Michigan: An Open Letter to Gov. Whitmer & state legislators: 36 Ways to Protect, Repair & Strengthen the ACA at the state level
Note: This isn't limited to Michigan...many of the items listed here could/should be applied in other states as well.
Dear Governor Whitmer & Michigan State House and Senate Members:
If you're familiar with me and this site, you probably know two things about me:
- 1. I strongly support achieving Universal Healthcare coverage, but I'm skeptical about single payer/Medicare for All, at least in the short term.
- 2. Having said that, until universal coverage is feasible at the federal level in one way or another, I strongly believe that it is vitally important to protect, repair and strengthen the Affordable Care Act even if it ends up being replaced by something else in the near future.
As I'm typing this up, the ACA is (once again) in jeopardy, due to an absurdly nonsensical lawsuit which, nonetheless, has managed to work it's way up to the 5th Federal Circuit Court of Appeals, and which will likely see its ultimate fate decided by the U.S. Supreme Court. This could happen as soon as this June...or as late as two years from now.
If the ACA is struck down without any serious replacement plan ready to take effect immediately, this would cause unbelievable turmoil and chaos across the entire U.S. healthcare system...including right here in Michigan. While the November election will play a major role in determining what happens with heathcare policy going forward, there's no guarantee that the ACA being saved will be a part of that.
The ACA is like a Swiss Army Knife...it has two big tools, plus a whole bunch of smaller ones which don't get a lot of attention (and some of them are too obscure for most people to even figure out what their purpose is). The tools people are most aware of are Medicaid expansion (known as "Healthy Michigan" here, of course) and the ACA exchange structure...which includes a suite of important protections for people with pre-existing conditions...many of which also apply to employer-based insurance coverage as well as ACA individual market policies.
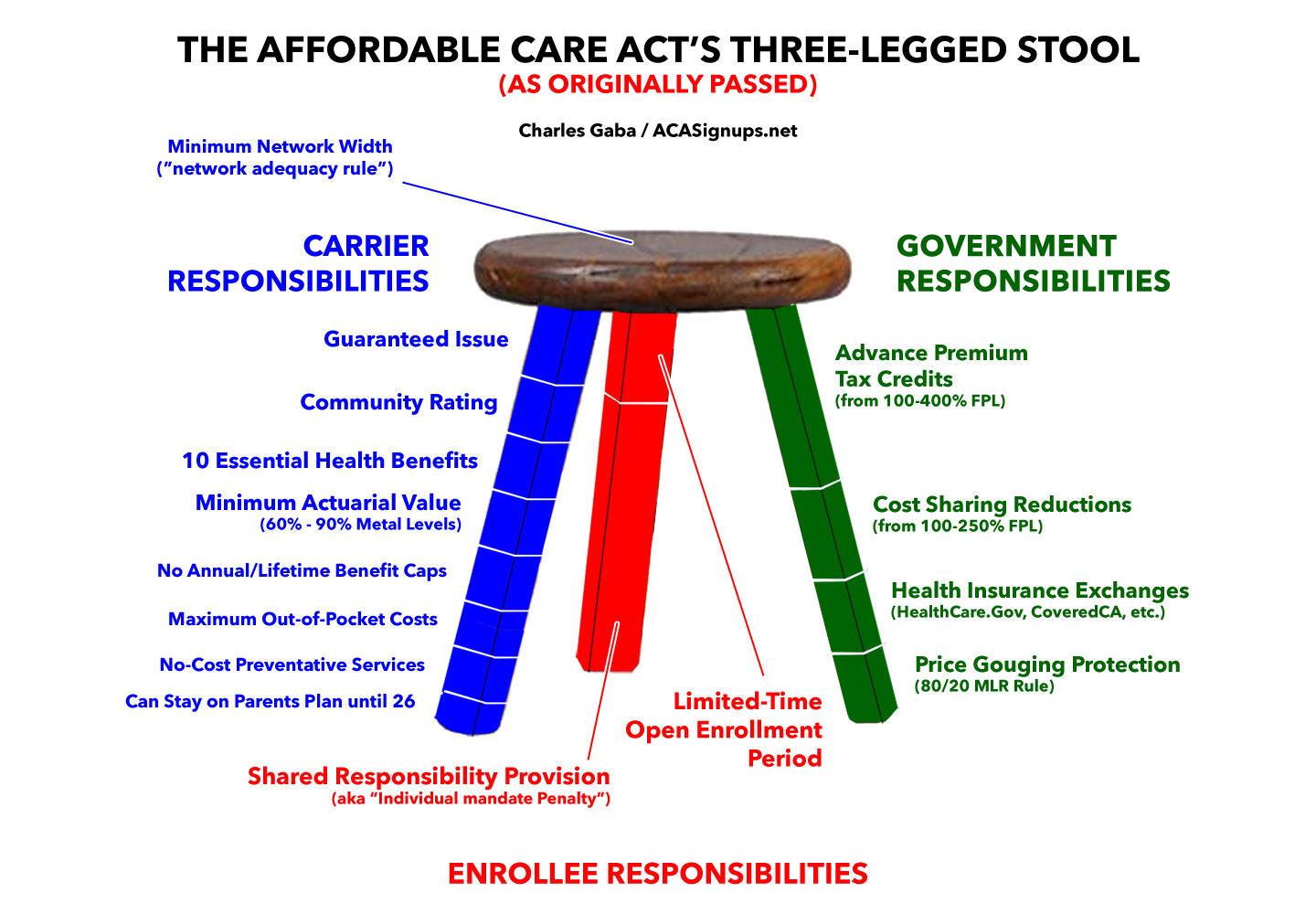
This structure is also known as the "Three-Legged Stool". While I didn't come up with the metaphor originally, I'm pretty well-known for popularizing it:
When people refer to "Protections for those with Pre-Existing Conditions", they're talking about most of the stuff in the blue leg of the 3-legged stool. These are the provisions which Gov. Whitmer was referring to in her State of the State address, and I'll define each of them below.
