ACA 2.0: South Carolina (SC-01): How much would #HR1868 lower YOUR premiums?
Last March I wrote an analysis of H.R.1868, the House Democrats bill that comprises the core of the larger H.R.1884 "ACA 2.0" bill. H.R.1884 includes a suite of about a dozen provisions to protect, repair and strengthen the ACA, but the House Dems also broke the larger piece of legislation down into a dozen smaller bills as well.
Some of these "mini-ACA 2.0" bills only make minor improvements to the law, or make improvements in ways which are important but would take a few years to see obvious results. Others, however, make huge improvements and would be immediately obvious, and of those, the single most dramatic and important one is H.R.1868.
The official title is the "Health Care Affordability Act of 2019", but I just call both it and H.R.1884 (the "Protecting Pre-Existing Conditions and Making Health Care More Affordable Act of 2019") by the much simpler and more accurate moniker "ACA 2.0".
The official lead sponsor of H.R.1868 is Rep. Lauren Underwood (IL-14). While it currently only has 35 cosponsors, the larger H.R.1884 bill that includes H.R.1868 has 160 total sponsors to date, so there's strong support within the Democratic caucus.
H.R.1868 itself is a very short and simple bill which does just two things, both of which involve changes to the current formula for ACA individual market subsidies:
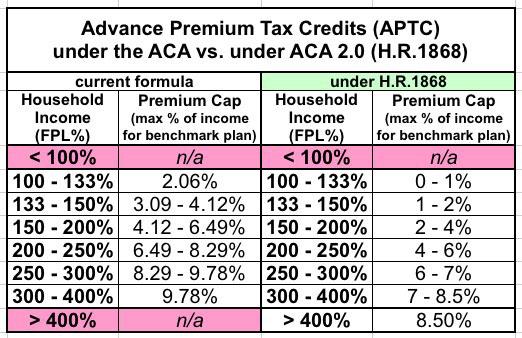
- First, it removes the current tax credit maximum income eligibility threshold of 400% of the Federal Poverty Line (around $50,000/year if you're single, or $100,000/year for a family of four).
- Second, it makes the underlying formula for the tax credits more generous: Instead of the maximum amount the enrollee has to pay for a benchmark Silver plan ranging from around 2.1% of their income up to around 9.8%, H.R.1868 would drop this down to between 0% - 8.5% of income at the outside.
This may not sound like much, but it would make a huge difference for millions of Americans. The main beneficiaries would be the middle class...people earning too much to qualify for subsidies today, but not enough to easily afford ACA-compliant policies (basically, between 400 - 800% FPL). However, many of those who are already receiving subsidies would also see additional savings.
It's important to keep in mind that there are three main trouble spots when it comes to the individual market under the ACA: Premiums (mostly for the unsubsidized); deductibles/co-pays (for those earning more than 200% FPL); and provider network width. H.R.1868 addresses the first of these three, and it does so very well.
There are other provisions in the larger "omnibus" ACA 2.0 bill (and especially in the Senate version, S.1213) which deal with the other two, but for this project I'm only looking at the first: High premiums.
When I ran the numbers for my March analysis of H.R.1868, I used the national average premiums for Silver plans, which cover around 70% of the average person's medical expenses per year. However, that premium can vary greatly from state to state, county to county, carrier to carrier and even by the specific Silver plan you're looking at.
The actual measure is to look at the benchmark plan for the specific geographic area that the enrollee(s) live in. Under the ACA, the benchmark plan is the second lowest-cost Silver plan available on the ACA exchange.
It's important to understand that in addition to where they live, the benchmark plan premium will also vary greatly depending on...
- The number of people living in the household; obviously it will be different for a single adult vs. a family of four.
- The age of the enrollees: Unless you live in New York or Vermont, a millennial will cost a lot less than a baby boomer.
- In some states, children under 18 are eligible for CHIP or Medicaid at lower income levels even if the parents aren't.
- In states which have refused to expand Medicaid, those who earn 100-138% FPL are also eligible for extremely generous private plan subsidies.
- In Alaska and Hawaii, the FPL threshold is higher than in the rest of the country.
