Vermont: Final OEP exchange enrollment down 12.3%...for a VERY good reason
At long last, the final piece of the puzzle can be added: I just received the final 2019 Open Enrollment Period numbers from Vermont Health Connect.
Before looking at it, it's important to understand that Vermont has a unique way of reporting ACA-compliant healthcare policy enrollments.
For the first two years of Open Enrollment, the state didn't allow any off-exchange (or "direct") enrollments for the individual market (or the small business market, I believe). That means all indy market enrollments were done through the exchange. Due to technical problems (and possibly for other reasons as well), however, starting in 2016 they started allowing direct/off-exchange enrollment as well, as every other state does (the District of Columbia is the only other ACA exchange which has no off-exchange market). However, Vermont still requires the insurance carriers to report those off-exchange enrollees to them and they report them as well.
I wish every state reported their enrollment data this way; it would make it much easier for me to do my job, since as it stands the off-exchange market is a bit of a mystery in most states.
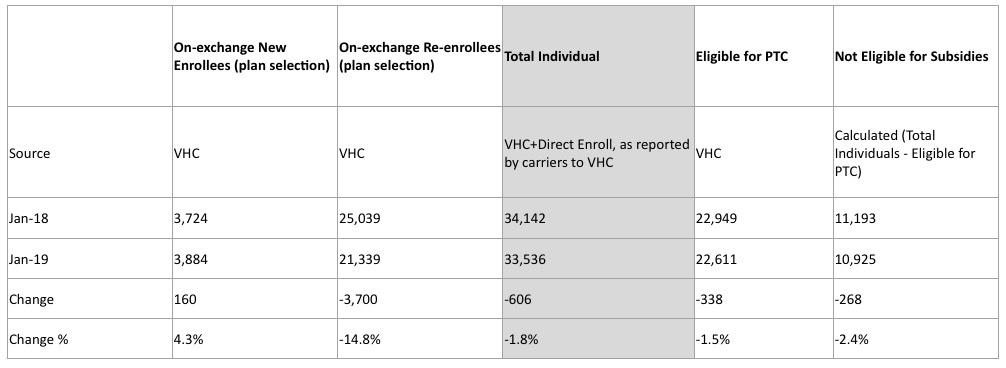
With that in mind, here's a table breaking out the year over year top-line numbers (more details should be forthcoming in the next week or two):
OK, so what's going on here? Well, on the surface, there were a total of 25,223 exchange-based QHP selections...down 12.3% year over year, or 3,540 people. Not good...in fact, this puts Vermont near the bottom of the list in terms of year over year performance, ahead of just Louisiana, West Virginia and Virginia. New enrollments are actually up 4.3% but re-enrollees are down 14.8%. Ouch.
HOWEVER, that's only half the story. When you include the off-exchange market, it's a very different picture. Last year, 5,379 people enrolled off-exchange (for a total of 34,142 QHPs both on+off). This year that number skyrocketd by 54% to 8,313 off-exchange enrollees. This means the total ACA-compliant individual market in Vermont actually only dropped slightly, by around 600 people or 1.8%.
On-exchange renewals dropped by 3,700 people...but off-exchange enrollment increased by 2,934.
Why? Simple: Silver Loading, or more specifically, the silver switcharoo:
An Open Letter to Everyone Who Has Helped Vermonters Get into the Right Health Coverage
As we enter the final week of Open Enrollment, the Department of Vermont Health Access wants to thank you for all you’ve done to help spread the word about this year’s changes. We also want to ask your help with a final push to get Vermonters into the ‘right plans.’
Due to a complex set of policy changes, the federal government is providing a lot more financial help in 2019. This means:
- A family of four earning $100,000 will receive over $3,000 more in financial help than they received in 2018;
- Most uninsured Vermonters have a household income that would now qualify for a zero-premium plan, meaning their financial help would cover their whole monthly premium;
- Many Vermont Health Connect members can save more than a thousand dollars by changing to a different ‘metal level’ insurance plan, per the 2019 Plan Comparison Tool.
With your help over the last few years, Vermont has achieved one of the lowest uninsured rates in the nation. With your help this week, we can drive it even lower.
...For Vermonters who are sure their income is too high to qualify for financial help, the ‘wrong plan’ can be a silver plan with Vermont Health Connect. On-exchange silver plans cost much more in 2019, so unsubsidized Vermonters are better off changing to a different metal level plan – for example, gold plans now have a similar premium to silver plans, but lower out-of-pocket costs – or enrolling in a lower cost “reflective silver” plan directly with Blue Cross Blue Shield of Vermont or MVP Health Care.
In other words, the Vermont exchange, which didn't do silver loading last year but is doing so for 2019, handled the Silver Switcharoo perfectly. Not only did they load all of the CSR costs onto on-exchange Silver plans exclusively, they also created "mirrored" off-exchange Silvers and made certain to ensure that unsubsidized Vermont residents KNEW about that option.
I cannot stress enough how important this last point is. Just like with Massachusetts' state-based individual mandate penalty, silver switching only works if people KNOW about it.
In Vermont's case, they made a concentrated effort to get the word out and it worked exactly as it should have: Several thousand people who were enrolled in on-exchange Silver plans shifted over to the virtually-identical off-exchange variant, saving hundreds or thousands of dollars for the exact same coverage. This makes it seem like VT had a crappy year...but in fact it was just people shifting from one category to another. The total risk pool is what matters.
This is also one reason why CMS Administrator Seema Verma trashing New Jersey for their 7.1% on-exchange enrollment drop in spite of them reinstating their own mandate penalty was extremely premature. Until New Jersey releases their off-exchange enrollment numbers (which they'll likely do in April), there's no way of knowing whether their total ACA indy market actually dropped or not. MAYBE that will still turn out to be the case...but we don't know yet. If NJ's off-exchange number increased by 19,500 people vs. last year, voila, that would completely cancel out their on-exchange drop.
How to support my healthcare wonkery:
1. Donate via ActBlue or PayPal
2. Subscribe via Substack.
3. Subscribe via Patreon.