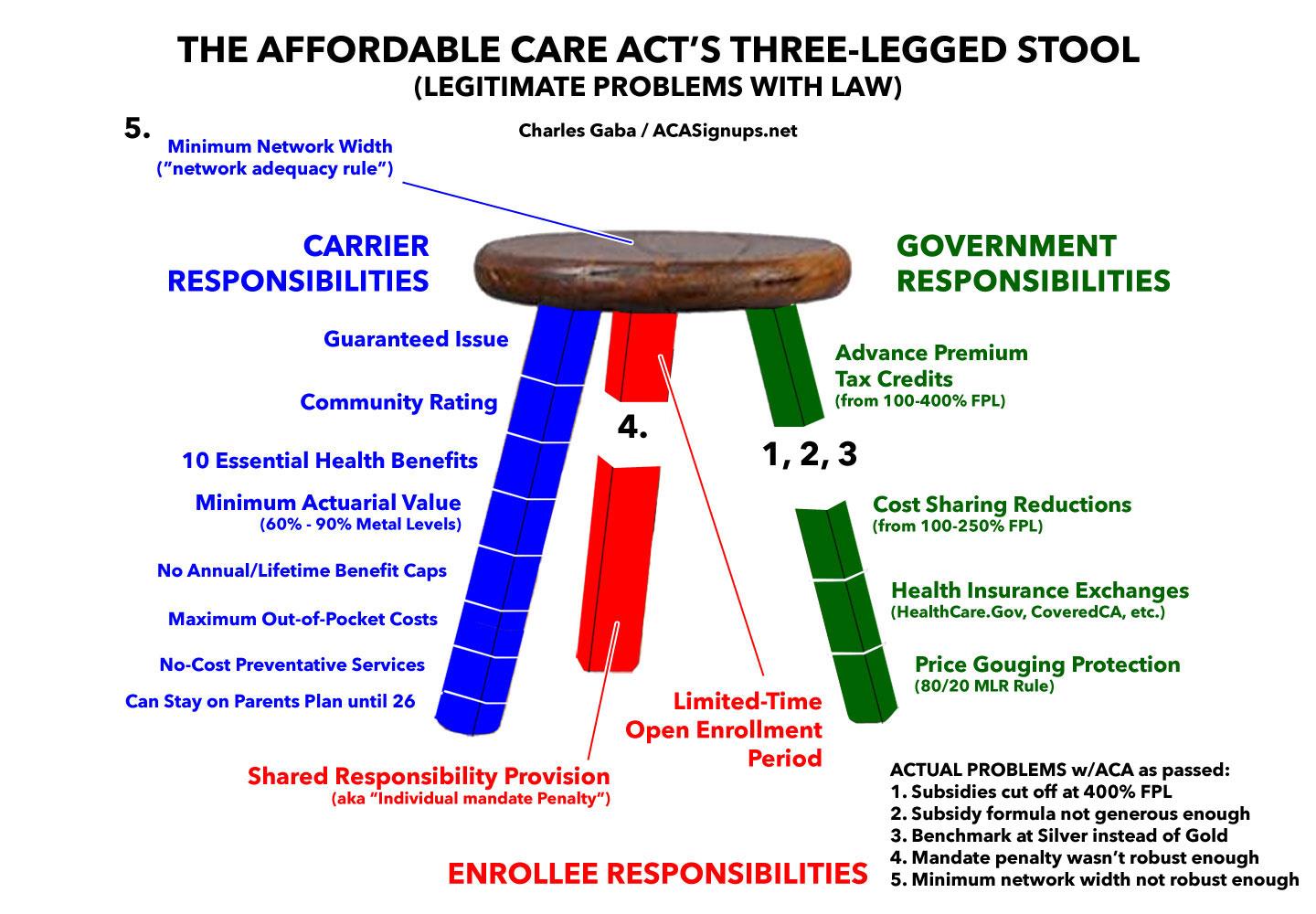
Unfortunately, the "3-legged stool" structure had some flaws even before the Trump Administration and Congressional Republicans started monkeying around with it...flaws which have been made worse in the past few years. Here's some of the major ones:
Essentially, the ACA financial subsidies aren't generous enough and don't apply to enough people; the individual mandate penalty was never robust enough to be fully effective; and the requirements for provider network width are too narrow, leading to problems like the Surprise Billing debacle which has received so much attention nationally of late.
Here's what the 3-legged stool looks like today, after various Trump-era policy changes:
The most obvious changes are:
- The federal Individual Mandate Penalty has been zeroed out (from $695/person or 2.5% of household income down to $0/person or 0.0% of income); and...
- Cost Sharing Reduction (CSR) subsidy reimbursement payments have been cut off by the Trump Administration in an attempt to sabotage the exchanges.*
*(That's not just my opinion...Donald Trump openly and repeatedly stated that he was cutting these off in a deliberate attempt to "blow up" the exchanges and "destroy Obamacare").
Zeroing out the mandate penalty led to average annual premiums for ACA policies shooting up around 8% or roughly $48/month on average nationally. It also means that federal taxpayers had to start shelling out an additional $5 billion/year or so in subsidies to absorb the increased cost for subsidized enrollees...while unsubsidized enrollees have to pay the additional $580/year.
The insurance carriers responded to the CSR reimbursement payment cut-off, meanwhile, coming up with a clever pricing workaround strategy called "Silver Loading" which has actually resulted in reduced premiums for many subsidized enrollees...but also to higher premiums yet for some unsubsidized enrollees.
So what happens if the Texas vs. Azar lawsuit is ultimately successful? Well, it's possible that the only thing which will happen is the underlying individual mandate penalty is struck from the law, in which case the rest of the ACA would continue to chug along as is. It's also conceivable that only the blue leg would be ripped away (i.e., the protections for coverage of pre-existing conditions), leaving the rest of the stool intact.
However, it's also very possible that the entire ACA will be struck down en masse...which would be a catastrophe:
Here's the thing, though: Even if the ACA does survive this lawsuit, there's no guarantee that it will be improved in any substantial way at the federal level anytime soon.
That leaves things up to the states.
Here's the good news: There's plenty of less dramatic, less complex but still important legislation to protect, repair and strengthen the ACA which can be done right here in Michigan.
Some of the protections needed were already included in the Michigan Health Care Bill of Rights resolution introduced by MI House Dems a few years ago, or were referenced by Gov. Whitmer in her State of the State address a few days ago. I agree with all of this, but there's much more needed...and those measures still don't really improve things, they just prevent them from sliding backwards.