Therefore, I've decided to launch a new project: I'm going to run the numbers for H.R.1868 for all 435 Congressional Districts.
In terms of methodology, the first challenge is the geography. Most states have multiple premium rating areas (that is, carriers can charge different rates for the same plan in one vs. another within the state); not every carrier offers plans in every part of the state; and of course there's no connection between the insurance rating areas and Congressional District boundaries (especially with some gerrymandered districts winding their way from one end of the state to the other).
My solution to this is to simply pick the zip code of each Representative's home town (there are nearly 42,000 zip codes nationally).
Second: I have to account for the wide variance of household makeups. There's an endless array of possibilities, but I settled on four specific households. Collectively, I think these are about as representative as I could reasonably be.
This is, needless to say, an extremely ambitious and time-consuming project. It'll take months for me to get to every district, assuming I even do get to all of them.
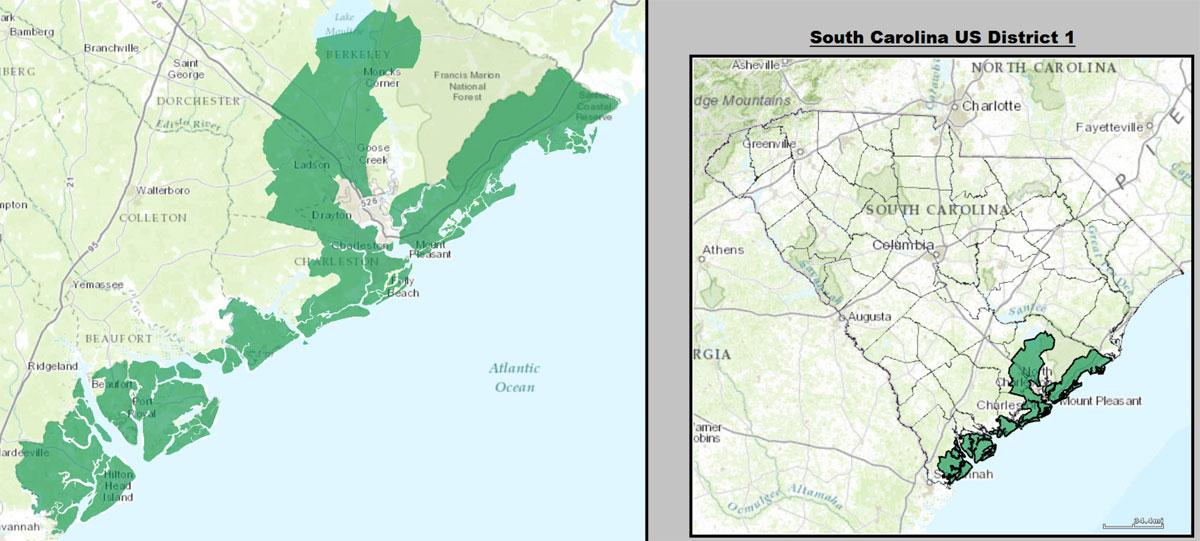
Today, I'm looking at South Carolina's First Congressional District. SC-01 stretches across the southeast coast of the state, and includes Charleston and Myrtle Beach, along with a bunch of coastal island communities. It's been represented by Democrat Joe Cunningham (who lives in Charleston) since 2019; he's the first Democrat to represent the area in decades:
First up: A single 30-year old:
IMPORTANT: This is the first time I've done one of these analyses for a district located in a state which hasn't expanded Medicaid. This makes a dramatic difference in the tables and graphs below, because anyone below the 100% FPL subsidy cut-off point would still be pretty much screwed under H.R. 1868.
There are other bills which have been introduced in the House which would help address that population as well, such as H.R. 584, which would encourage non-expansion states to go ahead and expand the program by providing 100% federal funding for the first 3 years regardless of when they do so, instead of the state having to contribute 10% of the cost of doing so right out of the gate. H.R. 1868 itself would not address the Medicaid expansion population, however.
