Sanger-Katz: Significant rate hikes coming for real this time around.
Almost exactly 1 year ago over at healthinsurance.org, I posted the following:
May 15 officially marked the start of the 2016 rate review season. What that means for Americans is that over the next month or so, newspapers and web sites across the country will start running stories with scary-sounding headlines like this:
Some Oregonians could face major insurance rate hikes next year
Health plans request double-digit premium increases
… or, more reassuringly, like this:
Lower rate increases, more plans proposed for state’s health exchange in 2016
The articles will throw a bunch of numbers around, saying that the “average” premium rate increase for a given state is expected to be X percent, followed by examples of the highest and lowest increases. There may even be a few “Company Y will actually be reducing their rates!” thrown in.
Before you freak out, there are a few important things to look for.
I then went on to list several key caveats about the requested rate hike requests being released publicly:
- The "average" hikes have to be weighted by carrier market share (ie, if company A has 90% of the market and requests a 10% hike, while company B has 10% and requests a 50% hike, the average is not 30%, but 14%).
- The "average" hikes also have to be weighted by metal level/specific policy (ie, if a company requests a 20% hike on Gold plans but only 5% on Silver plans, but 90% of their enrollees are in the Silver plan anyway, the weighted average will be much closer to 5% than 20%).
- The percent hike isn't nearly as important as the actual dollar figure (ie, a 20% increase on a plan costing $300/month is still gonna cost less than a 5% hike on a plan costing $400/month).
- These are requested rate hikes, not approved (a carrier can ask for a 500% increase; that doesn't mean they're gonna get approved for it. Over the past two years, many state regulators made carriers reduce their rate increases significantly, or even lower their rates in some cases...although in other cases, they actually told the carriers to increase rates more than originally requested).
These factors and others had already been illustrated perfectly a year earlier:
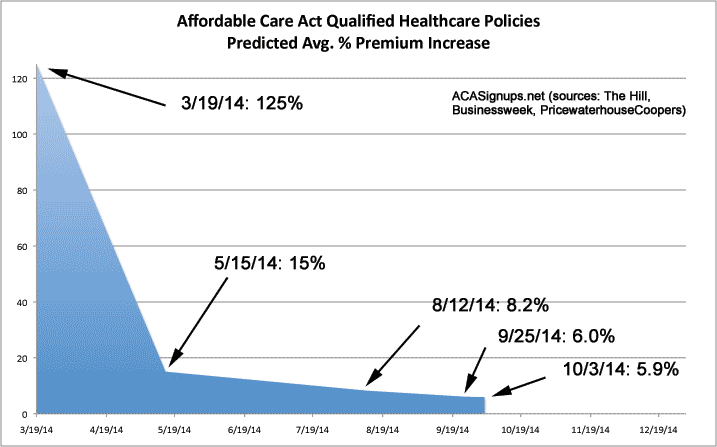
Hmmm. Somehow we've gone from "double to triple" increases in March (let's split the difference and go with a 125% increase projection) to "double digits" (let's call it 15%) in May to 8.2% in August to 6.0% in September to 5.9% last week.
Just for fun, I decided to chart this (hey, everyone likes charts, right?):
In the end, I believe the average 2015 individual market (full price) rate hike ended up being only around 5.5% or so.
Anyway, for 2016's rate hikes, I decided to be a bit more methodical. I peformed a whole bunch of research and number-crunching, and eventually concluded that the overall, weighted average rate hike nationally for the individual market would likely be roughly 12-13%. HOWEVER, I also added one more important point: The shop-around factor:
*IMPORTANT: This assumes that everyone currently enrolled sticks with their current policy next year. If enough people shop around and consider their options, the average premiums for various plans, various companies, in vartious states and nationally could end up being considerably lower (possibly coming in under 10% overall).
Sure enough, when the dust settled:
...During the Marketplaces’ annual Open Enrollment Period, new consumers select plans and current consumers have the option to switch plans. Overall, 6.4 million individuals (67 percent) of HealthCare.gov consumers selected a new plan for 2016: 4.0 million new consumers, plus 2.4 million (43 percent) of returning consumers. After taking into account shopping, the average premium among all HealthCare.gov consumers increased 8 percent from 2015 to 2016 (Table 1), not much higher than the 7.2 percent increase in the second-lowest silver plan premium reported at the start of the 2016 open enrollment. The 8 percent increase in the average premium after shopping demonstrates that enrollees’actual premiums depend on the dynamics of the entire market not just issuers’ pricing decisions.
Of course, for those receiving APTC assistance via the ACA exchanges, that average increase was even lower: Around 4% on average.
So...only around 5.5% in 2015, only 8% in 2016. Not fantastic, but much lower than the 10-12% average annual hikes prior to the ACA.
For 2017, however, it appears that the double-digit rate hikes really are gonna be back.
All of the caveats I wrote about last year remain the case. The final hikes more than likely won't be as bad as some of the headlines over the next month or so suggest.
HOWEVER, "not as bad as suggested" is a subjective thing. A 15% hike instead of a 30% hike is still a 15% hike.
With that in mind, Margot Sanger-Katz of the New York Times lowered the boom this morning:
Over the last few years, average premium increases in the Obamacare markets have been lower than the increases for people who bought their own insurance in premiums before the Affordable Care Act. But several trends are coming together that suggest that pattern will break when plan premiums are announced in early November. Many plans may increase prices by 10 percent, or more. Over the last two years, I’ve written articleswarning against scary headlines that exaggerate premium increases. Next year, those scary headlines are more likely to be accurate.
Peter Lee runs the country’s largest and most stable state marketplace, Covered California. The typical rate increase has been only 4 percent over the last two years. Next year will be different. “We expect our rates to go up more than that this year,” he said at a recent meeting with health reporters. He predicted “big rate increases” in other states.
Only two states have collected proposed rates for 2017 yet, but in both of them, popular carriers are asking for double-digit increases. Insurers don’t always get what they want, and there is local variation in insurance rates, but these early requests are in line with statements from insurance offiicals and regulators about what to expect.
Sanger-Katz goes on to break out three major reasons why rates will likely go up more than they did the first two years:
- Medical care is expected to cost more (in general; not ACA/Obamacare-related)
- Two of the "3 R's" (the programs put in place to help cushion the blow/smooth over cost spikes for insurance carriers) are being sunsetted at the end of 2016
- The carriers simply screwed up by under-pricing in the first place (either by mistake or in an ill-conceived attempt to snap up marketshare), and are now correcting for this
She also provides one important factor which should help mitigate the rate hikes:
As part of its spending deal late last year, Congress gave the insurance industry a big financial gift that should help drive down premiums. It temporarily eliminated a tax on health insurance premiums. The tax had been passed along to customers, as taxes usually are, in the form of higher prices. Experts claim that the savings should flow the other way — making price increases about 2 percent less than they would be otherwise.
I'll be keeping a close eye on the requested rate hike filings in all 50 states (+DC) just as I did last year; it might end up not being all that bad after all. However, assuming all the current indications prove to be accurate, I wouldn't be surprised to see a weighted requested average of perhaps 15-20% nationally for 2017, although that will hopefully end up being only in the 10-15% range once the dust settles (note that we won't know the actual effective average rate increases until next spring, after the 2017 Open Enrollment Period (OE4) is over).