The purpose of this letter is to provide a list of the various ACA protection, repair and strengthening bills I strongly recommend you pass & sign into law this year.
Other states have already introduced, passed, and/or implemented several of the items on this list, including Alaska, California, Colorado, D.C., Hawaii, Maine, Maryland, Massachusetts, Minnesota, New Jersey, New Mexico, New York, Oregon, Rhode Island, Vermont and Washington State and others.
PROTECTIONS: Legislation which would lock in existing ACA protections in the event they're stripped away at the federal level:
- 1. Guaranteed Issue: Health insurance companies cannot deny coverage to anyone for having a pre-existing condition, nor can they subject enrollees to medical underwriting. According to this analysis by the Commonwealth Fund, Michigan already codified partial guaranteed issue protection pre-ACA, but if my memory serves that was structured completely differently from the current situation...I believe Blue Cross Blue Shield of Michigan was legally required to be the "insurer of last resort"...they had to accept anyone who enrolled, although they were allowed to impose a six-month waiting period first before coverage began.
- 2. Community Rating: Health insurance companies cannot charge people higher premiums or deductibles for a policy based on their health status/history or other factors. Again, the Commonwealth Fund says that some sort of limited community rating provision is included under state law in Michigan already, but I don't know the details; my guess is that it's completely inadequate to what the landscape would look like if the ACA were to be struck down.
- 3. Gender Equality: Health insurance companies cannot charge more for a policy based on gender.
- 4. Limiting the Age Tax: Prior to the ACA (and under GOP repeal bills), seniors were often charged 5 times as much as younger enrollees; the ACA restricts the premium age band to a 3:1 ratio.
- 5. Essential Health Benefits: All health insurance policies must include coverage of at least the same 10 Essential Health Benefits mandated by the Affordable Care Act.
- 6. No Annual or Lifetime Coverage Limits: ACA-compliant health insurance policies cannot include caps on annual or lifetime benefit limits on covered medical claims.
- 7. Minimum Actuarial Value: Health insurance policies must cover at least 60% of enrollees' healthcare expenses on an actuarially-determined level.
- 8. Free Preventative Services: The ACA mandates a list of services such as annual physicals, mammograms, drug screenings etc. which enrollees cannot be charged any out-of-pocket fees for (as long as the provider is in-network).
- 9. Medical Loss Ratio: Health insurance companies are required to spend at least 80% of premium revenue on actual healthcare services for individual (nongroup) or small group market policies; anything under that has to be rebated to the policyholder. In the case of the large group market, the threshold is 85%.
In fact, there are two states which have set higher MLR ratios on the individual and small group markets than the ACA: New York sets them at 82% while Massachusetts sets it at 88%...yet Massachusetts still somehow manages to have the lowest unsubsidized individual market premiums in the country year after year, which means that their insurance carriers are still making a profit. Food for thought.
- 10. Cap on Maximum Out of Pocket Costs: The ACA mandates that health insurance policies include a cap on the maximum amount that enrollees have to pay for medical services out of pocket (for in-network care) regardless of how much the deductibles, co-pays and coinsurance are.
- 11. Young Adults on Parents Plans: Under the ACA, young adults are allowed to remain enrolled on their parents or guardians' insurance policies until they turn 26 years old.
- 12. Rate Review Protection: Under the ACA, insurance carriers which ask for rate increases of more than 10% per year have to undergo an additional regulatory process to review and justify those increases.
- 13. Limit Smoker Surcharge to 50% (or lower): As noted above, under the Affordable Care Act, insurance carriers aren't allowed to ask about or vary your premiums for any medical history/status or lifestyle choices...with one exception: Premiums can be up to 50% higher for those who smoke. There's four states which match that or which have tighter ratios (ranging from 15% - 50%), and seven states which don't allow smoker premium variances at all. I actually have mixed feelings about this, since smoking is a major contributor to bad health...but according to this study, the 50% surcharge isn't doing anything to improve anyone's health or cause anyone to quit smoking anyway. With that in mind, Michigan might consider either tightening up on that ratio or eliminating the smoker surcharge altogether.
REPAIRS: Legislation which would restore ACA protections/regulations which have already been stripped away at the federal level either legislatively or via regulatory changes by the Trump Administration:
- 14. Eliminate Work Requirements from ACA Medicaid expansion (Healthy Michigan)
This one is a no-brainer, but it's still important to include here. The work requirement provision is cruel, counterproductive and very likely illegal, given the recent federal judicial ruling in Kentucky and Arkansas (that remains to be seen of course; it's an ongoing saga). The reality is that after a lot of states jumped onto the work requirement train a few years ago, more recently there's been a reversal. Indiana, Arizona, Montana and Virginia have all either abandoned work requirements entirely or put an indefinite delay on implementing them. The bottom line is that they're simply too much of a waste of time, effort and money to be worth the "advantages"...especially when recent studies have shown that Medicaid expansion actually increases employment without work requirements...which is the supposed justification for adding them.
- 15. Regulate Short-Term, Limited Duration Plans more strictly.
The ACA didn't actually ban STLDs, which don't include most of the protections listed above; instead, it laid out what provisions a policy had to include in order to qualify as ACA-compliant coverage to avoid having to pay the Individual Mandate penalty. Therefore, someone could still enroll in an STLD if they wanted, but they'd still have to pay the ACA penalty. In 2016, the Obama Administration put some additional restrictions on STLDs, limiting enrollment in them to no more than 3 months per year (thus keeping them "short-term") and forbidding them from being renewed within the same year (thus keeping them "limited duration"). Because of this (as well as the fact that STLDs fall far short of comprehensive coverage and are often junk plans), only a small number of people have enrolled in STLDs over the past few years, limiting their adverse selection impact on the ACA market risk pool.
More recently, however, the federal mandate penalty was zeroed out (removing one disincentive to enroll in junk policies)...and at the same time, the Trump Administration removed the 3-month and non-renewable regulatory limits on STLDs at the federal level, pushing the throttle wide open for junk plans to flood the market with no disincentive involved...other than the fact that these plans allow pre-existing condition denials, pricing discrimination, don't cover all 10 EHBs, have no minimum AV threshold, have annual/lifetime caps and so on.
