Not Just UHC: Has the Great Insurance Broker Purge begun??
"Get him out of my sight, Lou! I want him in town, though. He's still under contract. I want you in town, Fink...and out of my sight." --Barton Fink
The big ACA story Thursday morning was about UnitedHealthcare announcing that while they're still available across half the country for 2016, they may drop out of the ACA exchanges next year (2017). Furthermore, they're cutting their marketing/promotional efforts for the exchanges and, in an additional exclusive tidbit from myself, they've also informed their commission-based brokerage network that they'll be slashing their commission rates by as high as 80% for exchange-based enrollments. On top of that, they've even supposedly deliberately disabled various database tools used specifically by brokers to assist in helping people sign up for UHC policies through the exchanges.
The oddest thing about today's announcement...and the one which made it come as such a shock to interested parties...is that just a month ago, in UHC's quarterly financial report, they stated the following (verbatim):
The annual care ratio is being modestly affected by the performance of our new public exchange benefit programs, which now serve nearly 550,000 people. Like others, we observed market-wide data this past spring that suggested the risk pool served by public exchanges would require more medical services than original expectations. Rather than wait for our own experience with our new members to fully develop, we increased rates and repositioned certain products market by market for 2016, and we expect improved performance next year. We will expand to 11 new markets in 2016 and we continue to expect exchanges to develop and mature over time into a strong, viable growth market for us.
That was an official quarterly financial report. I presume they have these things reviewed up the yin-yang by auditors, actuaries and analysts before releasing them...yet somehow between 10/15/15 and 11/19/15 (strike that...the letter to brokers was sent out on 11/17, presumably the decision was made at least a day or to before that) they did a complete 180 and now are suddenly running around with their hair on fire?
Even more interestingly, they're only making these moves for exchange policies, not for OFF-exchange policies...even though those are, for the most part, part of the same risk pool and in some cases are the exact same policies. Even curiouser, they decided to make this announcement right now, in the very thick of the open enrollment period itself, instead of waiting until the dust settled on 2016 Open Enrollment. Making a big, splashy announcement like this today all but guarantees that they've likely scared off a chunk of potential enrollees who are now wary of signing up with UHC for 2016 when there's a good chance they'll have to switch again for 2017.
In short, UHC is choosing to remain on the exchanges but at the same time are doing everything in their power to prevent people from actually buying their products through the exchanges...and are taking extra measures to lower the number of enrollees who sign up specifically with the help of commissioned brokers.
However, believe it or not, I'm not here to write about UnitedHealthcare tonight; that was all just the back story.
Instead, I'm here to write about a second (much, much smaller) insurance carrier which--while they probably aren't likely to make a shocking announcement tomorrow morning like UHC did--has made an almost identical move when it comes to their insurance brokers. The following was forwarded to me, once again, by insurance broker Josh Dickerson:
November 19, 2015
Dear Valued Agent,
The 2016 Federal Exchange has introduced many healthcare benefit options to the Arizona market. With the rate increases, benefit changes and plans exiting the market, many Arizonans are looking for affordable healthcare coverage. As a result of these market conditions, Phoenix Choice has experienced robust enrollment, more quickly than expected.
Going into OEP, Phoenix Health Plans set enrollment targets, including a goal for a substantial proportion of the enrollments to come through the broker channel. As of November 19th, 2015 that goal has been met. In order to continue to provide high quality health coverage at an affordable price and to sustain our market position, we must make changes to our sales strategy and commission model.
After much consideration, Phoenix Health Plans, Inc. has made a difficult decision to discontinue Phoenix Choice broker commissions for new Marketplace enrollments as of November 19th, 2015. We will pay commission and renewals in accordance with the agent agreement for all Phoenix Choice applications received on or before November 19th, 2015. This decision does not impact commission payment for any of our plans in other states.
We appreciate your understanding and hope to continue to partner with you in the future. We also offer Medicare Advantage Plans in Arizona. If you are interested in selling our MAPD Plans, contact us about becoming contracted and certified. You can find the details at Phoenix Health Plans | Arizona Medicare Plans | Medicare Advantage Plans in Phoenix, AZ.
