Kentucky: New Gov. Bevin still promising to kill kynect, screw up Medicaid expansion
Here's what Democratic Kentucky Governor Steve Beshear's official "Healthier Kentucky" webpage looked like yesterday. Outdated, of course (no updates since the end of the 2015 Open Enrollment Period), but lots of data touting the thousands and thousands of people the Affordable Care Act (aka OBAMACARE, guys) has helped receive healthcare coverage via either private policies or Medicaid expansion:
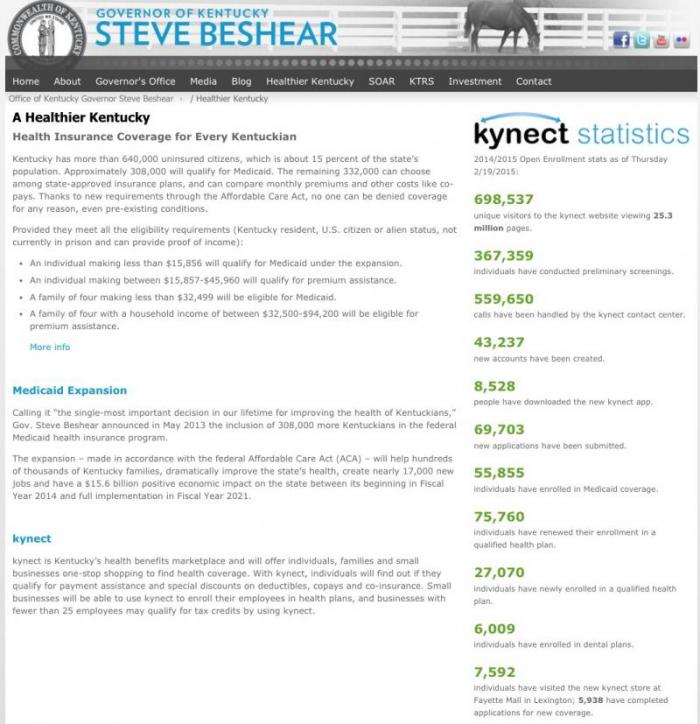
Here's what the same page looks like today.
Amusingly, BeShear's name and image are still in the upper-right corner, but other than that there's nothing funny about it.
Bevin now promising to shut down "redundant" Kynect program.
— Lawrence Smith (@LASmithReports) December 8, 2015
Shutting down kynect next year (assuming he's able to actually do so legally) would be a shame, but not devastating. I mean, Kentuckians love kynect, and it won't actually save any money or anything, but whatever; so one more state would join the MotherShip at Healthcare.Gov. However...
Bevin says he will copy best parts of Indiana's Medicaid program. Gov. Mike Pence is in attendance
— Lawrence Smith (@LASmithReports) December 8, 2015
Well, I guess that's better than kicking a half-million people under the bus completely, but what are these "Best Parts" of the Indiana program he means?
While all waivers involve some amount of administrative complexity, Indiana’s demonstration is more complex than others approved to date. The program has multiple parts, including four different Medicaid benefit packages for the populations covered by the waiver (aside from premium assistance for employer-sponsored insurance). It also requires administering and tracking a number of elements, such as premium payments or co-payments, compliance with healthy behaviors, health savings account balances and rollover funds, presumptive eligibility determinations, and services that would have been covered retroactively for certain groups. Beneficiaries are treated differently based on their coverage group, and beneficiaries within the same coverage group are treated differently depending upon their income level, medical frailty status, and whether they have paid premiums.
Oh. And here I thought Bevin was going to complicate things. What a relief.
In all seriousness, it's possible that bogging down the Medicaid program with all of these rules, restrictions and fees (seriously, a $1.00/month premium?) will indeed save the state a few bucks, but bear in mind that the state would only have to pay 10% of the program's cost at most under the ACA (the feds cover the other 90%). Even then, I'd have to imagine that the sheer cost of the red tape/paperwork/bureaucracy to track all of this nonsense would cancel out any savings anyway.