Basically, while not every STLD is junk, they're all discriminatory, and these are exactly the types of policies which the ACA set out to get people off of in the first place.
Michigan does currently have partial regulation of STLDs. According to the Commonwealth Fund, in Michigan...
- Total contract period for STLDs, including any renewal periods, cannot exceed 185 days out in a 365-day period
- Michigan keeps STLDs a small part of an insurer’s individual market portfolio by limiting the share of individual market premiums an insurer can collect from them.
However, I urge MI lawmakers to go further. Some states have banned them entirely like New Jersey and California have. I'm not calling for them to be completely banned (yet), since ACA policies are unaffordable for many unsubsidized enrollees; I am, however, urging you to at least codify the Obama regulations restricting STLDs to no more than 3 months per year and preventing them from being renewable, as DC, Hawaii and Maryland are doing/have done. This wouldn't likely have a significant impact on premiums in Michigan given the limited protections already on the books, but even a 1% premium drop would save tens of thousands of Michiganders ~$60/year apiece.
- 16. Regulate Association Health Plans more strictly.
Here's a good explainer of what Associaion Health Plans (AHPs) are and why they're problematic for similar reasons to Short-Term, Limited Duration plans from the Commonwealth Fund:
AHPs have existed for decades. Many are legitimate arrangements made by associations to offer health benefits to members, but some have defrauded enrollees or ended up insolvent, unable to pay members’ claims. They are typically subject to the federal Employee Retirement Income Security Act (ERISA) because they are multiple employer welfare arrangements (MEWAs), but are also subject to state regulation. Illegitimate AHPs have exploited the gaps resulting from AHPs falling in an ambiguous place between state and federal regulation.
The Affordable Care Act (ACA) enhanced regulatory oversight of AHPs, clarifying that AHPs that enrolled individuals or small groups were generally subject to ACA’s individual and small-group market rules. For instance, an AHP that covered individuals or small groups would be required to offer essential health benefits.
There was, however, a very limited exception. An AHP covering small employers could be considered a single large-group health plan under ERISA for regulatory purposes if the employers were bound together by a common interest beyond health coverage and effectively operated as one employer controlling the association. Employers had to share a common trade, business, or profession; shared geographic location (e.g., a chamber of commerce) was not enough. “Plan MEWAs” that qualified would be regulated by the less stringent large-group rules even though they covered only small groups. The exception did not apply to individual sole proprietors. Associations of individuals could never be considered a single employer nor be regulated as a large group. AHPs formed under this exception are now called “pathway 1” AHPs.
In June 2018, the Department of Labor (DOL) greatly expanded the circumstances under which an aggregation of small groups could be considered a large group, creating what are now called “pathway 2” AHPs. Under DOL’s new regulations, an AHP could pass muster as a single employer plan if:
- it served at least one substantial business purpose other than providing health coverage, even though its primary purpose was offering health coverage
- its member employers were either in the same trade or business or in the same geographic area, which could span several states, and
- the employer members in some sense controlled the AHP and health plan.
Under the new regulations, AHPs could also cover individual “working owners,” even though the working owners had no employees other than themselves. The rule prohibited AHPs from discriminating against enrollees on the basis of health status but allowed AHPs to exclude or charge higher premiums to employers on the basis of age, gender, occupation, or other factors.
Although AHPs continue to exist under the pathway 1 rules, a number of entities — in particular, chambers of commerce — have moved quickly to take advantage of the new rule. The Congressional Budget Office projects that more than 3 million people will be covered by an AHP under the new rule. Some states have taken legislative or regulatory actions to encourage or to discourage AHP formation under the new rules.
Maryland, New Jersey and Vermont have each either banned or put strict controls on AHPs. Michigan should join them.
- 17. Restore the Individual Mandate Penalty:
While Michigan didn't get hit as hard as some states, the federal Individual Mandate being zeroed out caused average individual market premiums in Michigan to increase by roughly 5% in 2019. That's an extra $300 per person for unsubsidized individual market enrollees.
Restoring the mandate should, in turn, result in 2021 rates dropping by around the same amount (or at least increasing by less than they would have otherwise).. I know very well that this may be considered Kryptonite politically, but New Jersey, Vermont, DC, California and Rhode Island have all done it, and Massachusetts just reverted back to their Romney-era penalty, which means at least 18% of the U.S. population has a mandate penalty in place as of today. Many healthcare analysts feel that the ACA's penalty ($695/adult + $348/child or 2.5% of household income) was too weak to be properly effective, but I have to imagine that increasing it beyond that amount would be a bridge too far, so I'd recommend simply restoring it to the ACA levels, as most of these states have done.
STRENGTHEN: These are improvements to the ACA which take the ACA as it was supposed to be implemented to the next logical phase. Again, none of these steps go as far as either Single Payer or even a Public Option, but even a handful of them would dramatically improve & expand coverage and lower costs for enrollees.
- 18. REINSURANCE!
When the ACA exchanges first launched for the 2014 Open Enrollment Period, the law included three individual market stabilization programs. One of the programs was called reinsurance, and it worked pretty well. Unfortunately, the federal ACA reinsurance program sunsetted after only three years, at the end of 2016, which is part of why rates spiked so much in 2017 (they shot up in most states in 2018 as well, but for very different reasons).
In response, over a dozen states including Alaska, Minnesota, Oregon, Maryland, New Jersey, Wisconsin, Delaware, North Dakota and Maine have instituted something called an ACA Section 1332 Waiver reinsurance program which replicates the federal version. It's a fairly cut & dried way of keeping unsubsidized premiums down (or even lowering them in some cases) which requires no additional federal spending and much less state spending than you might think.
I've written a (hopefully) straightforward tutorial on how reinsurance works. The beauty of it is that looking at some of the other states which have implemented similar programs, it's likely that the federal government would end up covering anywhere from 35% - 85% of the cost.
How much would this cost in Michigan in real dollars?