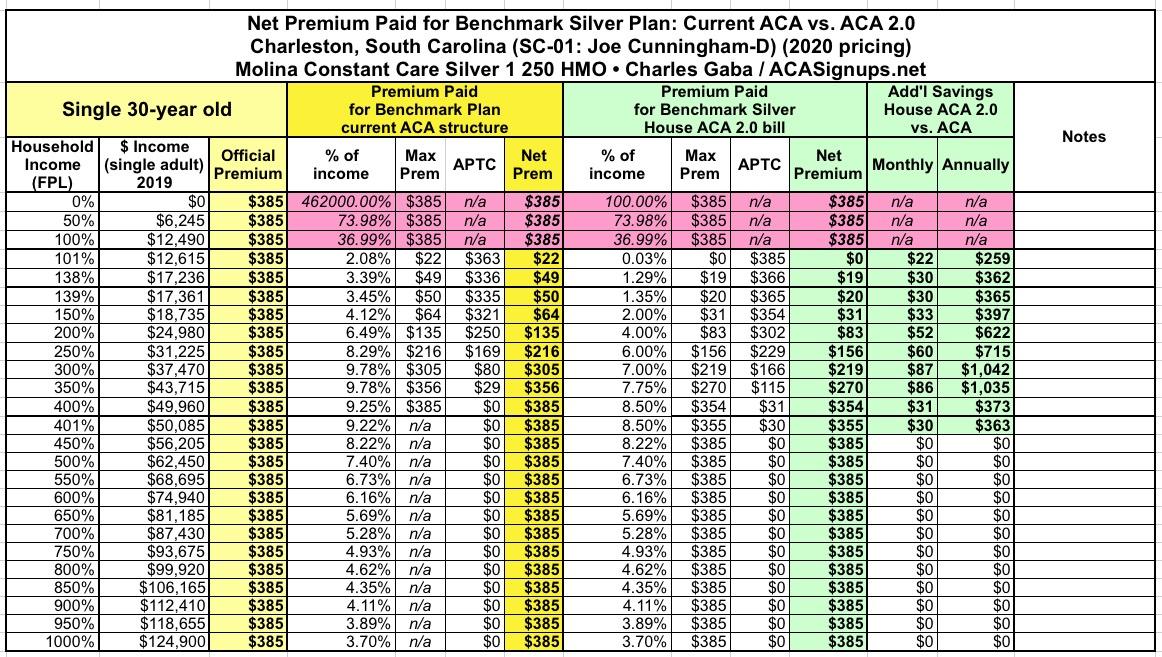
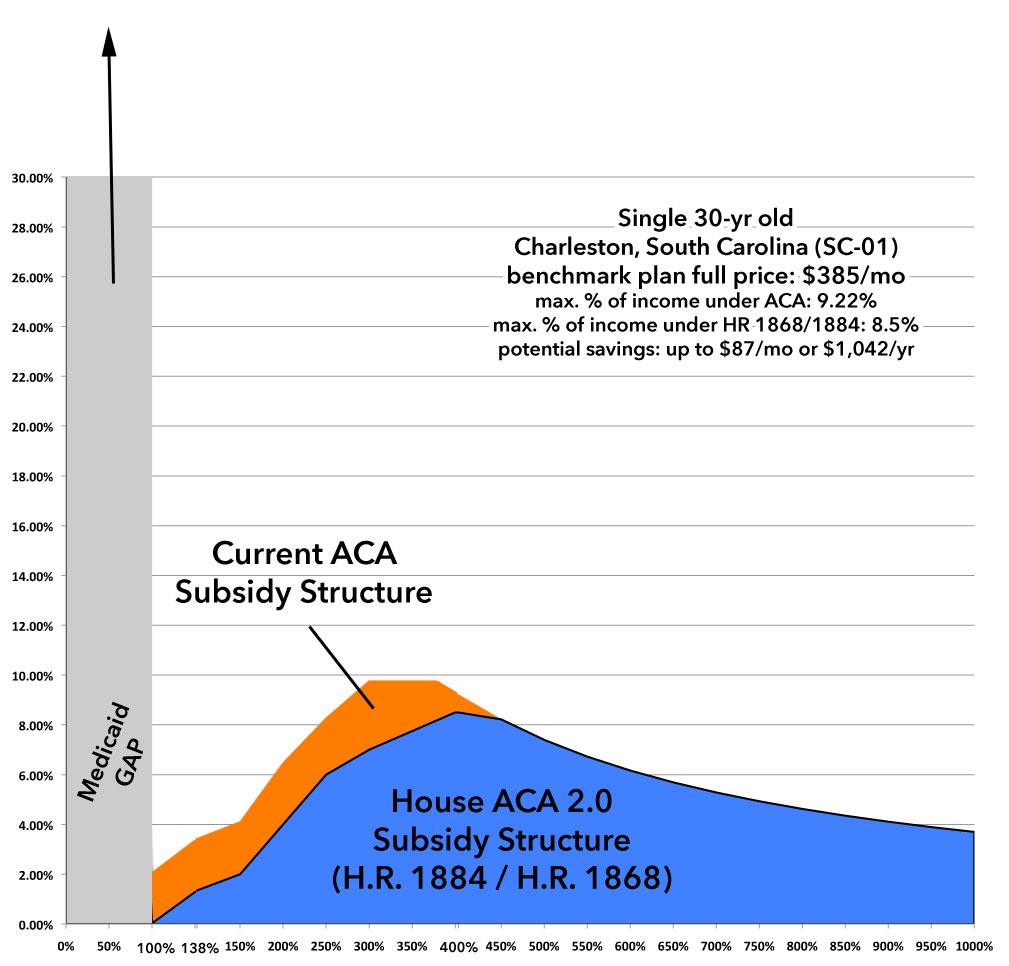
Without any subsidies, this young adult would be paying $385/month regardless of his or her income. Under the current ACA subsidy formula, at just over 100% FPL, their monthly premiums start at $22/mo, then gradually increase to the full $385/mo. Under H.R.1868, that $22/mo would baically drop down to $0/mo, and others in that range would save up to $87 more per month or $1,042/year. Those barely over 400% FPL would also save a nominal amount...around $30/month.
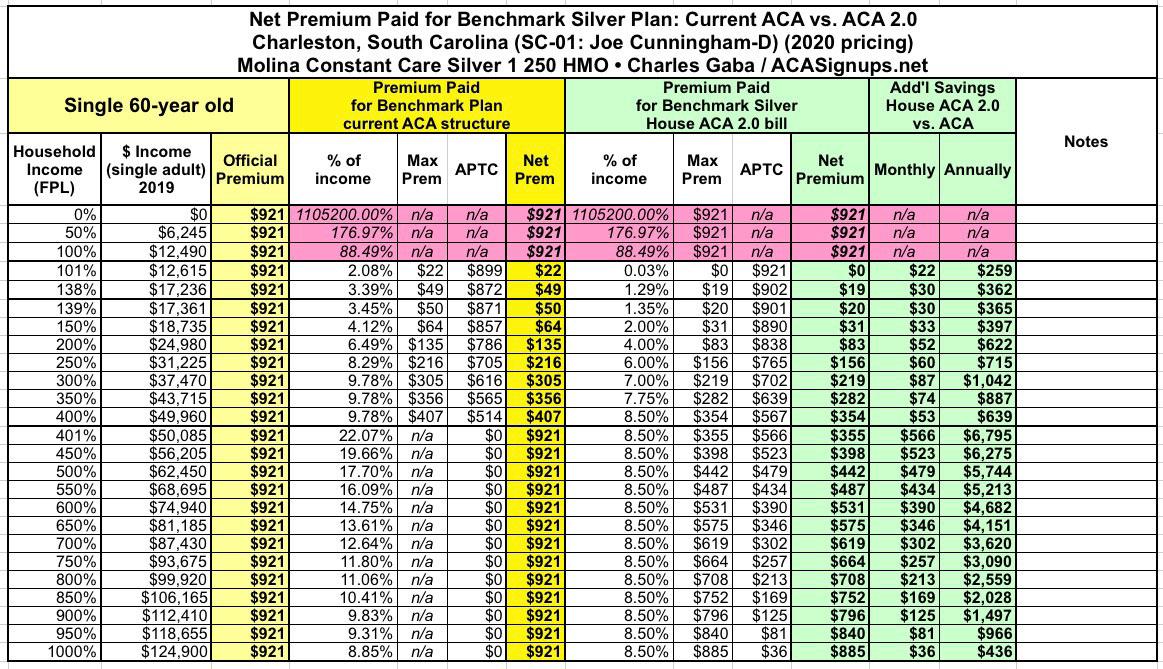
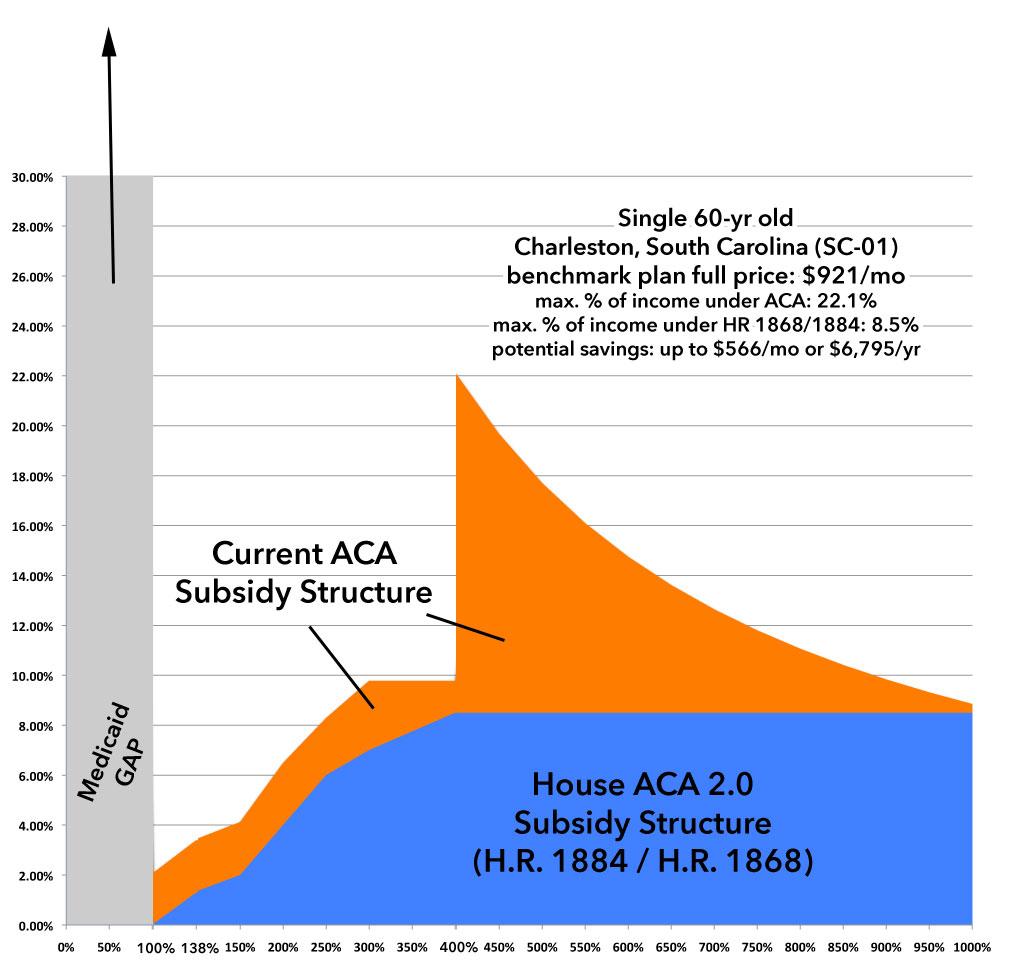
Next: A single 60-year old:
You can really see the Subsidy Cliff problem here. At 60 years old, they'd have to pay $921/month at full price...and with that 400% FPL cut-off, it eats up 22% of their income.
Under H.R.1868 / H.R. 1884, that would be cut down to just 8.5%, saving the enrollee up to $566/month or $6,800/year.
