UPDATE: CMS Medicaid Report: Expansion Finally Tapped Out? Net increase of 13.2M thru July
Every month the CMS division of the HHS Dept. issues a formal Medicaid/CHIP enrollment report, and pretty much every month (until now) the numbers have grown rapidly. This has been the case even during the "off-season", since there isn't an off season for Medicaid/CHIP enrollment; those eligible for the programs can enroll year-round (on the other hand, promotion/outreach efforts are higher during Open Enrollment, so enrollment does still tend to be more rapid during that period).
As of the end of June, this trend was still continuing: While not hitting the half-million plus rates of many earlier months, nearly 300,000 more people still signed up in June.
292,112 additional people were enrolled in June 2015 as compared to May 2015 in the 51 states that reported comparable June and May 2015 data.
However, with the King v. Burwell court case finally squared away (Medicaid/CHIP wouldn't have been directly impacted by an adverse ruling, but there was still tremendous amounts of media coverage about the ACA and low-income citizens, so I have to assume there was some residual impact), as the summer heat took hold, CMS's July report shows that additional Medicaid/CHIP enrollment has finally tapered off significantly:
- Over 72 million individuals were enrolled in Medicaid and CHIP in July 2015.7 This enrollment count is point-in-time (on the last day of the month) and includes all enrollees in the Medicaid and CHIP programs who are receiving a comprehensive benefit package.
- 28,524 additional people were enrolled in July 2015 as compared to June 2015 in the 51 states that reported comparable July and June 2015 data.
Yes, that's right: The net total number of Medicaid/CHIP enrollees went up fewer than 30,000 people in July.
It's worth noting that the improving economy may be a significant part of this. Remember that this is the net number of enrollees; for all I know, 300,000 new people joined the program but 270,000 who were already on it left. Baseline churn is tricky to keep track of.
However, the more likely cause is far simpler: ACA Medicaid expansion has simply finally maxed out in most of the states allowing it, and most of the "woodworker" crowd has presumably finally figured out that they're eligible as well.
For evidence of this, I need look no further than my own home state of Michigan. As of the end of March, the Wolverine state's "Healthy Michigan" program (aka, Medicaid expansion), which had been shooting quickly upwards for months, broke through the 600,000 enrollee mark.
- In early April, due to the baseline churn factor I noted above, it was 573,000.
- As of early July, the tally stood at...606,000.
- And as of yesterday (September 28th) it stood at...600,000.
In other words, the expansion program has finally hit 100% capacity in Michigan...and the same is true in many other states as well. Indiana didn't start their Expansion program until the end of January of this year and was already up to 290,000 as of July...83% of their estimated total eligible population. 206,000 have enrolled in New Mexico...21% more than estimated to be eligible, and so on.
As far as I can tell, the only way that Medicaid will continue to increase their enrollment numbers at this point will be for additional states to finally stop acting like children holding their breath until they turn blue and actually expand the program. Fortunately, there's some movement on this front:
- Alaska finally jumped on board the expansion program via the Governor's executive order; that could be goood for 40,000 people.
- South Dakota is in discussions to possibly do so as well, though still at an early stage; that could be up to 48,000.
- and in Utah, the last I heard, Governor Herbert had called for a Special Session of the state legislature regarding his version of the program; if approved, that could mean up to 50,000 new enrollees.
Of course, these are all tiny states, and two of the three haven't agreed to anything yet, but it's still a positive sign in my book.
Now if only Florida, Texas and/or North Carolina would jump on board...
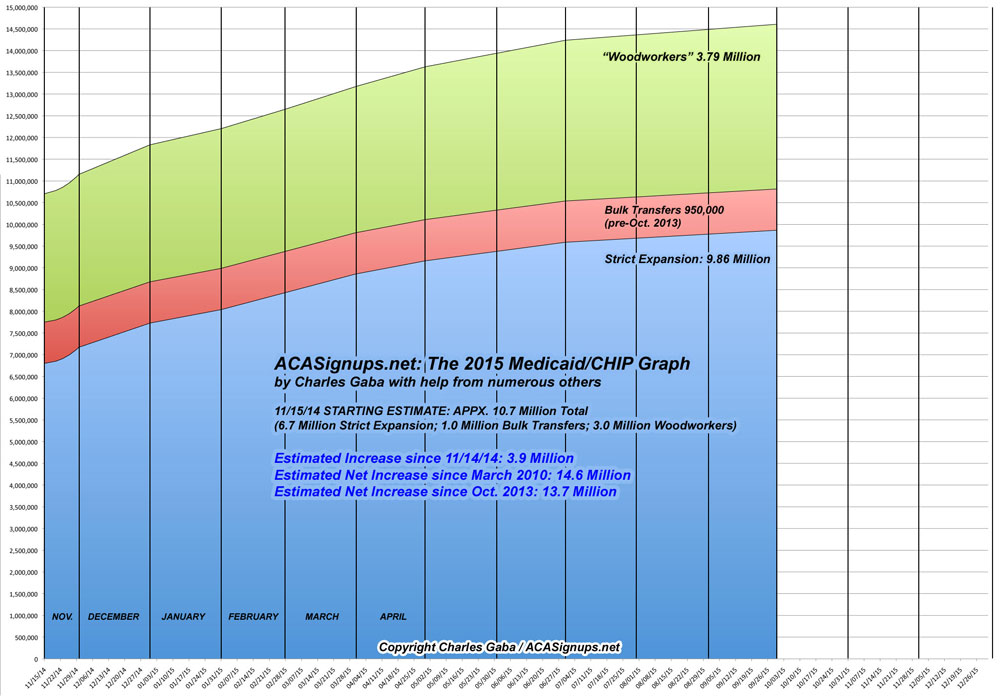
In any event, here's what Medicaid/CHIP growth looks like, including my own estimates of growth since July; as you can see, it's prettty much plateaued and likely now stands at around 13.7 million more than it did just before the ACA expansion started (click for higher-res version):
UPDATE: Thanks to Justin Hoca for bringing up two other factors which might lead to continued growth and/or less churn in Medicaid enrollment:
- First, as I noted in August, CMS has wisely decided to allow states to use SNAP (food stamp) data to automatically enroll & renew eligible Medicaid enrollees.
- Second, Hoca claims that earlier this year, CMS changed the rules on how renewals are handled, making it easier for current enrollees to "passively" renew without having to do anything (as long as they're still eligible). That should help with the churn issue; he's promised to see if he can hunt down a link about it.