Well, in 2019 Michigan's individual market was around 317,000 people. In 2020, unsubsidized enrollees are paying an average of around $485/month last year. That's a total of around $1.84 billion in total premium revenue. Let's assume that a little over 80% of those premiums are actual medical claims (to meet the 80/20 MLR rule). That means Michigan ACA individual market enrollees rack up around $1.48 billion in insurance claims each year, or around $4,700 apiece.
Let's suppose we established a reinsurance program identical to New Jersey's, and the enrollee cost breakout in Michigan was something similar to the following:
In this scenario, $134 million of the total expenses would be covered by the reinsurance program, or around 9% of total claims, which translates to around a 7.3% reduction in unsubsidized premiums.
However, thanks to the way the ACA federal waiver program works, as I explained here, a good chunk of that $134 million...perhaps 75% of it...would actually be covered by the federal government as a portion of the reduced ACA subsidies are redirected towards the reinsurance fund.
Put another way, it might only cost the state of Michigan $34 million to cut healthcare premiums by 7.3% for over 120,000 people. And where would that $34 million come from? Well, in New Jersey, they expect to raise $90 million or so per year from...reinstating the individual mandate, which they're in using to help fund their reinsurance program.
Obviously the actual cost and impact on premium reductions could very widely depending on what the actual claim breakout is across the enrollees, how the program is structured and how much medical claims for high-risk enrollees are. In New Jersey, which actually has fairly close individual market demographics to Michigan, unsubsidized premiums are over 15% lower than they otherwise would've been due specifically to their reinsurance program (and another 8% lower thanks to them reinstating the mandate penalty).
If you want some real-world examples of how effective reinsurance programs can be, in Alaska, premiums dropped by a whopping 23.6% in 2018. In Colorado, they dropped by over 20% on average this year.
There's actually a more effective way of providing premium relief to enrollees than reinsurance...but it requires more prep work to establish, and in particular it first requires the state to...
- 19. Lower state ACA premiums by $10 million/year by Establishing a State-Based ACA Exchange!
Right now, 3.0% of the premiums paid by Michigan ACA exchange enrollees goes to pay for the marketplace fee which funds HealthCare.Gov. That 3.5% remained the same for five years straight, even as baseline premiums more than doubled. While it was reduced from the prior 3.5%, it still means Michigan residents are paying more than twice as much to fund the federal exchange today as they were six years ago for the same services. In fact, as noted below, CMS has slashed the budget for marketing and outreach by around 90%.
If Michigan broke off from HC.gov and established our own full ACA exchange, as Nevada did this year, and as New Mexico, Pennsylvania and New Jersey are all doing next year, we could cut that cost down to as low as, say, 2.2% of premiums or lower. If so, that would save over 210,000 Michiganders around $48/year apiece, or $10 million per year total or more.
As for actually establishing the exchange in the first place, the world has changed dramatically since the ugly launch of HC.gov and some of the state exchanges back in 2013. Back then, many states spent hundreds of millions of dollars on technical disasters. Since then, however, exchange technology has become nearly an out-of-the-box commodity. Nevada's ACA exchange is only costing about $24.5 million over five years (plus a $1 million Design Development & Implementation expense). Heck, that could potentially even be paid for just by delaying the fee reduction for the first two years or so.
Assuming 2.2% per enrollee, 210,000 effectuated exchange enrollees per month would generate at least $27 million per year, which would be more than ample to operate the entire exchange. For comparison, Nevada and Idaho's annual budgets currently run around $10 million each for their exchanges; Michigan is a larger state, but the additional costs wouldn't scale up proportionately, so it's conceivable that the fee could be kept as low as 1.5% or so, saving enrollees up to $20 million/year!
Once this is established, it would allow Michigan to...
- 20. Provide additional subsidies to those under 400% FPL, and/or...
- 21. Provide additional susbsidies to those OVER 400% FPL
The reinsurance programs described above technically lower premiums for everyone on the individual market, but in practice it's only unsubsidized enrollees who see their premiums drop significantly, since most subsidized enrollees would see their subsidies drop to match the premium drop. Unfortunately, one downside to reinsurance programs is that depending on the state, reducing unsubsidized premiums can also have the seemingly counterintuitive effect of raising subsidized premiums! This is because in some cases the amount of the subsidies drops more than the amount of the full premium, leaving a higher net premium for subsidized enrollees. Huh.
However, there's another variant of this which does't require any federal funding at all and therefore doesn't require a federal waiver either: The state could simply cut out the middle man and provide supplemental premium subsidies to those earning too much for APTC assistance directly.
Two other states provide their own, additional subsidies to ACA enrollees today (Massachusetts and Vermont). In each of those cases, they provide enhanced assistance to enrollees earning less than 300% FPL. While that's not a terrible thing, the 100-300% FPL crowd isn't where the biggest problems are; it's those earning too much for subsidies (basically enrollees earning over 400% FPL).
As it happens, California just became the first state in the country to expand ACA subsidies to those earning more than 400% FPL. In their case they're using the revenue from their reinstated mandate penalty (combined with some additional funding) to provide subsidies to enrollees earning 400 - 600% FPL, plus enhanced subsidies to those earning 200 - 400% FPL.
An average of 317,000 Michiganders were on the individual market last year. Of those, around 110,000 were unsubsidized. When you include middle-class folks who've been forced to drop their coverage due to unsubsidized premiums rising too much, state-based subsidies could likely go to perhaps 150,000 Michiganders over the 400% threshold. Average Silver ACA policy premiums are around $5,800 this year.
Reestablishing the mandate penalty would likely generate around $100 million or so (I'm basing this on New Jersey figures; NJ has a slightly smaller population than Michigan and a similar individual market size). That would be enough to provide supplemental subsidies of up to $650/apiece for 150,000 enrollees or $2,000/apiece for 50,000 enrollees.
Establishing our own ACA exchange would also allow Michigan to...
- 22. Extend the Open Enrollment Period.
This one really belongs under the "repair" category, but I'm listing it here since it would depend on moving to a state-based exchange: For several years, the official Open Enrollment Period ran for a solid 3 months: November, December and January. The Trump Administration decided to slash that in half to just 6 weeks (11/01 - 12/15). While this had the upside of ensuring that a higher percentage of enrollees hit the ground running with effectuated coverage starting January 1st, it also caused problems for people with special circumstances who rely on having extra time to sign up.