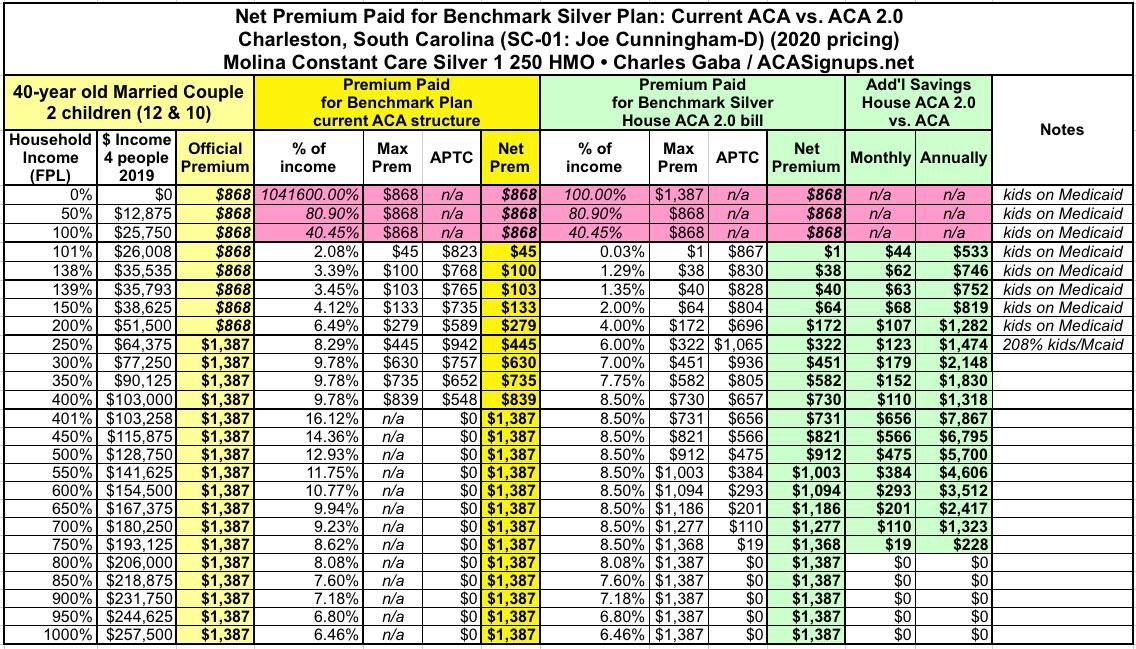
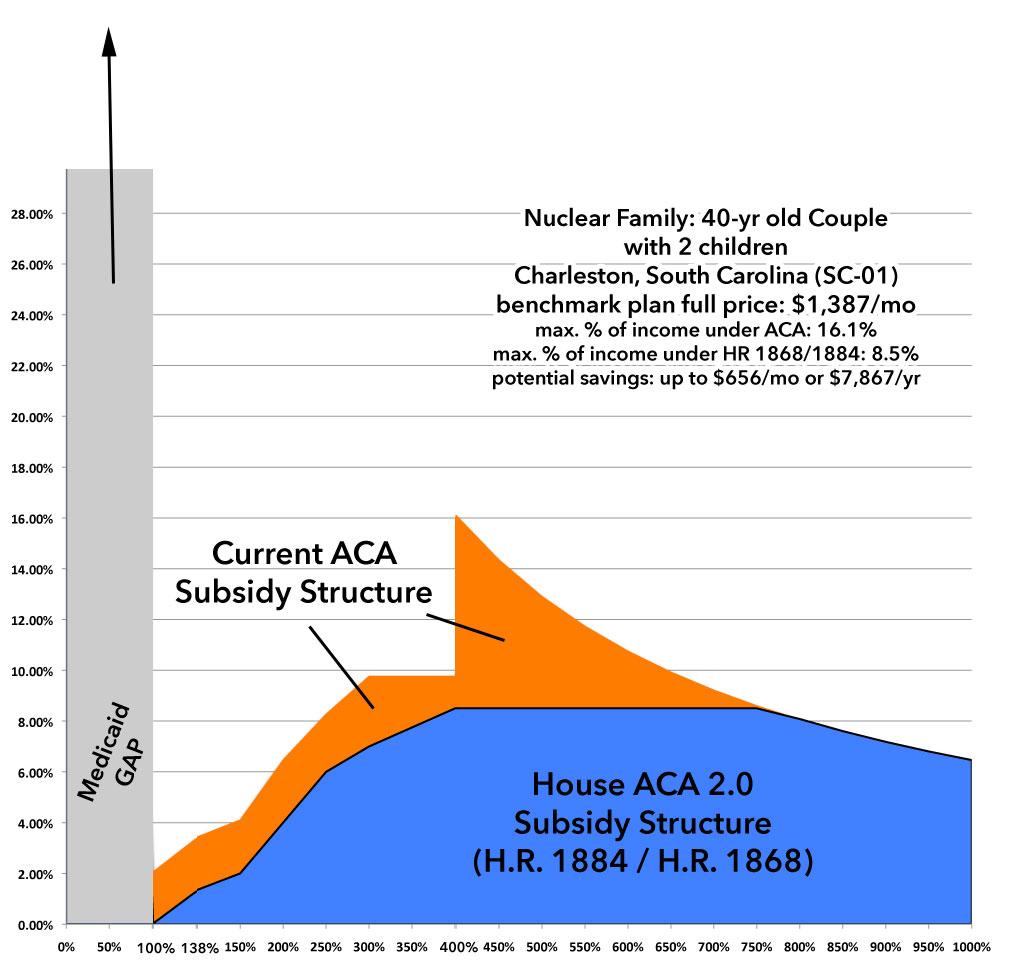
Nuclear Family: A 40-year old married couple with two children aged 12 & 10:
In South Carolina, the kids would be on CHIP until the family hits 200% FPL, or $51,500/yr in income, so the unsubsidized premium for the parents only would run $868/mo. Over that, it's $1,387/month for all four of them at full price.
