Trumpcare Coverage Loss & Pre-Existing Estimates: Special Election Edition!
Over the past few months, my Congressional District Breakdown tables estimating how many people would likely lose healthcare coverage if the ACA were to be "cleanly" repealed (with no replacement) have gotten a lot of attention. This was followed by the Center for American Progress (CAP) running their own estimates of how many would likely lose coverage if, instead of a "clean" repeal of the ACA as a whole, the ACA were to be partially left in place, with the GOP's AHCA (Trumpcare) bill, which dramatically changes the ACA, being signed into law instead.
Later, CAP did a follow-up analysis to determine just how many non-elderly people in each district have pre-existing conditions which would likely make them either uninsurable or potentially charged exorbitant rates for coverage if the ACA's pre-existing condtion protections were to be stripped away. I grouped their CD-level estimates together by state and color-coded them for easier viewing, and also added my own estimates of how many of those with pre-existing condition are currently on individual market policies, since that's the primary population which would be impacted.
Now that the House has actually voted to pass the AHCA bill, the next order of business are the three special Congressional elections coming up in Georgia, Montana and South Carolina, so I decided to make it easy for activists to focus on the three districts in question: GA-06 (the ultra-high profile race between Democrat Jon Ossoff and Republican Karen Handel); MT-AL (Democrat Rob Quist vs. Republican Greg Gianforte) and SC-05 (Democrat Archie Parnell vs...whoever wins the GOP nomination runoff in mid-May).
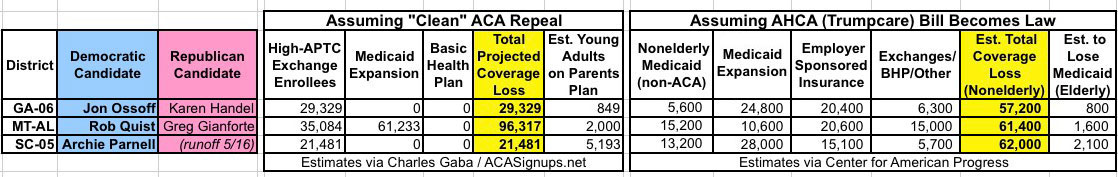
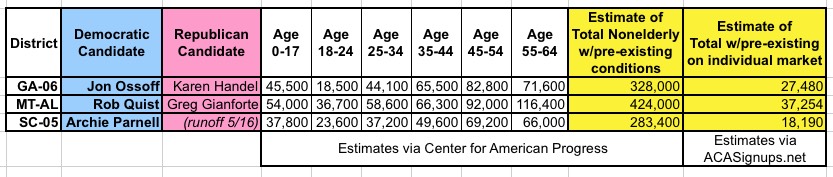
One thing to note re. the "Medicaid Expansion" column in the first graphic: Neither Georgia nor South Carolina have expanded Medicaid yet, making it a bit confusing as to why there'd be any numbers listed there at all. Here's CAP's explaination:
Estimating reductions in Medicaid by district required more assumptions. The CBO projects that a total 14 million fewer people would have Medicaid coverage by 2026 under the House bill: 5 million fewer would be covered by additional Medicaid expansion in new states, and 9 million fewer would have Medicaid coverage in current expansion states and among pre-ACA eligibility groups in all states. The CBO projects that, under the ACA, additional Medicaid expansion would increase the proportion of the newly eligible population residing in expansion states from 50 percent to 80 percent by 2026. It projects that, under the House bill, just 30 percent of the newly eligible population would be in expansion states. Extrapolating from the CBO’s numbers, we estimate the bill results in a Medicaid coverage reduction of 3.3 million enrollees in current expansion states by 2026.
Basically, the CBO assumes that if the ACA is left alone, eventually at least some of the 19 remaining non-expansion states will finally come around and expand Medicaid after all. The CBO's logic, therefore, is that if the AHCA is passed, those same states would certainly not be expanding Medicaid in the first place, therefore they still count those enrollees as having lost coverage by 2026. This may not seem to make sense at first, but you have to understand that the CBO has to make a 10-year projection based on certain assumptions under both the "baseline" scenario (ie, what they expect to happen if the AHCA isn't passed and the ACA is left alone for a decade) and under the AHCA-becoming-law scenario. The CBO is called upon to do this all the time; it's not an easy task, usually they do a pretty good job, sometimes they miss the mark.
My own "Clean Repeal" numbers are easier, since they're based on only next year alone: If the ACA were to be repealed outright this year, no additional states would be expanding Medicaid anyway, so no one would be losing coverage who didn't already have it.
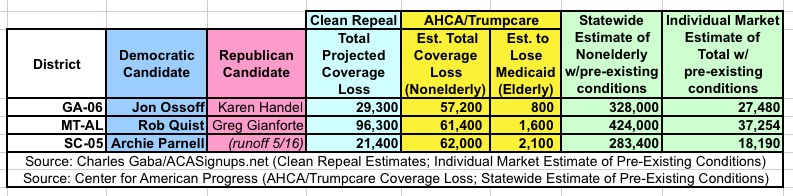
UPDATE: I've merged both (all three, really) tables above into a single, handy table suitable for sharing on social media:
How to support my healthcare wonkery:
1. Donate via ActBlue or PayPal
2. Subscribe via Substack.
3. Subscribe via Patreon.