State-based exchanges have the ability to establish their own Enrollment Periods. California, New York and DC are keeping 1/31 as their deadline, while several other states bumped theirs out anywhere between one to five weeks. If Michigan had its own exchange, we'd have the flexibility to set enrollment dates that work best for us.
Establishing our own ACA exchange would also allow Michigan to...
- 23. Actively Negotiate Standardized Exchange Plans
Under the ACA, every individual market policy has to meet certain standards: They have to be grouped into one of four categories (Bronze, Silver, Gold and Platinum) which have to cover roughly 60%, 70%, 80% or 90% of the enrollee's medical expenses for in-network care. They have to cover all 10 Essential Health Benefits, and so on and so forth.
However, within those parameters, they're allowed to very pretty widely in terms of exact Actuarial Value, exact networks, what co-pays they charge, what deductibles they charge, what their drug formularies are and so forth. This causes a lot of confusion for people trying to choose a policy and also allows for the carriers to try and game the system via a gimmick known as "Silver Spamming", in which they deliberately flood the market with dozens of nearly-identical policies which only vary slightly in an attempt to "own" the benchmark Silver policy position...which happens to also generally be the most popular plan chosen by enrollees.
As Louise Norris explains, several states have put the kibosh on this practice by instituting "Standard Plans":
Several states either require or encourage insurers to offer standardized plans in their exchanges. HealthCare.gov no longer offers an option to differentially display any sort of standardized plan, but if a state runs its own exchange (ie, it doesn't use HealthCare.gov), the exchange can highlight standardized plans when consumers are shopping for coverage.
The plan designs vary from state to state, but the overall focus is on keeping deductibles, copays, coinsurance, and total out-of-pocket costs identical across all standardized plans at a given coverage level. So for example, all standardized silver plans in Oregon's exchange have $2,850 individual deductibles in 2019 and $35 primary care office visit copays.
Many of the standardized plan designs cover outpatient care with copays, rather than applying it towards the deductible. Most states with standardized plan designs also allow carriers to offer non-standardized plans as well:
- In California, the exchange only allows carriers to offer standardized plans.Covered California—the state-run exchange—does not allow non-standardized plans to be sold, and was very much in support of the introduction of standardized plans in states that use Healthcare.gov instead of running their own exchanges.
- New York requires health insurers to offer at least one standardized plan at each metal level, although insurers are also allowed to offer up to three non-standardized plans. More than two-thirds of the people who enrolled through New York State of Health in 2019 selected standardized plans.
- Massachusetts introduced standardized individual health insurance plans in 2010, and they continue to be available through the state-run exchange, Massachusetts Health Connector. But carriers selling plans in the Massachusetts exchange also have the option of offering non-standardized plans.
You get the idea.
Establishing our own ACA exchange would also allow Michigan to...
- 24. Take full control over our ACA marketing budget.
Again, this really belongs under "repairs:" Last year the Trump Administration slashed the marketing/advertising budget for HealthCare.Gov by 90%. While there are a lot of factors which impact enrollment each year, total enrollment across the 39 states which rely on HC.gov dropped by 5% this year...while enrollment in the 12 states which operate their own ACA exchanges (along with their own brands and marketing budgets) remained flat. If Michigan had its own ACA exchange, it would also include its own branding and marketing program/budget, not subject to the whims of the Trump Administration.
Establishing our own ACA exchange would also allow Michigan to...
- 25. Take full control over our navigator/outreach budget.
Yet another "repair": Last year the Trump Administration ALSO slashed the budget for HealthCare.Gov's "navigator" program (which funds 3rd-party nonprofit organizations which assist people with enrolling in ACA exchange plans and Medicaid programs, as well as generally educating them about how both private insurance and Medicaid work, among other services) by 40%. This year they're slashing it another 72% and will be "encouraging" the remaining navigators to push enrollees towards...short-term and other non-ACA compliant policies. Again, if Michigan had its own ACA exchange, we wouldn't have to rely on federal funding for our navigator program.
- 26. Sunset any remaining Transitional policies.
Under the ACA, all individual market policies were supposed to be fully ACA-compliant (guaranteed issue, community rated, etc.) starting on January 1, 2014. Originally, the only exceptions to this were "Grandfathered" policies which people were already continuously enrolled in since 2010. However, in response to the backlash over his "If you like it, you can keep it!" promise, President Obama had the HHS Dept. issue a policy change which allowed another batch of non-ACA-compliant policies (those enrolled in from 2010 - 2013) to be renewed for another year (these were called "Transitional" or "Grandmothered" policies).
The decision about whether to allow Transitional plans was left up to the individual states. Some states allowed them, some didn't. Even in the states which allowed them, it was still up to the individual insurance carriers whether to cut them off or not; some did, some didn't. Michigan, unfortunately, was among the states which did allow transitional plans. One way or another, that "one year" extension became two years...then three...and now it's at the point where "transitional" plans might as well be considered "grandfathered".
Just like with Short-Term plans, every Transitional Plan enrollee siphons away a healthy person from the ACA-compliant risk pool. Transitional plans probably shouldn't have been allowed in the first place (this is one mistake which belongs to President Obama, not Donald Trump), and even then they definitely shouldn't still be allowed nearly 5 years later. It's time to cut them off and transition the remaining enrollees over to fully ACA-compliant policies, which would also improve the ACA risk pool.
Unfortunately, I don't know exactly how many Michiganders are still enrolled in Transitional policies today, but I guesstimated it at perhaps 82,000 earlier this year. If that's accurate and even half of them shifted to ACA policies, that would enlarge the ACA market by over 10% with mostly healthy enrollees.
- 27. Merge the Individual and Small Group markets!
Most states have three major private insurance markets, which in turn have their own separate risk pool for purposes of setting rates: Large Group (companies employing 100 people or more); Small Group (companies employing fewer than 100 people) and Nongroup (aka Individual), which is for people who are either self-employed (like myself) or who work for companies which don't provide healthcare coverage.
In Michigan, around 51% of the population is covered through their employer. The small group market in Michigan is around 410,000 people, or 4.1% of the population, which means roughly 47% (4.7 million) are part of the large group market. I'm not sure how many of the 4.7 million work for companies with self-insure, but the point is that the large group market is huge. The individual market, of course, is the smallest and most volatile; that's what most of these bullet points focus on stabilizing and improving. In Michigan, the individual market currently consists of around 300,000 people, or 3% of the population.