Currently, once the family breaks the 400% threshold, premiums run as much as 16.1% of their income. Under H.R.1868 / H.R. 1884, this would drop to 8.5%, saving them as much as $656/mo or $7,867/year...and they'd still save up to $1,300 more per year even if they already receive assistance.
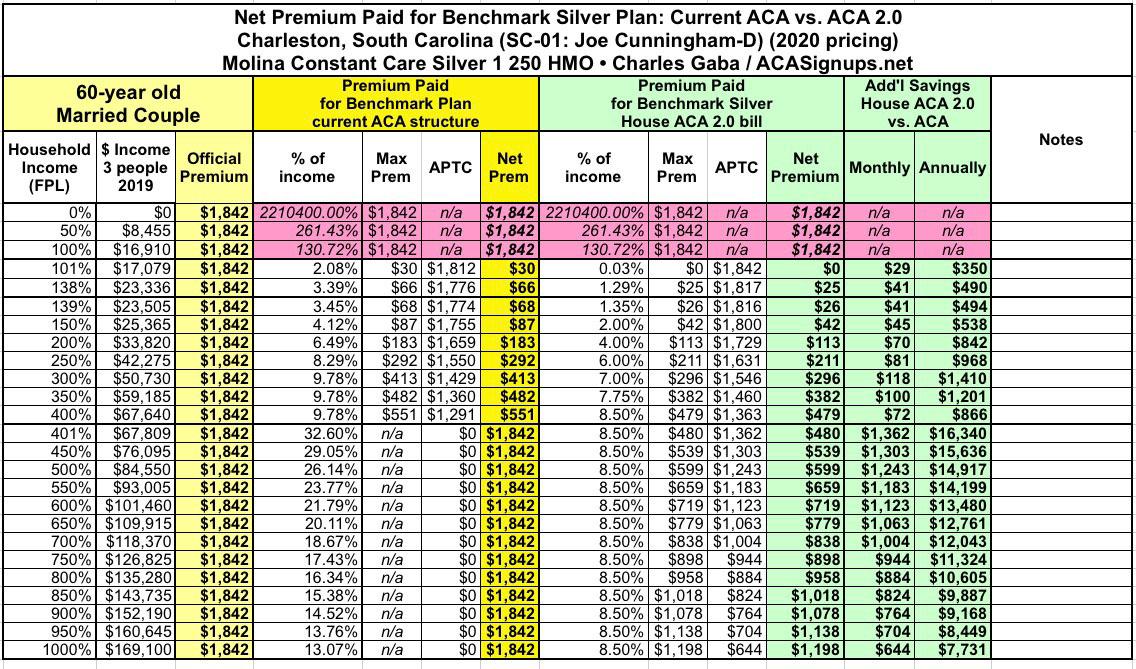
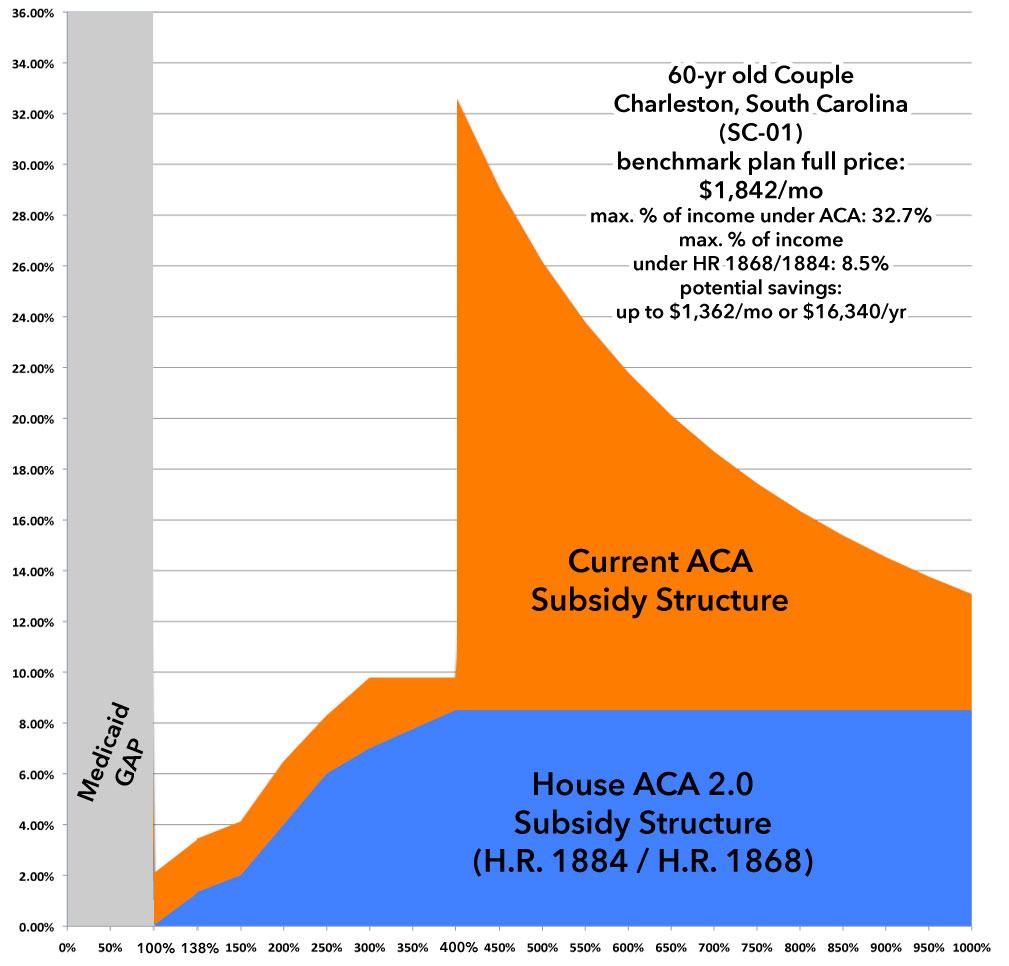
Finally, a 60-year old married couple:
Under the current ACA formula, if they earn between $68,000 and, say, $140,000/year, this couple is almost certainly not going to buy any ACA plan unless one of them has extremely expensive conditions...at full price they'd have to pay as much as 32.6% of their income in premiums alone. The Subsidy Cliff is now a Subsidy Chasm.
Under ACA 2.0, again, they'd pay no more than 8.5% in premiums, reducing their net premiums from $1,842/month down to as little as $480/month, a reduction of a whopping $1,362/month or over $16,300/year.