which jumped out at me. Here's one more amusing finding:
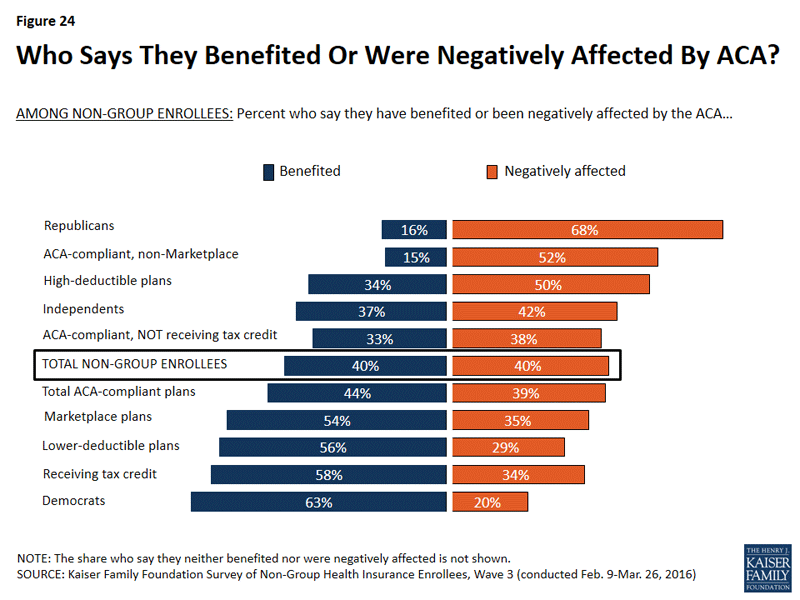
Imagine that: Exactly the same number of individual market enrollees think the ACA has helped them as think it has hurt them...and the split is almost entirely partisan.