The larger and more widespread demographically the risk pool, the more stable it tends to be...which is why the large group market tends not to be in the news a lot over dramatic rate increases.
Since both the small group and individual markets are so small, a couple of states (Massachusetts and Vermont) have merged these two into a single risk pool. If that was done in Michigan, it would total roughly 710,000 people, or 7.1% of the population. This would still be much smaller than the large group market, but it would be far more stable than either of them were before.
The downside is that this would mean higher rates for small businesses; the upside is that it would mean lower rates for the individual market...and it would mean both categories would be more stable and consistent going forward.
- 28: Merge the 16 Rating Areas into a single statewide one
The Centers for Medicare & Medicaid (CMS) lists every state as being divided into geographic rating areas, In some smaller/lower-population states, there's a single statewide rating area, but in others there are dozens, and premiums can vary widely from one to another. In Michigan's case there are 16 of areas: Area 1 includes Wayne and Monroe County, Area 2 includes Oakland and Macomb County and so forth. Area 16 includes 13 different counties.
The result of this is that people who move from one part of the state to another can see their health insurance premiums change dramatically...even if nothing else they've done has changed. This bears an eerie resemblance to the "redlining" controversy which was supposed to be fixed in last year's auto insurance reform bill...but wasn't.
To give you an idea of how much of a difference this can make, the benchmark health insurance policy premium in Wayne County (population nearly 1.8 million) costing $333/month for a 40-year old adult may cost $437/month in the more rural Isabella County (population 71,000). Interestingly, this tends to be the exact opposite of auto insurance redlining, where the sparsely populated rural areas tend to be priced cheaper than the densely populated urban areas...but it's something which should be looked into either way.
- 29. Tie ACA market participation to MCO or State Employee contracts
This one probably isn't necessary in Michigan at the moment since we seem to have pretty robust participation in the ACA market throughout the state, with several carriers available in each rating area. Still, it wouldn't be a bad idea to put into place anyway to prevent a "bare county" situation down the road. Basically, you pass a law mandating that in order to win either a managed Medicaid contract or, alternately, a state employee/public school group coverage contract, the insurance carrier has to also agree to offer a minimum number of individual market policies on the ACA exchange as well.
This policy is already in place in New York State (via executive order by Gov. Cuomo), while there's a bill to do so pending in California. Washington State, menawhile, recently passed HB2408, which would tie public school employee coverage contracts to ACA exchange participation.
- 30. Establish a Maryland-style All-Payer Rate Requirement.
Here's a simple explanation of what All-Payer means from Sarah Kliff of Vox a couple of years back:
All-payer rate setting, as the system is known, shares the same goals of single-payer: it aims to increase efficiency and reduce insurer overhead in the health care system. Single payer does this by eliminating private plans for one government plan. All-payer rate setting gets there by setting one price that every health insurer pays for any given medical procedure.
"[All payer] has everything except the government-run plan," says Mark Pauly, a health economist at University of Pennsylvania. "In all-payer systems, the government uses Blue Cross and other insurers as their agent. For consumers its the exact same except for who they write their check for premiums to."
...Right now, there is huge variation in health care costs at different hospitals and doctor offices. The reason is different health-insurance plans pay different prices for medical care. That means the price of an MRI scan or knee replacement surgery, for example, can vary widely, depending on how good an insurance plan is at negotiating.
Bigger plans tend to negotiate deeper discounts. Most research shows that private insurance plans pay the most, Medicare pays slightly less, and Medicaid pays the lowest rates. And even between different private insurance plans, there can be huge variation — a bigger plan with more members might be able to ask hospitals for lower prices because it can promise lots of patients.
Read the whole thing for more details. The point here is that Maryland recently experimented with All-Payer on a limited basis, and it worked well enough that they recently expanded upon the program:
Maryland Gov. Larry Hogan signed a contract with the federal government on Monday to enact the state’s unique all-payer health care model, which he said will create incentives to improve care while saving money.
Hogan signed the five-year contract along with the administrator of the federal Centers for Medicare and Medicaid Services, Seema Verma.
...The Hogan administration said the new contract is expected to provide an additional $300 million in savings a year by 2023, totaling $1 billion in savings over five years.
Maryland is the only state that can set its own rates for hospital services, and all payers must charge the same rate for services at a given hospital. The policy has been in place since the 1970s, though Maryland modernized its one-of-a-kind Medicare waiver about four years ago to move away from reimbursing hospitals on a fee-for-service basis to a fixed budget.
Because that change focused on hospitals only, the federal government required the state to develop a new model that would provide comprehensive coordination across the entire health care system.
Under the agreement, Maryland will be relieved of federal restrictions and red tape that the other 49 states face in the Medicare program. However, the state will have to meet benchmarks of improving access to health care while improving quality and reducing costs.
I know of quite a few progressive healthcare wonks who are more excited about All-Payer than they are about Single Payer, although obviously your mileage may vary.
- 31. Restrict sales of ACA-compliant policies to the ACA exchange.
This is something I've been pushing states to do since the very first Open Enrollment Period launched in 2013. For all the talk about how many people are enrolled "in Obamacare" each year, the truth is that there's a second batch of ACA individual market enrollees called the off-exchange market. These are, for the most part, the exact same insurance policies, as those sold via HealthCare.Gov and other ACA exchanges, but people enroll in them directly through the insurance carriers or via insurance brokers, just as they did before the ACA.
The main reason people do this is because it saves filling out some additional paperwork. If you know that your income is going to be too high to be eligible for financial subsidies, there's not much point in enrolling on exchange, so the off-exchange market is mostly composed of middle- and higher-income people.
Unfortunately, this also causes confusion and unawareness of the benefits of enrolling on-exchange, such as the following:
Plus, the call that triggered this tweet was a single mom, 2 kids who has been off exchange and subsidy eligible since 2014. Last year, she was eligible for $15K.