Sincerely,
Phoenix Health Plans
There's several things to digest here.
First of all, as far as I can tell, Phoenix Health Plans doesn't operate in any other states besides Arizona, unless they're owned by a larger holding company or something, so the "doesn't impact other states" part seems kind of weird.
Secondly, they're at least being more up front/forthright about the situation. Unlike the UHC broker letter, Phoenix is coming right out and laying it on the line: We've already hit our limit for broker-assisted enrollees, so no more soup for you; buzz off. The wording doesn't make it clear whether the "goal" which has been met only applies to broker-assisted enrollees specifically or to their total exchange enrollment target, but either way, they're cutting off the commission tap. UHC also didn't say anything about "meeting their goals" or enrollment being "robust, more quickly than expected"; they danced around with a lot of talk about "adjusting to market changes" and so on. Phoenix is stating point-blank: We hoped to enroll X people for 2016, we've enrolled X people already, that's that. They aren't "reducing" broker commissions, they're cutting them off completely for the year.
Third, the reference to "plans exiting the market" is a pretty clear reference to Arizona's Meritus Co-Op being yanked off of the exchange just 24 hours before Open Enrollment launched. Meritus is covering around 59,000 Arizonans for 2015 who have to find another carrier for next year.
My take is that Phoenix got flooded with a whole bunch of Meritus "refugees" (sorry, couldn't help myself) in the first 2 weeks of #OE3, decided they didn't want any more of them and are therefore winding down 2016 enrollment only 2 1/2 weeks into the season as a result.
There's also one other interesting thing about Phoenix Health Plans: According to RateReview.HealthCare.Gov, Phoenix is actually lowering their average premium rates by 16.6% for 2016.
I have no idea how many exchange enrollees Phoenix Health Plans has currently, but according to this redacted version of their 2016 filing , it looks like they were only expecting to enroll around 8,000 people (on average per month) next year:
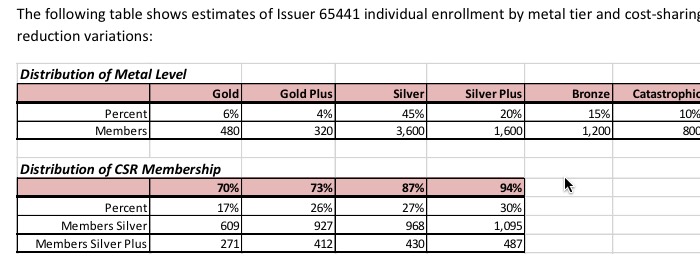
Arizona is on the federal exchange, which has confirmed that 1.08 million people selected policies as of 11/14, or around 12.2% of the total via HC.gov last year. They haven't broken that 1.08M out by state, but let's assume that the 38 states are proportionate. If so, that means Arizona should have enrolled roughly 25,000 people to date (12.2% of 205,666).
(For the record, according to the HC.gov Data site, the other 8 carriers on the exchange in Arizona are: Humana, Health Choice, Health Net, BCBS AZ, Aetna, Cigna, U of AZ and United Health One.)
OK, so let's assume that 25,000 Arizonans have already selected a plan for 2016. Who are the ones most likely to enroll in a new policy early? Why, the ones who are otherwise at risk of losing their coverage entirely, of course: The 59,000 or so on the failed Co-Op.
I'd be willing to bet that the vast majority of those 25K or so who've selected new plans are from the Meritus Co-Op...and assuming Phoenix's rates are fairly low relative to other carriers, the Meritus folks are probably pouncing all over Phoenix...which was only really anticipating taking on around 1/3 of that number signing up for the entire enrollment period (and that presumably includes their own current enrollees sticking around).
Anyway, I have no idea whether this is connected with the UHC situation, but the "no more commissions!" part sure sounds like it's from the same playbook. Like the movie producer character at the end of Barton Fink who insists on keeping Fink under contract but refuses to actually produce anything he writes, the exchange carriers are saying that they want to participate in the exchange...without letting anyone actually enroll beyond a certain threshold.