— Jenny*KG Health Insurance* Hogue (@kgmom219) February 5, 2020
That's a Texas-based insurance broker talking about a single mother of two children who has apparently been missing out on up to $15,000/year for the past 6 years straight...all because she enrolled in an ACA-compliant insurance policy off-exchange instead of on-exchange.
As of today, the District of Columbia is the only place where all ACA policies have to be enrolled in via their exchange. Vermont did that for a few years as well, though they've backed off of it more recently. I'd prefer to have all ACA policies run through the on-exchange market. In addition to avoiding the problems like the woman described above, this would also make tracking enrollment trends/etc. a lot easier, which helps make it easier to set future policy changes as well.
- 32. Expand Medicaid coverage to at least some undocumented immigrants.
I realize this is a long shot, but Michigan had around 130,000 undocumented immigrants as of 2014...that's 1.3% of the entire state's population. Nationally, around 45% of undocumented immigrants are uninsured. I have no idea if that's representative in Michigan specifically, but if it is, that amounts to roughly 59,000 in our state.
California, which has a much larger undocumented immigrant population, of course...over 5.5% of the state's population (around 2.2 million people) recently enacted a law which expands Medicaid to around 100,000 income eligible young adults age 19 - 25. In Michigan that would likely amount to just 2,700 young undocumented immigrants.
- 33. Establish a Basic Health Plan program under the ACA
I'll let Louise Norris of healthinsurance.org explain:
Under the ACA, most states have expanded Medicaid to people with income up to 138 percent of the poverty level. But people with incomes very close to the Medicaid eligibility cutoff frequently experience changes in income that result in switching from Medicaid to ACA’s qualified health plans (QHPs) and back. This “churning” creates fluctuating healthcare costs and premiums, and increased administrative work for the insureds, the QHP carriers and Medicaid programs.
The out-of-pocket differences between Medicaid and QHPs are significant, even for people with incomes just above the Medicaid eligibility threshold who qualify for cost-sharing subsidies.
The Basic Health Program (BHP) – section 1331 of the ACA — was envisioned as a solution, although most states did not establish a BHP. Under the ACA (aka Obamacare), states have the option to create a Basic Health Program for people with incomes a little above the upper limit for Medicaid eligibility, and for legal immigrants who aren’t eligible for Medicaid because of the five-year waiting period.
The Basic Health Program was originally scheduled to begin January 1, 2014, but was postponed until 2015. And even then, only two states chose to implement a BHP: Minnesota‘s BHP was effective in January 2015 (see Minnesota’s BHP blueprint), and New York‘s took effect in January 2016 (see New York’s BHP blueprint).
There's over 820,000 people enrolled in BHP plans across New York and Minnesota. It covers people earning between 138 - 200% FPL, and is sort of a hybrid between Medicaid and a heavily-subsidized ACA exchange plan...but it's vastly simplified in design and is a perfect solution for a lot of people. Since it's part of a separate risk pool from ACA plans, and since lower-income people tend to be sicker than higher-income folks, this can also improve the ACA risk pool a bit. Michigan might consider looking into this.
- 34. Petition the Federal Government to be able to Import Drugs from Canada
This is one which the state unfortunately has no control over since it's a federal issue, but we can certainly give it a shot (this is from 2018):
As states pursue a wide range of legislation to address rising drug costs, four more states have joined Utah and Vermont to introduce bills to import prescription drugs from Canada through a state-run, wholesale operation. This market-based approach to providing more affordable medicines from Canada, where prescription drugs cost on average 30 percent less than in the United States, is appealing to a politically diverse group of states, and is currently under review by legislators in:
- Colorado (S 80); Missouri bill studies the creation of an importation program (SB 722); Oklahoma (SB 1381); Utah (HB 163); Vermont (S 175); and West Virginia (HB 4294).
A fiscal analysis recently completed in Utah indicated the potential for millions in reduced spending due to the significant price differences between certain products sold in the United States and Canada. This month, NASHP is convening state legislative sponsors to share information and expertise about the importation policies in their states. Many of the importation bills currently under review are based on National Academy for State Health Policy’s (NASHP) model legislation.
With Michigan right on the border of Canada and Windsor right across the Detroit River, this should be a no-brainer.
- 35. Crack down on Surprise Billing
This major problem has been in the news a lot lately. The most common example is when someone has a surgical procedure at a hospital they know is in-network, performed by a surgeon they know is in-network...but it turns out that the anesthesiologist isn't in-network. A few weeks later the patient receives a bill for $10,000 (or whatever) from a doctor they've never heard of who they had no way of knowing was out of network. That's an absurd situation; no one can be expected to know whether every single person who provides medical care or services is within their insurance policy's network or not (especially if they're unconscious at the time).
There's been a big, rare bipartisan push to deal with it at the federal level, it somehow still hasn't happened yet. Generally the solution involves dumping these types of charges on either the provider or the insurance company, or forcing some sort of arbitration or standardized rate for such charges. The main point is to take the patient out of the loop. A bunch of states have passed laws or regulations to crack down on the Surprise Billing problem, however, including California, Connecticut, New Jersey, New Mexico and Washington State among others; Michigan should join them.
- 36. Establish a state-level Public Option!
For all the fuss & bother being made about this at the federal level in the Democratic Presidential candidate debates, several states have already taken action locally, including Washington State and Colorado. In both cases, the plans aren't quite what most people are envisioning as a full public option; instead of having state employees actually administer the plans, both states are essentially outsourcing the adminstration of the plan itself to a private insurance carrier, but the state designs the plan designs, establishes the networks and sets the provider reimbursement rates.
It's this last point which is the most important one: In Washington State, providers will be paid 160% of Medicare rates (up from the originally proposed 100%, which was never likely to happen), while in Colorado, they'll be paid between 175 - 225% of Medicare rates, which is also an important testament to either how little Medicare pays or how much private insurance pays relative to it in Colorado.
There are plenty of other bills which could improve things as well, of course (I haven't even touched on prescription drugs), but this list should give plenty to chew on.
In closing, I need to once again stress that all of the above improvements should be pushed simultaneously with whatever the next phase in healthcare reform ends up being at the federal level. One doesn't preclude the other.
How to support my healthcare wonkery:
1. Donate via ActBlue or PayPal
2. Subscribe via Substack.
3. Subscribe via Patreon.